Office-Based Methadone Treatment for Opioid Use Disorder and Pharmacy Dispensing: A Scoping Review
Abstract
Objective:
The authors conducted a scoping review to survey the evidence landscape for studies that assessed outcomes of treating patients with opioid use disorder with methadone in office-based settings.
Methods:
Ovid MEDLINE and the Cochrane Database of Systematic Reviews were searched, and reference lists were reviewed to identify additional studies. Studies were eligible if they focused on methadone treatment in office-based settings conducted in the United States or other highly developed countries and reported outcomes (e.g., retention in care). Randomized trials and controlled observational studies were prioritized; uncontrolled and descriptive studies were included when stronger evidence was unavailable. One investigator abstracted key information, and a second verified data. A scoping review approach broadly surveyed the evidence, and therefore study quality was not rated formally.
Results:
Eighteen studies of patients treated with office-based methadone were identified, including six trials, eight observational studies, and four additional articles discussing use of pharmacies to dispense methadone. Studies on office-based methadone treatment, including primary care-based dispensing, were limited but consistently found that stable methadone patients valued office-based care and remained in care with low rates of drug use; outcomes were similar compared with stable patients in regular care. Office-based methadone treatment was associated with higher treatment satisfaction and quality of life. Limitations included underpowered comparisons and small samples.
Conclusions:
Limited research suggests that office-based methadone treatment and pharmacy dispensing could enhance access to methadone treatment for patients with opioid use disorder without adversely affecting patient outcomes and, potentially, inform modifications to federal regulations. Research should assess the feasibility of office-based care for less stable patients.
In the United States, federal regulations (title 42 of the Code of Federal Regulations, part 8 [42 CFR, part 8]) for opioid treatment programs (OTPs) require accreditation by organizations approved by the Substance Abuse and Mental Health Services Administration (SAMHSA), as well as adherence to SAMHSA’s standards of care and certification from SAMHSA (1). State regulations may also influence the delivery of care in OTPs (2). Because of federal legislation and regulations, methadone is dispensed only in federally certified OTPs for treatment of opioid use disorder.
Restriction of methadone dispensing to OTPs reduces access to potentially life-saving opioid agonist therapy. Individuals living in rural areas tend to have lengthy commutes to OTPs, which are located primarily in metropolitan settings (3). Daily dosing requirements further inhibit access to care. Because pharmacies dispense methadone prescribed for pain indications, using pharmacies to dispense methadone to OTP patients could facilitate access to opioid agonist therapy in rural communities (4, 5).
The Drug Addiction Treatment Act of 2000 (DATA 2000) amended federal statutes to permit office-based treatment with buprenorphine and facilitate access to opioid agonist therapy; office-based care is not generally permitted for methadone. A commentary published in the New England Journal of Medicine in 2018 advocated amendments to the Controlled Substances Act to allow buprenorphine-waivered physicians to prescribe methadone for opioid use disorder and to manage patients in their primary care practices with methadone dispensed in pharmacies (6). This is standard practice in many countries (7).
Office-based methadone treatment (also referred to as “methadone medical maintenance”) for stable patients can occur with SAMHSA-approved exceptions if the physician’s office is affiliated with an OTP (8). Routine use of office-based methadone treatment, however, is uncommon. To assess the harms, benefits, and feasibility of office-based methadone treatment, we conducted a scoping review (9, 10) to systematically survey the evidence landscape and highlight studies that assessed outcomes of treating patients with opioid use disorder with methadone in primary care settings and other office-based settings and/or with pharmacy dispensing for patients.
Methods
Search Strategies
We searched Ovid MEDLINE and the Cochrane Database of Systematic Reviews from database inception to July 2020. For a description of the search strategies, see Table S1 in the online supplement. We also reviewed reference lists of relevant articles to identify additional studies. The analysis was conducted as part of a larger scoping review of policy research on methadone treatment for opioid use disorder that covered additional research areas (Figure 1) (11). In the present analysis, we focused on the literature on methadone in office-based settings and U.S. studies of pharmacy dispensing of methadone.
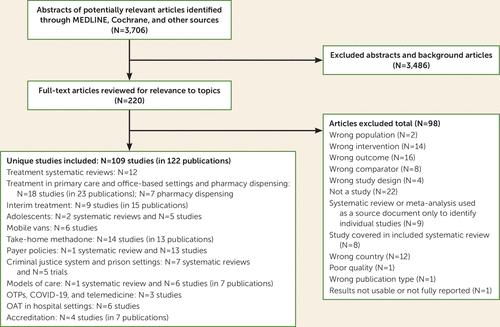
FIGURE 1. Flow diagram of studies assessing outcomes of opioid use disorder treatment with methadone in office-based settings in the United States and other highly developed countriesa
a Other topics included in the larger evidence review are also listed. OAT=opioid agonist therapy; OTPs=opioid treatment programs.
Study Selection
Studies were selected using a hierarchical approach. Randomized trials and controlled observational studies were prioritized; observational and descriptive studies were included when the priority evidence was unavailable. Studies addressing methadone policy were eligible if they focused on office-based settings and included outcomes (e.g., treatment initiation, treatment receipt, retention in care, or drug use) and were conducted in the United States or in other highly developed countries. One investigator abstracted key information (clinical setting, country, sample size, intervention/comparison, and main findings) into a table and a second investigator verified data. Because this was a scoping review that broadly surveyed the relevant literature, we used a descriptive approach to summarize the literature and did not formally synthesize or grade the quality of the evidence. The literature flow diagram is presented in Figure 1.
Results
We identified 18 studies of patients treated with office-based methadone in 23 publications, including six trials (with eight publications) (12–19), eight observational studies (with 11 publications) (20–30), and four descriptive studies (4, 5, 31, 32) (Table 1). Four randomized trials (with seven publications) (12–17, 30) were conducted in the United States (sample sizes ranged from N=26 to N=136), one in France (N=221) (18), and one in Australia (N=136) (19). Six observational studies (reported in nine publications) were U.S.-based studies. One group of medical methadone patients was reported in four publications; sample sizes increased from 28 to 156 participants, and follow-up increased from 1 to 15 years (23–26). The other U.S. observational studies had sample sizes from 10 to 127 participants (20–23, 27). Three non-U.S.-based observational studies included analyses from the United Kingdom (N=240; N=400) (28, 32) and Ireland (N=1,269) (29). One trial (16, 17) and three observational studies (20–22) of office-based methadone treatment utilized pharmacy dispensing, and pharmacy dispensing was addressed in four additional descriptive studies (4, 5, 31, 32).
| Study and Description | Study Design and Number of Patients | Setting and Location | Intervention | Main Findings | Limitations |
|---|---|---|---|---|---|
| U.S.-based RCTs | |||||
| Fiellin et al. (12) | RCT, N=46; SAMHSA and DEA exceptions | Office-based primary care setting; New Haven, Conn. | Comparison of methadone OTP in primary care with OTP in stabilized patients on methadone. A: primary care methadone dispensed in the office (N=22); B: OTP methadone opioid agonist therapy (N=24) | Similar rates of illicit drug use, functional status, and use of health, legal, or social services; primary care methadone maintenance more likely to be rated excellent by patients | Small sample |
| King et al. (13); 12-month follow-up results for King et al. (14) | RCT, N=92; SAMHSA and DEA exceptions | Primary care, office-based specialