Maternal Immune Activation and Neuropsychiatric Illness: A Translational Research Perspective
Abstract
Epidemiologic studies, including prospective birth cohort investigations, have implicated maternal immune activation in the etiology of neuropsychiatric disorders. Maternal infectious pathogens and inflammation are plausible risk factors for these outcomes and have been associated with schizophrenia, autism spectrum disorder, and bipolar disorder. Concurrent with epidemiologic research are animal models of prenatal immune activation, which have documented behavioral, neurochemical, neuroanatomic, and neurophysiologic disruptions that mirror phenotypes observed in these neuropsychiatric disorders. Epidemiologic studies of maternal immune activation offer the advantage of directly evaluating human populations but are limited in their ability to uncover pathogenic mechanisms. Animal models, on the other hand, are limited in their generalizability to psychiatric disorders but have made significant strides toward discovering causal relationships and biological pathways between maternal immune activation and neuropsychiatric phenotypes. Incorporating these risk factors in reverse translational animal models of maternal immune activation has yielded a wealth of data supporting the predictive potential of epidemiologic studies. To further enhance the translatability between epidemiology and basic science, the authors propose a complementary approach that includes deconstructing neuropsychiatric outcomes of maternal immune activation into key pathophysiologically defined phenotypes that are identifiable in humans and animals and that evaluate the interspecies concordance regarding interactions between maternal immune activation and genetic and epigenetic factors, including processes involving intergenerational disease transmission.
[AJP AT 175: Remembering Our Past As We Envision Our Future
October 1857: The Pathology of Insanity
J.C. Bucknill: “In the brain the state of inflammation itself either very quickly ceases or very soon causes death; but when it does cease it leaves behind it consequences which are frequently the causes of insanity, and the conditions of cerebral atrophy.” (Am J Psychiatry 1857; 14:172–193)]
Epidemiologic studies have repeatedly implicated prenatal environmental factors, including maternal immune activation, in the etiology of neuropsychiatric illnesses (1, 2). Maternal infectious pathogens and inflammation are plausible risk factors for these outcomes and have been associated with schizophrenia (1–3), autism spectrum disorder (4–11), and bipolar disorder (12, 13). Concurrent with epidemiologic studies are animal models of maternal immune activation that have documented behavioral, neurochemical, neuroanatomic, and neurophysiologic disruptions in offspring (14–17). The use of animal models in translational research aims to complement this work by establishing causal relationships, identifying cellular and molecular mechanisms, and exploring potential therapeutic interventions (14–17). Despite progress in addressing these issues, there remain challenges regarding how best to approach the bidirectional translation between the findings of epidemiologic and basic neuroscience studies of schizophrenia and other neuropsychiatric disorders.
The Epidemiologic Perspective
A proliferation of epidemiologic studies have implicated maternal infection as a risk factor for neuropsychiatric illness (1–13). Although early epidemiologic studies, which made use of ecologic data, suggested associations between influenza epidemics and schizophrenia among offspring exposed in utero, findings were inconsistent. Such studies have been supplanted in more recent years with birth cohort studies that use prospectively acquired serologic biomarkers of infection or inflammation in individual pregnancies. As discussed in the next section, an increasing number of published studies suggest associations between maternal infectious or inflammatory biomarkers and schizophrenia, autism spectrum disorder, and bipolar disorder (1, 2, 6, 14–16, 18). Other studies, which have used prospective data on maternal infection drawn from records on clinically diagnosed infections, have also yielded evidence in support of these exposures as risk factors (1, 6).
The Basic Science Perspective
Motivated by epidemiologic findings, a plethora of animal models of maternal immune activation have been established over the past two decades. As extensively reviewed elsewhere (14–17), one class of animal models is based on prenatal exposure to live pathogens, such as influenza virus (19–22) and Toxoplasma gondii (T. gondii). These models are particularly useful for the verification of causal relationships in epidemiologic studies that assess the role of specific infectious pathogens. Another class of animal models makes use of immune-activating agents that primarily stimulate the innate immune system, such as the bacterial endotoxin lipopolysaccharide and the synthetic double-stranded RNA analogue polyriboinosinic-polyribocytidylic acid (poly[I:C]) (14, 15, 17, 21, 23–25). These were developed initially to test whether imbalances in maternal or fetal cytokines may be critical to the association between prenatal infection and postnatal brain pathology (26, 27). An important refinement of this second class of models was the application of individual cytokines as immune-activating agents (9, 28, 29). This approach aims to address whether specific cytokines, or cytokine networks, mediate the association between maternal immune activation and neuropsychiatric illnesses. A third class of models is based on specific immunopathological processes that have been implicated in the etiology of neuropsychiatric illnesses. Two prominent examples of this class are animal models of maternal exposure to autism-related maternal autoantibodies (30–33) and allergic disorders and asthma (34–36).
The majority of current maternal immune activation models are based on maternal exposure to nonvirulent, immune-activating agents, such as the viral mimetic poly(I:C) (14–17, 37). Although this experimental approach offers some clear advantages (14–17, 37), it does not reproduce the full spectrum of immune responses normally induced by infectious pathogens. For example, this method falls short in stimulating pathogen-specific humoral and cellular immune reactions, which may be part of the mechanism mediating the negative effects of maternal infection on offspring. As discussed in detail elsewhere (37), one reason the field shifted from maternal immune activation models that are based on exposure to infectious pathogens is that they require stringent biosafety levels, which cannot be easily realized in many research laboratories. Another reason for the increasing popularity of nonvirulent immune-activating agents, such as poly(I:C), in maternal immune activation models is that they allow researchers in basic science to tightly control the intensity and duration of the (innate) maternal immune response. This, in turn, allows researchers to identify subthreshold and suprathreshold effects of maternal immune activation on brain and behavioral functions in offspring (24, 27) and to determine whether these are influenced by the precise gestational timing of this activation (38–42). Finally, maternal immune activation models that use nonvirulent immune-activating agents were initially developed with the aim of exploring whether the association between prenatal infection and neurodevelopmental abnormalities is mediated by specific infectious processes or, alternatively, by components of immune responses that are commonly triggered by various infections, including cytokine production (26, 27, 43). Although infection-triggered immune responses seem to be a crucial contributing factor to many associations (2, 15), it is unlikely that distinct pathogens mediate the negative effects of maternal infection on offspring through the same immune responses and pathophysiologic mechanisms (44). To fully appreciate and approach this complexity, we believe that the field would benefit from a revival and extension of experimental approaches that make use of prenatal exposure to distinct virulent and nonvirulent agents.
Another limitation of maternal immune activation models is that they typically exclude real-life influences in humans other than the primary exposure of interest. Additionally, this limitation may be one of the reasons the findings from animal models of maternal immune activation appear to be more robust in their effects on adult brain functions compared with the findings from epidemiologic studies that explore the association between markers of infection and risk of psychiatric disorders. In keeping with their artificial nature, the findings from animal models of maternal immune activation may be associated with their potential to provide data that cannot be derived from human studies. The recent finding that maternal segmented filamentous bacteria mediate the association between prenatal poly(I:C)-induced immune activation and autism-related brain abnormalities in mouse offspring (45) is a demonstrated example. Segmented filamentous bacteria are a family of autochthonous, apathogenic bacteria occurring in the ileum of rodents and other vertebrate species and have been shown to potently influence immune development and functions in mice (46). However, it remains controversial whether, and to what extent, these bacteria modulate the same immune parameters in humans (47–49).
The use of cross-species approaches in maternal immune activation models is one possible approach to minimizing the potential for overinterpreting or oversimplifying the findings obtained in a certain animal species or strain (50–57). Although the majority of these models have been developed in rodent species, most notably rats and mice, some have been extended to species that are evolutionarily and ethologically closer to humans, including rhesus monkeys (8, 50, 55, 56). Whereas rodents are separated evolutionarily from humans by more than 70 million years, rhesus monkeys diverged from human evolution approximately 25 million years ago and thus exhibit greater similarity to humans in terms of genetics, immunology, neurobiology, and behavior (57, 58). Compared with rodents, rhesus monkeys are also more comparable to humans in their placental physiology, gestational timelines, pre- and postnatal brain development, and cortical architecture (57, 58). Thus, the inclusion of species that are more similar genetically to humans, such as the rhesus monkey, can aid in interpreting the outputs of rodent maternal immune activation models in terms of what they might mean for pathological symptoms in humans (51–54), thereby enhancing the cross-species transfer of information and translatability to the clinical condition in humans (57, 58).
Findings From Maternal Immune Activation Studies of Neuropsychiatric Outcomes and Relatedness of Findings Between Epidemiology and Basic Science
A key question is how the findings from the disciplines of epidemiology and basic science can complement and inform one another in furthering our understanding of the role of maternal immune activation in neuropsychiatric outcomes. In particular, we consider reverse translational approaches to this question, that is, whether human findings on maternal infection can predict parallel findings in experimental model systems. We first consider the parallels between the findings in epidemiologic and animal studies for schizophrenia, bipolar disorder, and autism spectrum disorder. Because a full review of the findings of maternal immune activation and neuropsychiatric outcomes is beyond the scope of this article, we highlight some key results and refer the reader to several comprehensive reviews (1, 2, 6, 14–18). Below, we focus on the potential areas of concordance between epidemiologic and basic science studies for each of these disorders.
Schizophrenia
To date, maternal immune activation and offspring psychiatric outcomes have been most commonly investigated for schizophrenia. We focus here on selected findings that are based on biomarkers of infection. Although not all findings have been replicated, key epidemiologic results include associations between maternal infectious pathogens (i.e., influenza virus, herpes simplex virus [HSV], T. gondii, rubella, and bacterial pathogens) and inflammatory biomarkers (i.e., cytokines and C-reactive protein) and schizophrenia (1, 59). Maternal exposure to influenza during early to mid-gestation, as quantified by antibody in maternal sera, was associated with a threefold increased risk of schizophrenia in the Child Health and Development Study (CHDS), which was based on a large birth cohort in northern California (3). An elevated maternal T. gondii IgG level was associated with a twofold elevation in schizophrenia risk in this same birth cohort (60), and maternal genital and reproductive infections were associated with schizophrenia in this cohort (61). Maternal exposure to HSV-2 was associated with nonaffective and affective psychoses in the National Collaborative Perinatal Project (62) but not in the birth cohorts of the CHDS or of the Finnish Prenatal Studies, which is based on a large national birth cohort in Finland (63). Neonatal antibodies to T. gondii and cytomegalovirus have been associated with nonaffective psychosis in adulthood (64). In our study of maternal cytokines in the CHDS, we observed that increased interleukin-8 was related to schizophrenia (65). In the Finnish Prenatal Studies, we found that maternal C-reactive protein, a nonspecific biomarker of inflammation, was associated with an increased risk of schizophrenia (59). Because it is unlikely that associations between biomarkers of inflammation are accounted for by one or a small group of infections, these findings may point to a common pathogenic pathway by which different infections give rise to schizophrenia.
Since their initial establishment, animal models of maternal immune activation have repeatedly documented structural and functional phenotypes that are implicated in schizophrenia and related psychotic disorders (2, 14–17). On the basis of early epidemiologic findings on maternal influenza and schizophrenia (1), Fatemi et al. (19–22, 27) pioneered an experimental mouse model of prenatal exposure to human influenza virus in mice. As reviewed elsewhere (14, 15), maternal influenza infection in mice led to a variety of behavioral, neurochemical, morphological, and transcriptional changes in the offspring, many of which are implicated in schizophrenia and related disorders. These findings are thus strongly related to, and provide experimental support for, the association between maternal influenza infection and risk of schizophrenia (1, 3, 63). Since then, many additional investigations based on reverse translational animal models of maternal immune activation have yielded a wealth of new data supporting the predictive potential of epidemiologic studies. For example, deficits in sensorimotor gating, impairments in selective or sustained attention, deficiencies in working memory, and hyperresponsiveness to psychotomimetic drugs have been found in various rodent models of maternal immune activation, including prenatal exposure to influenza virus, the viral mimetic poly(I:C), the bacterial endotoxin lipopolysaccharide, and selected inflammatory cytokines (14–17). Some of these deficits show a maturational delay in their appearance and can be mitigated by symptomatic or preventive treatments with antipsychotic medications (14–17).
Notably, the fact that prenatal exposure to various immune-activating agents can elicit similar phenotypes is consistent with epidemiologic findings suggesting that the association between maternal immune activation and schizophrenia is not limited to a single infectious or inflammatory condition (1, 15). Despite the similarities between maternal immune activation models, however, there are also some notable differences between the models with respect to the nature of brain and behavioral changes. For example, whereas prenatal poly(I:C) exposure in rats and mice has been shown to induce cellular, neurochemical, and behavioral phenotypes that are characteristic of a hyperdopaminergic state (23, 66, 67), prenatal lipopolysaccharide exposure may instead induce a hypodopaminergic state in adult rodent offspring (68). Prenatal lipopolysaccharide exposure in the rhesus monkey was found to cause a significant increase in global white matter volume (50), whereas an opposite pattern (i.e., decreased white matter volume) was observed in rhesus monkey offspring born to mothers infected with influenza (55). Besides the notable influence of prenatal timing and the genetic background discussed above, such differences may arise because different immunogens can induce a distinct set of neuroimmune abnormalities across brain development and, consequently, may lead to differing long-term deficits in brain structure and function. This notion would also be consistent with epidemiologic findings that appear to suggest that not all infectious pathogens have the same potential to increase neuropsychiatric disease risk (1, 13). As discussed more extensively later, a closer examination of the commonalities and differences between the mediating factors and outcomes of distinct maternal immune activation models should help to further address this important issue.
Another question is whether animal models can also predict certain epidemiologic associations. Although comparatively little work has been done, our more recent findings support this assertion (69). We developed an environmental two-hit model in mice, in which prenatal exposure to mild but physiologically relevant maternal immune activation served as the first hit, and subchronic exposure to unpredictable psychological stressors in pubescence served as the second hit (69). Hence, this multifactorial model incorporates two environmental risk factors that have each been associated with increased risk of psychiatric disorders such as schizophrenia. We showed that combined exposure to the two environmental adversities acted in synergy to induce psychosis-related neural and behavioral abnormalities in adult mice (69). These results provided the first evidence, to our knowledge, suggesting that prenatal immune adversities can function as a neurodevelopmental disease primer, which in turn can increase the offspring’s vulnerability to the detrimental neuropathological effects of subsequent stress exposure during pubescence (69). These basic science findings have recently been translated to a large population-based epidemiologic study, which comprised nearly 1 million Danish persons born between 1980 and 1998 (70). In that study, Danish nationwide registers were linked to estimate the independent and joint effects of exposure to prenatal infection and peripubertal psychological trauma on the risk of schizophrenia. Prenatal exposure to infection was defined on the basis of records of hospital admissions with an infection during pregnancy, and exposure to traumatizing experiences during peripuberty (ages 8 to 14 years) was defined according to Danish standards and included parental death, maltreatment or physical or sexual abuse, and maternal and paternal occupational situation and history of crime. Confirming the hypothesis initially put forward by the environmental two-hit model in mice (69), the Danish study demonstrated that exposure to prenatal infection and peripubertal psychological trauma was associated with a significantly higher risk of developing schizophrenia (among males) compared with exposure to either insult alone, and the interaction between infection and trauma attained statistical significance (70). These findings suggest that the cross-fertilization between basic research in animals and risk factor epidemiology may offer the potential for predicting yet undiscovered associations between maternal immune activation and neuropsychiatric illnesses.
Bipolar Disorder
To date, only a few epidemiologic studies have evaluated maternal immune activation associated with bipolar disorder in offspring. Our group has demonstrated that maternal influenza, documented by antibodies in prenatal sera (59) and physician diagnoses (71), is associated with a fivefold increased risk of bipolar disorder. Although most other studies suggest no association between maternal infectious pathogens and bipolar disorder (13), one study found that maternal exposure to the type 1 strain of T. gondii was related to an increased risk of affective psychoses in offspring, which includes bipolar disorder (72).
Even though animal models of maternal immune activation have not been specifically explored for their validity for bipolar disorder, some of the experimentally induced phenotypes may be relevant for this neuropsychiatric illness as well. For example, deficits in sensorimotor gating, as seen in various rodent maternal immune activation models (2, 14–17), are also present in patients with acutely manic (73) and remitted bipolar disorder (74). Moreover, several animal studies have reported the emergence of depression-like behaviors in offspring exposed to maternal immune activation (75, 76). The latter phenotypes may be relevant not only for unipolar depression but also for depressive episodes in bipolar disorder. The investigation of other core behavioral symptoms of bipolar disorder, such as poor decision making, altered risk-taking behavior, impulsivity, and loss of inhibitory control, remain unexplored in maternal immune activation models. Additional work is necessary to evaluate whether maternal immune activation–induced deficits can be mitigated by pharmacological treatments used in bipolar disorder, including the mood stabilizer lithium and anticonvulsants such as valproate and lamotrigine (77).
Autism
In recent years, maternal infection and inflammation have been investigated in relation to autism spectrum disorder. Although findings are mixed and more work is necessary, evidence has emerged linking maternal inflammation to the risk of autism spectrum disorder in offspring. In the Finnish Prenatal Studies birth cohort, our group demonstrated that elevated maternal levels of C-reactive protein, a nonspecific biomarker of inflammation, in early to mid-gestation was related to an increased risk of autism spectrum disorder in offspring (4). However, in the Early Markers for Autism study conducted in northern California, maternal mid-pregnancy levels of C-reactive protein were related to a decreased risk of autism spectrum disorder (78). Examination of cytokines and chemokines in archived maternal serum samples in the Early Markers for Autism study demonstrated that significantly increased levels of these analytes were related to autism spectrum disorder (5, 11). In amniotic fluid samples from a Danish study, several cytokines, including tumor necrosis factor-alpha, and several inflammatory interleukins were related to autism spectrum disorder in offspring (7). Moreover, maternal fever has been associated with autism. Although replication of these findings is necessary, they suggest that maternal immune activation may be related to autism spectrum disorder. Consistent with this interpretation, other maternal immune factors, including maternal autoantibodies targeting fetal proteins, have been associated with increased risk of autism spectrum disorder in offspring (for a review, see reference 79). These findings include significant associations between paired maternal antibody reactivity to fetal brain proteins with the 37-kDa and 73-kDa molecular weight bands and diagnosis of autism spectrum disorder in children (80). Within proteins corresponding to the 37-kDa, 39-kDa, and 73-kDa bands, maternal autoantibodies recognized seven developmentally regulated proteins in the fetal brain, including lactate dehydrogenase A and B, stress-induced phosphoprotein 1, and collapsin response mediator proteins 1 and 2 (79, 80). Several of these proteins are critical for normal brain development, including neuronal migration and neural network formation.
Animal models further support the hypothesis that maternal immune activation is an environmental risk factor for autism spectrum disorder. For example, prenatal exposure to the viral mimetic poly(I:C), the bacterial endotoxin lipopolysaccharide, or allergies and asthma can all induce behavioral abnormalities that are reminiscent of core symptoms of autism spectrum disorder, including deficits in social interaction and communication and high levels of repetitive behaviors (9, 15, 34, 81). These manipulations also cause brain morphological and cellular abnormalities implicated in autism spectrum disorder, including abnormal cerebellar development, impaired expression of the extracellular matrix protein reelin, and altered synapse density and neural connectivity (2, 15, 21). Notably, some of these rodent findings have been extended to rhesus monkeys, both at the behavioral and brain morphological levels (8, 50, 56, 82).
Future Research
Broadening the Concepts to the Study of Maternal Immune Activation and Pathophysiologically Defined Phenotypes
One key unanswered question is whether there are particular factors that account for differences in psychiatric outcomes following maternal immune activation. There do not seem to be clear differences between these disorders in the gestational timing of maternal immune activation, although larger sample sizes are needed given the reduction in statistical power that results from stratification of analyses by periods of pregnancy. Similarly, the data are insufficient to permit comparisons between disorders of the effects of individual maternal infections, and there is a lack of information on the intensity of the immune response.
Although the study of the interaction of maternal immune activation with parental or offspring genes that cluster with particular disorders is a promising research direction, only a few studies of maternal immune activation, discussed later, have evaluated possible gene-by-environment interactions, and, to our knowledge, none have compared such interactions between different disorders.
Although there is clear merit in conducting such comparisons, our view is that the above question could be addressed more effectively by asking how the field might move from the study of maternal immune activation and specific psychiatric outcomes to improving our understanding of the connections this risk factor has to key elements of these disorders. One approach is to deconstruct the psychiatric outcomes into their essential psychopathological and neuropathological components. This approach is conceptually closer to research on maternal immune activation in animal models and thus appears more likely to maximize the extent to which findings in animal models can be translated to humans, and back-translated to animals (Figure 1), and advance the field by opening new avenues for the discovery of novel etiopathogenic factors and pathways. In this regard, animal models of maternal immune activation will be key in identifying neurobiological pathways leading to discrete pathological outcomes that may (or may not) cross current diagnostic boundaries.
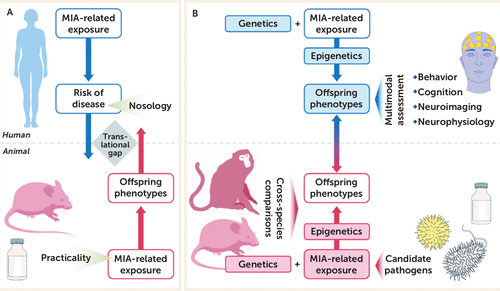
FIGURE 1. Contribution of Epidemiologic and Basic Science Studies to Translational Research of Maternal Immune Activation (MIA) in Neuropsychiatric Disordersa
a Panel A is a schematic illustration of the prevailing research approaches in epidemiology and basic science. With a few exceptions, epidemiologic studies of maternal immune activation generally aim to establish associations between infectious, inflammatory, or other immune exposures and risk of certain neuropsychiatric disorders, the latter of which are defined by the current nosologic system. On the other hand, most animal models of maternal immune activation are single-factor models, in which the isolated effects of maternal immune activation-related exposures are investigated with respect to behavioral, cognitive, neuroimaging, and neurophysiologic phenotypes in the offspring. For practical reasons, these models are often implemented in rodent species and are based on artificial immune-activating agents (e.g., synthetic double-stranded RNA) that do not require stringent biosafety precautions. The outcome of these epidemiologic and basic science approaches is often a lack of analogy, resulting in a translational gap that can undermine their translational validity. Panel B is a schematic illustration of epidemiologic and basic science approaches that can maximize the bidirectional translational validity through the modification of research concepts and the addition of supplementary research modules. In these alternative approaches, the objective of assessing maternal immune activation exposure disease-risk associations in epidemiologic designs is complemented or even replaced by 1) attempts to explore the effects of maternal immune activation on specific behavioral, cognitive, neuroimaging, and neurophysiologic phenotypes, which are free of nosologic constraints; 2) the concomitant study of genetic and epigenetic factors; and 3) the establishment of multifactorial animal models that incorporate genetic or epigenetic risk factors and maternal immune activation-related exposures that involve epidemiologically established infectious pathogens and other immune factors, such as inflammatory mediators. In addition, cross-species comparisons involving animal species with advanced cortical development will further enhance the bidirectional translatability between epidemiologic and basic science studies.
Here, we illustrate this with the example of schizophrenia. Cognitive and neuroimaging anomalies are key components of the phenotype of schizophrenia (83) and are also amenable to modeling in animals. To date, however, only a few studies have attempted to determine whether exposure to maternal immune activation confers vulnerability to these and other phenotypic characteristics of schizophrenia. In the CHDS birth cohort, we demonstrated that maternal exposure to infection (i.e., influenza and toxoplasmosis) was associated with impairments in executive functions, including abnormalities in cognitive set-shifting ability on the Wisconsin Card Sorting Test and disruptions in performance on the Trail-Making Test, Part B (84). Elevated maternal levels of interleukin-8, which were associated with risk of schizophrenia in this cohort, were also related to ventricular enlargement (85). Notably, similar phenotypes, including impairments in executive functions and ventricular enlargement, have been observed in adult rats and mice exposed to maternal immune activation (2, 14, 15, 86–91), suggesting that there is bidirectional translational validity between the outcomes in the animal model and the epidemiologic or clinical condition.
The application of more systematic methods of classification of outcomes that are based on phenotypes that are biologically relevant (92) to maternal immune activation models may offer further promise: the studies reviewed above suggest that this exposure alters neurobiological and behavioral functions that cannot be simply mapped onto a particular diagnostic phenotype. Parenthetically, prenatal exposure to infectious or inflammatory adversity may be viewed as a general vulnerability factor for developmental disturbances rather than a disease-specific risk factor. This view is compatible with the Research Domain Criteria system, which capitalizes on biological determinism to explain the pathogenesis of distinct psychiatric symptoms and focuses on endophenotypes rather than nosologic entities (92). Shifting the research focus to classification of neurobiological outcomes rather than nosologic entities likely minimizes strict disease-to-model correspondence, a major challenge for translational studies (Figure 1).
The potential to realize these research aims exists. Several existing large population-based birth cohorts with biospecimens and data on early development have been linked to national databases on psychiatric outcomes (59, 93, 94). Study subjects from these cohorts have the potential to be located through national registries and followed up for neurobiological outcomes, and biomarkers of maternal infection and inflammation have already been assessed in the mothers of case subjects and matched control subjects from these cohorts. Given their translational value, the findings from animal models of maternal immune activation could facilitate the selection of biobehavioral outcomes to be investigated in corresponding human epidemiologic studies.
Conducting such research in prospective birth cohort studies, however, requires either long follow-up intervals or identification of a sample of case subjects who belonged to a birth cohort. Given the relatively rare outcome, the limitations inherent to such research include loss to follow-up with consequent bias and small sample sizes. One potential solution to this problem is exemplified by a recent study of maternal and childhood micronutrient supplementation (95). In that study, pregnant mothers and their neonates received supplementation with phosphatidylcholine (aimed to deliver choline to the offspring’s brain), and the offspring received neurophysiologic testing of sensorimotor gating during infancy and of neurocognition during childhood. Compared with offspring who were not in the supplementation group, children in the phosphatidylcholine supplementation group had an increased likelihood of normal inhibition of the P50 auditory evoked response, a biomarker of improved sensorimotor gating, and fewer attention problems and social withdrawal in early childhood (95). The P50 auditory evoked response is mediated by a specific cholinergic receptor, the α7-nicotinic acetylcholine receptor, which is encoded by the CHRNA7 gene. These findings were also recapitulated in a mouse model, in which choline supplementation of wild-type mice led to improvement in sensory inhibition of this auditory evoked response, whereas no beneficial effects were observed in mice that were heterozygous or mutant for the CHRNA7 gene (96).
Transdisciplinary Approaches for Advancing the Understanding of the Role of Genetics and Epigenetics in the Context of Maternal Immune Activation
Several genes identified from genome-wide association studies, including those within the major histocompatibility complex locus (97) and complement C4 (98), encode proteins that play important roles in immune functioning and in neurodevelopment. With the exception of rare copy number variants (99, 100), mutations in these and other individual genes are generally associated with relatively small increases in the odds of psychiatric outcomes, such as schizophrenia (101) and autism spectrum disorder (102), but are hypothesized to confer larger disease susceptibility by interacting with environmental exposures, such as maternal immune activation. It is noteworthy that the assessment of environmental exposures is sometimes required to detect genetic effects, as demonstrated, for example, by the findings of a genome-wide study of association and interaction with maternal cytomegalovirus infection (103) and a study that showed an interaction between maternal pyelonephritis and family history of psychosis (104). Hence, environmental factors, such as maternal immune activation, may unmask the (statistical and biological) significance of certain genetic variations.
Recently, Mendelian randomization approaches, combined with genome-wide association studies, have been used to interrogate the genetic architecture of biomarkers of inflammation and infection. In one study, summary association results from large consortia of candidate gene and genome-wide association studies were included in concert with Mendelian randomization methods to evaluate associations between the soluble interleukin-6 receptor, levels of C-reactive protein, and schizophrenia (105). The findings revealed a protective effect of C-reactive protein and a risk-increasing effect of soluble interleukin-6 receptor on schizophrenia risk, possibly accounted for by early-life infection. Although this study was conducted in (mostly) nonpregnant adults, it provides proof of concept for the use of measures of the genetic architecture of response to infectious agents in the mother as a proxy for risk to the offspring after maternal infection. Although Mendelian randomization studies are not without limitations, this work has the potential to investigate maternal immune activation in neuropsychiatric disorders in birth cohorts in which only information on candidate genes, but not maternal infection, are available. This approach could be broadly applicable to many cohorts, because prospective data on infections during pregnancy are not widely ascertained, whereas genetic markers can be assessed using biospecimens that are more readily obtainable. Studies that use Mendelian randomization methods coupled with genome-wide association studies to explore the role of infection in triggering autoimmune disorders and inflammation, combined with evaluation of shared genetic variance for autoimmune disorders in separate cohorts, offer further promise.
To date, however, few epidemiologic studies have conducted a thorough evaluation of risk genes in relation to maternal immune activation in studies of neuropsychiatric outcomes (103). A major reason is that such studies require availability of DNA and a measure of maternal infection or inflammation during pregnancy and follow-up of the offspring for the neuropsychiatric outcomes as well as large sample sizes, given that studies of gene-by-environment interaction generally require greater statistical power. The integration and evaluation of putative risk genes in animal models of maternal immune activation may offer a complementary approach to the investigation of gene-by-environment interactions in human studies (Figure 1). This has been a fruitful strategy for unraveling interactions between maternal immune activation and selected risk genes of neuropsychiatric illnesses (106), including CHRNA7 (107), disrupted-in-schizophrenia 1 (DISC1) (108, 109), neuregulin 1 (NRG1) (110), and Nurr1 (NR4A2) (111). Apart from providing evidence for additive effects on brain and behavioral abnormalities resembling aspects of major mental illnesses, these basic science studies show that prenatal immune activation can interact with selected risk genes to produce novel neurobehavioral phenotypes that are not apparent in animals harboring the genetic variant alone (106). For example, while mutations in the dopamine-related transcription factor Nurr1 and poly(I:C)-induced maternal immune activation in mice exert additive effects on locomotor hyperactivity and sensorimotor gating deficits, the combination of the two is required to impair attentional shifting and sustained attention (111). Similarly, the combination of mild maternal immune activation (induced by subthreshold doses of poly[I:C]) and mutations in DISC1 is necessary to impair social interaction in adult mouse offspring (108, 109).
Transdisciplinary approaches involving epidemiology and basic science may also advance our understanding of the role of epigenetics in the context of maternal immune activation. Epigenetic factors, defined as nonheritable alterations in the genome, are becoming increasingly recognized in the etiology of neuropsychiatric disorders (36, 112, 113). It has already been demonstrated that prenatal environmental factors, such as smoking (114), are linked to epigenetic alterations and to psychiatric disorders. In addition, advanced paternal age has been related to an increased rate of de novo mutations (115) and to autism (116) and schizophrenia (117) and may have transgenerational effects (116). Although maternal immune activation has not been examined to date in relation to epigenetic effects and de novo mutations in human populations, research in animal models suggests that epigenetic modifications may be a critical molecular mechanism by which maternal immune activation can mediate changes in brain development and function (36, 112, 118–122). Lasting epigenetic changes in response to maternal immune activation have been identified in various brain areas, including cortical and subcortical regions (36, 119–121), and in specific cell types, such as microglia (36). Furthermore, using the maternal poly(I:C) administration model in mice, we recently provided the first evidence showing that maternal immune activation–induced behavioral abnormalities and whole-genome transcriptional changes can be transmitted across generations without additional immune exposures (122). These transgenerational effects were mediated via the paternal but not maternal lineage and were present for at least three generations, pointing toward epigenetic inheritance via male gametes. Further studies on the identification of epigenetic and transgenerational effects in maternal immune activation–induced neurodevelopmental disorders may help to identify complex patterns of transgenerational disease transmission beyond genetic inheritance. Conceivably, the consideration of ancestral histories of infection may be a useful approach toward developing new preventive treatment strategies against infection-mediated neurodevelopmental disorders.
Implications of Research in Maternal Immune Activation for Health Policy and Prevention
The work reviewed in this article has the potential for significant impact on future health policy and prevention. Many infectious agents are preventable with relatively straightforward public health measures (123). In research conducted by our group, we estimated that the population attributable risk for schizophrenia after exposure to three maternal infections (influenza, T. gondii, and genital reproductive infections) was 30% in the CHDS birth cohort, suggesting that the proportion of cases in this population that would be preventable by elimination of these infections from the population could be as much as one-third (1, 123). T. gondii can be prevented by the use of simple hygienic measures, such as the use of gloves when gardening or cleaning cat litter boxes, adequate cooking of meat before consumption, and washing kitchen knives after cutting meats and produce (124). The occurrence of many sexually transmitted infections can be reduced by the use of barrier contraceptives, antimicrobials, educational programs to promote safe sex, the delay of first sexual contacts, and partner notification (125, 126). Maternal immunization during pregnancy is another health policy option with potential ramifications for prevention of neuropsychiatric disorders. Influenza vaccination is a mainstay for the prevention of the influenza virus, although it does not always provide complete protection (127). These measures are scalable to large populations given their relatively low cost and practicality. Most influenza vaccines do not appear to be related to significant risk for maternal, fetal, or neonatal complications when administered to pregnant women (128–131), and several health organizations recommend prophylactic influenza vaccination for this population (128).
Conclusions
Accumulating evidence suggests that maternal exposure to infectious and inflammatory insults is related to the etiology of major neuropsychiatric illnesses. The bidirectional translation of epidemiologic studies to basic neuroscience studies offers the promise of developing a more complete and nuanced understanding of maternal immune activation in relation to biological mechanisms. We suggest that further studies be conducted with the aim of capitalizing on the integration of these disciplines, particularly in relation to pathophysiologic entities that transcend diagnostic boundaries, and to assess multifactorial models, including genetic and epigenetic factors, in maternal immune activation-induced psychopathology.
1 : Prenatal infection and schizophrenia: a review of epidemiologic and translational studies. Am J Psychiatry 2010; 167:261–280Link, Google Scholar
2 : Maternal immune activation: implications for neuropsychiatric disorders. Science 2016; 353:772–777Crossref, Medline, Google Scholar
3 : Serologic evidence of prenatal influenza in the etiology of schizophrenia. Arch Gen Psychiatry 2004; 61:774–780Crossref, Medline, Google Scholar
4 : Elevated maternal C-reactive protein and autism in a national birth cohort. Mol Psychiatry 2014; 19:259–264Crossref, Medline, Google Scholar
5 : Autism with intellectual disability is associated with increased levels of maternal cytokines and chemokines during gestation. Mol Psychiatry 2017; 22:273–279Crossref, Medline, Google Scholar
6 : Maternal infection during pregnancy and risk of autism spectrum disorders: a systematic review and meta-analysis. Brain Behav Immun 2016; 58:165–172Crossref, Medline, Google Scholar
7 : Amniotic fluid chemokines and autism spectrum disorders: an exploratory study utilizing a Danish Historic Birth Cohort. Brain Behav Immun 2012; 26:170–176Crossref, Medline, Google Scholar
8 : Maternal antibodies from mothers of children with autism alter brain growth and social behavior development in the rhesus monkey. Transl Psychiatry 2013; 3:e278Crossref, Medline, Google Scholar
9 : The maternal interleukin-17a pathway in mice promotes autism-like phenotypes in offspring. Science 2016; 351:933–939Crossref, Medline, Google Scholar
10 : Association between influenza infection and vaccination during pregnancy and risk of autism spectrum disorder. JAMA Pediatr 2017; 171:e163609Crossref, Medline, Google Scholar
11 : Increased midgestational IFN-γ, IL-4 and IL-5 in women bearing a child with autism: a case-control study. Mol Autism 2011; 2:13Crossref, Medline, Google Scholar
12 : Serological documentation of maternal influenza exposure and bipolar disorder in adult offspring. Am J Psychiatry 2014; 171:557–563Link, Google Scholar
13 : The Kraepelinian dichotomy from the perspective of prenatal infectious and immunologic insults. Schizophr Bull 2015; 41:786–791Crossref, Medline, Google Scholar
14 : Prenatal poly(I:C) exposure and other developmental immune activation models in rodent systems. Biol Psychiatry 2014; 75:307–315Crossref, Medline, Google Scholar
15 : In-vivo rodent models for the experimental investigation of prenatal immune activation effects in neurodevelopmental brain disorders. Neurosci Biobehav Rev 2009; 33:1061–1079Crossref, Medline, Google Scholar
16 : Prenatal and postnatal animal models of immune activation: relevance to a range of neurodevelopmental disorders. Dev Neurobiol 2012; 72:1335–1348Crossref, Medline, Google Scholar
17 : Epidemiology-driven neurodevelopmental animal models of schizophrenia. Prog Neurobiol 2010; 90:285–326Crossref, Medline, Google Scholar
18 : Infectious and immunogenetic factors in bipolar disorder. Acta Psychiatr Scand 2017; 136:409–423Crossref, Medline, Google Scholar
19 : Defective corticogenesis and reduction in Reelin immunoreactivity in cortex and hippocampus of prenatally infected neonatal mice. Mol Psychiatry 1999; 4:145–154Crossref, Medline, Google Scholar
20 : Maternal infection leads to abnormal gene regulation and brain atrophy in mouse offspring: implications for genesis of neurodevelopmental disorders. Schizophr Res 2008; 99:56–70Crossref, Medline, Google Scholar
21 : Activation of the maternal immune system alters cerebellar development in the offspring. Brain Behav Immun 2009; 23:116–123Crossref, Medline, Google Scholar
22 : The viral theory of schizophrenia revisited: abnormal placental gene expression and structural changes with lack of evidence for H1N1 viral presence in placentae of infected mice or brains of exposed offspring. Neuropharmacology 2012; 62:1290–1298Crossref, Medline, Google Scholar
23 : Immune activation during pregnancy in rats leads to a postpubertal emergence of disrupted latent inhibition, dopaminergic hyperfunction, and altered limbic morphology in the offspring: a novel neurodevelopmental model of schizophrenia. Neuropsychopharmacology 2003; 28:1778–1789Crossref, Medline, Google Scholar
24 : Towards an immuno-precipitated neurodevelopmental animal model of schizophrenia. Neurosci Biobehav Rev 2005; 29:913–947Crossref, Medline, Google Scholar
25 : Ontogeny of sensorimotor gating and immune impairment induced by prenatal immune challenge in rats: implications for the etiopathology of schizophrenia. Mol Psychiatry 2010; 15:372–383Crossref, Medline, Google Scholar
26 : Exposure to infection and brain development: cytokines in the pathogenesis of schizophrenia. Schizophr Res 1997; 24:365–367Crossref, Medline, Google Scholar
27 : Maternal influenza infection causes marked behavioral and pharmacological changes in the offspring. J Neurosci 2003; 23:297–302Crossref, Medline, Google Scholar
28 : Maternal immune activation alters fetal brain development through interleukin-6. J Neurosci 2007; 27:10695–10702Crossref, Medline, Google Scholar
29 : IL-1 receptor antagonist protects against placental and neurodevelopmental defects induced by maternal inflammation. J Immunol 2010; 184:3997–4005Crossref, Medline, Google Scholar
30 : Prenatal exposure to autism-specific maternal autoantibodies alters proliferation of cortical neural precursor cells, enlarges brain, and increases neuronal size in adult animals. Cereb Cortex 2016; 26:374–383Crossref, Medline, Google Scholar
31 : Behavioral correlates of maternal antibody status among children with autism. J Autism Dev Disord 2012; 42:1435–1445Crossref, Medline, Google Scholar
32 : Maternal autism-associated IgG antibodies delay development and produce anxiety in a mouse gestational transfer model. J Neuroimmunol 2012; 252:56–65Crossref, Medline, Google Scholar
33 : Stereotypies and hyperactivity in rhesus monkeys exposed to IgG from mothers of children with autism. Brain Behav Immun 2008; 22:806–816Crossref, Medline, Google Scholar
34 : Behavioral impact of maternal allergic-asthma in two genetically distinct mouse strains. Brain Behav Immun 2017; 63:99–107Crossref, Medline, Google Scholar
35 : Allergic fetal priming leads to developmental, behavioral and neurobiological changes in mice. Transl Psychiatry 2015; 5:e543Crossref, Medline, Google Scholar
36 : Microglia from offspring of dams with allergic asthma exhibit epigenomic alterations in genes dysregulated in autism. Glia 2018; 66:505–521Crossref, Medline, Google Scholar
37 : To poly(I:C) or not to poly(I:C): advancing preclinical schizophrenia research through the use of prenatal immune activation models. Neuropharmacology 2012; 62:1308–1321Crossref, Medline, Google Scholar
38 : Adult brain and behavioral pathological markers of prenatal immune challenge during early/middle and late fetal development in mice. Brain Behav Immun 2008; 22:469–486Crossref, Medline, Google Scholar
39 : The time of prenatal immune challenge determines the specificity of inflammation-mediated brain and behavioral pathology. J Neurosci 2006; 26:4752–4762Crossref, Medline, Google Scholar
40 : Effects of prenatal infection on prepulse inhibition in the rat depend on the nature of the infectious agent and the stage of pregnancy. Behav Brain Res 2007; 181:270–277Crossref, Medline, Google Scholar
41 : Alterations in cognitive function and behavioral response to amphetamine induced by prenatal inflammation are dependent on the stage of pregnancy. Psychoneuroendocrinology 2011; 36:634–648Crossref, Medline, Google Scholar
42 : Effects of immune activation during early or late gestation on schizophrenia-related behaviour in adult rat offspring. Brain Behav Immun 2017; 63:8–20Crossref, Medline, Google Scholar
43 : A review of the fetal brain cytokine imbalance hypothesis of schizophrenia. Schizophr Bull 2009; 35:959–972Crossref, Medline, Google Scholar
44 : Long-term pathological consequences of prenatal infection: beyond brain disorders. Am J Physiol Regul Integr Comp Physiol 2015; 309:R1–R12Crossref, Medline, Google Scholar
45 : Maternal gut bacteria promote neurodevelopmental abnormalities in mouse offspring. Nature 2017; 549:528–532Crossref, Medline, Google Scholar
46 : Segmented filamentous bacteria take the stage. Mucosal Immunol 2010; 3:209–212Crossref, Medline, Google Scholar
47 : Comparative analysis of the distribution of segmented filamentous bacteria in humans, mice and chickens. ISME J 2013; 7:615–621Crossref, Medline, Google Scholar
48 : Genome sequences of segmented filamentous bacteria in animals: implications for human research. Gut Microbes 2012; 3:401–405Crossref, Medline, Google Scholar
49 : Inter-population variations in concentrations, determinants of and correlations between 2,2′,4,4′,5,5′-hexachlorobiphenyl (CB-153) and 1,1-dichloro-2,2-bis (p-chlorophenyl)-ethylene (p,p′-DDE): a cross-sectional study of 3161 men and women from Inuit and European populations. Environ Health 2005; 4:27Medline, Google Scholar
50 : Brain enlargement and increased behavioral and cytokine reactivity in infant monkeys following acute prenatal endotoxemia. Behav Brain Res 2011; 219:108–115Crossref, Medline, Google Scholar
51 : Toward a valid animal model of bipolar disorder: how the Research Domain Criteria help bridge the clinical-basic science divide. Biol Psychiatry 2016; 79:62–70Crossref, Medline, Google Scholar
52 : Behavioral animal models of antipsychotic drug actions. Handb Exp Pharmacol 2012; 212:361–406Crossref, Google Scholar
53 : Behavioural phenotyping assays for mouse models of autism. Nat Rev Neurosci 2010; 11:490–502Crossref, Medline, Google Scholar
54 : Modeling madness in mice: one piece at a time. Neuron 2006; 52:179–196Crossref, Medline, Google Scholar
55 : Maternal influenza infection during pregnancy impacts postnatal brain development in the rhesus monkey. Biol Psychiatry 2010; 67:965–973Crossref, Medline, Google Scholar
56 : Maternal immune activation in nonhuman primates alters social attention in juvenile offspring. Biol Psychiatry 2015; 77:823–832Crossref, Medline, Google Scholar
57 : Advances in nonhuman primate models of autism: integrating neuroscience and behavior. Exp Neurol 2018; 299:252–265Crossref, Medline, Google Scholar
58 : Why primate models matter. Am J Primatol 2014; 76:801–827Crossref, Medline, Google Scholar
59 : Elevated maternal C-reactive protein and increased risk of schizophrenia in a national birth cohort. Am J Psychiatry 2014; 171:960–968Link, Google Scholar
60 : Maternal exposure to toxoplasmosis and risk of schizophrenia in adult offspring. Am J Psychiatry 2005; 162:767–773Link, Google Scholar
61 : Prenatal exposure to maternal genital and reproductive infections and adult schizophrenia. Am J Psychiatry 2006; 163:927–929Link, Google Scholar
62 : Maternal exposure to herpes simplex virus and risk of psychosis among adult offspring. Biol Psychiatry 2008; 63:809–815Crossref, Medline, Google Scholar
63 : Maternal exposure to sexually transmitted infections and schizophrenia among offspring. Schizophr Res 2015; 166:255–260Crossref, Medline, Google Scholar
64 : Associations between maternal infection during pregnancy, childhood infections, and the risk of subsequent psychotic disorder: a Swedish cohort study of nearly 2 million individuals. Schizophr Bull 2016; 42:125–133Medline, Google Scholar
65 : Elevated maternal interleukin-8 levels and risk of schizophrenia in adult offspring. Am J Psychiatry 2004; 161:889–895Link, Google Scholar
66 : A longitudinal examination of the neurodevelopmental impact of prenatal immune activation in mice reveals primary defects in dopaminergic development relevant to schizophrenia. J Neurosci 2010; 30:1270–1287Crossref, Medline, Google Scholar
67 : Immune activation during pregnancy in mice leads to dopaminergic hyperfunction and cognitive impairment in the offspring: a neurodevelopmental animal model of schizophrenia. Biol Psychiatry 2006; 59:546–554Crossref, Medline, Google Scholar
68 : Prenatal exposure to the bacteriotoxin lipopolysaccharide leads to long-term losses of dopamine neurons in offspring: a potential, new model of Parkinson’s disease. Front Biosci 2003; 8:s826–s837Crossref, Medline, Google Scholar
69 : Stress in puberty unmasks latent neuropathological consequences of prenatal immune activation in mice. Science 2013; 339:1095–1099Crossref, Medline, Google Scholar
70 : Joint effects of exposure to prenatal infection and peripubertal psychological trauma in schizophrenia. Schizophr Bull 2017; 43:171–179Crossref, Medline, Google Scholar
71 : Gestational influenza and bipolar disorder in adult offspring. JAMA Psychiatry 2013; 70:677–685Crossref, Medline, Google Scholar
72 : Serological pattern consistent with infection with type I Toxoplasma gondii in mothers and risk of psychosis among adult offspring. Microbes Infect 2009; 11:1011–1018Crossref, Medline, Google Scholar
73 : Sensorimotor gating deficits in bipolar disorder patients with acute psychotic mania. Biol Psychiatry 2001; 50:418–424Crossref, Medline, Google Scholar
74 : Evidence of disrupted prepulse inhibition in unaffected siblings of bipolar disorder patients. Biol Psychiatry 2007; 62:1418–1422Crossref, Medline, Google Scholar
75 : Long-term effects of maternal immune activation on depression-like behavior in the mouse. Transl Psychiatry 2014; 4:e363Crossref, Medline, Google Scholar
76 : Animal models of maternal immune activation in depression research. Curr Neuropharmacol 2016; 14:688–704Crossref, Medline, Google Scholar
77 : The World Federation of Societies of Biological Psychiatry (WFSBP) Guidelines for the Biological Treatment of Bipolar Disorders: update 2009 on the treatment of acute mania. World J Biol Psychiatry 2009; 10:85–116Crossref, Medline, Google Scholar
78 : Maternal mid-pregnancy C-reactive protein and risk of autism spectrum disorders: the early markers for autism study. Transl Psychiatry 2016; 6:e783Crossref, Medline, Google Scholar
79 : Autoimmunity, autoantibodies, and autism spectrum disorder. Biol Psychiatry 2017; 81:383–390Crossref, Medline, Google Scholar
80 : Autism: maternally derived antibodies specific for fetal brain proteins. Neurotoxicology 2008; 29:226–231Medline, Google Scholar
81 : Maternal immune activation yields offspring displaying mouse versions of the three core symptoms of autism. Brain Behav Immun 2012; 26:607–616Crossref, Medline, Google Scholar
82 : Maternal immune activation and autism spectrum disorder: from rodents to nonhuman and human primates. Biol Psychiatry 2017; 81:391–401Crossref, Medline, Google Scholar
83 : Neurocognition in first-episode schizophrenia: a meta-analytic review. Neuropsychology 2009; 23:315–336Crossref, Medline, Google Scholar
84 : Prenatal exposure to maternal infection and executive dysfunction in adult schizophrenia. Am J Psychiatry 2009; 166:683–690Link, Google Scholar
85 : Structural brain alterations in schizophrenia following fetal exposure to the inflammatory cytokine interleukin-8. Schizophr Res 2010; 121:46–54Crossref, Medline, Google Scholar
86 : Abnormal trajectories of neurodevelopment and behavior following in utero insult in the rat. Biol Psychiatry 2011; 70:842–851Crossref, Medline, Google Scholar
87 : Maternal immune activation leads to behavioral and pharmacological changes in the adult offspring. J Psychiatr Res 2005; 39:311–323Crossref, Medline, Google Scholar
88 : Prenatal immune challenge is an environmental risk factor for brain and behavior change relevant to schizophrenia: evidence from MRI in a mouse model. PLoS One 2009; 4:e6354Crossref, Medline, Google Scholar
89 : Cognitive impairment following prenatal immune challenge in mice correlates with prefrontal cortical AKT1 deficiency. Int J Neuropsychopharmacol 2010; 13:981–996Crossref, Medline, Google Scholar
90 : Prenatal immune activation induces maturation-dependent alterations in the prefrontal GABAergic transcriptome. Schizophr Bull 2014; 40:351–361Crossref, Medline, Google Scholar
91 : Evidence that aetiological risk factors for psychiatric disorders cause distinct patterns of cognitive deficits. Eur Neuropsychopharmacol 2014; 24:879–889Crossref, Medline, Google Scholar
92 : Research Domain Criteria (RDoC): toward a new classification framework for research on mental disorders. Am J Psychiatry 2010; 167:748–751Link, Google Scholar
93 : The Danish National Birth Cohort: selected scientific contributions within perinatal epidemiology and future perspectives. Scand J Public Health 2011; 39(Suppl):115–120Crossref, Medline, Google Scholar
94 : Cohort profile: the Norwegian Mother and Child Cohort Study (MoBa). Int J Epidemiol 2006; 35:1146–1150Crossref, Medline, Google Scholar
95 : Perinatal phosphatidylcholine supplementation and early childhood behavior problems: evidence for CHRNA7 moderation. Am J Psychiatry 2016; 173:509–516Link, Google Scholar
96 : Long-term improvements in sensory inhibition with gestational choline supplementation linked to α7 nicotinic receptors through studies in Chrna7 null mutation mice. Brain Res 2014; 1552:26–33Crossref, Medline, Google Scholar
97 : Genome-wide association studies: findings at the major histocompatibility complex locus in psychosis. Biol Psychiatry 2014; 75:276–283Crossref, Medline, Google Scholar
98 : Schizophrenia risk from complex variation of complement component 4. Nature 2016; 530:177–183Crossref, Medline, Google Scholar
99 : Contribution of copy number variants to schizophrenia from a genome-wide study of 41,321 subjects. Nat Genet 2017; 49:27–35Crossref, Medline, Google Scholar
100 : Functional impact of global rare copy number variation in autism spectrum disorders. Nature 2010; 466:368–372Crossref, Medline, Google Scholar
101 : Biological insights from 108 schizophrenia-associated genetic loci. Nature 2014; 511:421–427Crossref, Medline, Google Scholar
102 : A genome-wide linkage and association scan reveals novel loci for autism. Nature 2009; 461:802–808Crossref, Medline, Google Scholar
103 : Genome-wide study of association and interaction with maternal cytomegalovirus infection suggests new schizophrenia loci. Mol Psychiatry 2014; 19:325–333Crossref, Medline, Google Scholar
104 : Evidence for an interaction between familial liability and prenatal exposure to infection in the causation of schizophrenia. Am J Psychiatry 2009; 166:1025–1030Link, Google Scholar
105 : Inflammatory biomarkers and risk of schizophrenia: a 2-sample mendelian randomization study. JAMA Psychiatry 2017; 74:1226–1233Crossref, Medline, Google Scholar
106 : Animal models of gene-environment interaction in schizophrenia: a dimensional perspective. Prog Neurobiol 2016; 136:1–27Crossref, Medline, Google Scholar
107 : The interaction between maternal immune activation and alpha 7 nicotinic acetylcholine receptor in regulating behaviors in the offspring. Brain Behav Immun 2015; 46:192–202Crossref, Medline, Google Scholar
108 : Prenatal interaction of mutant DISC1 and immune activation produces adult psychopathology. Biol Psychiatry 2010; 68:1172–1181Crossref, Medline, Google Scholar
109 : Maternal immune activation during gestation interacts with Disc1 point mutation to exacerbate schizophrenia-related behaviors in mice. J Neurosci 2013; 33:7654–7666Crossref, Medline, Google Scholar
110 : Phenotypic effects of maternal immune activation and early postnatal milieu in mice mutant for the schizophrenia risk gene neuregulin-1. Neuroscience 2014; 277:294–305Crossref, Medline, Google Scholar
111 : Prenatal immune activation interacts with genetic Nurr1 deficiency in the development of attentional impairments. J Neurosci 2012; 32:436–451Crossref, Medline, Google Scholar
112 : Epigenetic and transgenerational mechanisms in infection-mediated neurodevelopmental disorders. Transl Psychiatry 2017; 7:e1113Crossref, Medline, Google Scholar
113 : Molecular insights into transgenerational non-genetic inheritance of acquired behaviours. Nat Rev Genet 2015; 16:641–652Crossref, Medline, Google Scholar
114 : Prenatal nicotine exposure and risk of schizophrenia among offspring in a national birth cohort. Am J Psychiatry 2016; 173:799–806Link, Google Scholar
115 : Rate of de novo mutations and the importance of father’s age to disease risk. Nature 2012; 488:471–475Crossref, Medline, Google Scholar
116 : Advancing paternal age and autism. Arch Gen Psychiatry 2006; 63:1026–1032Crossref, Medline, Google Scholar
117 : Advancing paternal age and the risk of schizophrenia. Arch Gen Psychiatry 2001; 58:361–367Crossref, Medline, Google Scholar
118 : Genome-wide DNA methylation changes in a mouse model of infection-mediated neurodevelopmental disorders. Biol Psychiatry 2017; 81:265–276Crossref, Medline, Google Scholar
119 : Prenatal maternal immune activation causes epigenetic differences in adolescent mouse brain. Transl Psychiatry 2014; 4:e434Crossref, Medline, Google Scholar
120 : Alteration of imprinted Dlk1-Dio3 miRNA cluster expression in the entorhinal cortex induced by maternal immune activation and adolescent cannabinoid exposure. Transl Psychiatry 2014; 4:e452Crossref, Medline, Google Scholar
121 : Maternal immune activation epigenetically regulates hippocampal serotonin transporter levels. Neurobiol Stress 2016; 4:34–43Crossref, Medline, Google Scholar
122 : Transgenerational transmission and modification of pathological traits induced by prenatal immune activation. Mol Psychiatry 2017; 22:102–112Crossref, Medline, Google Scholar
123 : Maternal infection and schizophrenia: implications for prevention. Schizophr Bull 2011; 37:284–290Crossref, Medline, Google Scholar
124 : Control of the risk of human toxoplasmosis transmitted by meat. Int J Parasitol 2008; 38:1359–1370Crossref, Medline, Google Scholar
125 : Global control of sexually transmitted infections. Lancet 2006; 368:2001–2016Crossref, Medline, Google Scholar
126 Stoner BP: Sexually transmitted infections: overview, in International Encyclopedia of Public Health. Edited by Heggenhougen HK. San Diego, Academic Press, 2008, 713–723Google Scholar
127 : Influenza. New York, Plenum Medical Book Co, 1987Crossref, Google Scholar
128 : Seasonal influenza and 2009 H1N1 influenza vaccination coverage among pregnant women: 10 states, 2009–10 influenza season. MMWR Morb Mortal Wkly Rep 2010; 59:1541–1545Medline, Google Scholar
129 : Effectiveness of influenza vaccine during pregnancy in preventing hospitalizations and outpatient visits for respiratory illness in pregnant women and their infants. Am J Perinatol 2004; 21:333–339Crossref, Medline, Google Scholar
130 : Immunization during pregnancy against poliomyelitis and influenza in relation to childhood malignancy. Int J Epidemiol 1973; 2:229–235Crossref, Medline, Google Scholar
131 : Association between pandemic influenza A(H1N1) vaccination in pregnancy and early childhood morbidity in offspring. JAMA Pediatr 2017; 171:239–248Crossref, Medline, Google Scholar
132 : Modern Epidemiology. Philadelphia, Lippincott Williams and Wilkins, 1998Google Scholar
133 : Prenatal immune challenge disrupts sensorimotor gating in adult rats: implications for the etiopathogenesis of schizophrenia. Neuropsychopharmacology 2002; 26:204–215Crossref, Medline, Google Scholar
134 : The risk for behavioural deficits is determined by the maternal immune response to prenatal immune challenge in a neurodevelopmental model. Brain Behav Immun 2014; 42:138–146Crossref, Medline, Google Scholar
135 : Combination of prenatal immune challenge and restraint stress affects prepulse inhibition and dopaminergic/GABAergic markers. Prog Neuropsychopharmacol Biol Psychiatry 2013; 45:156–164Crossref, Medline, Google Scholar



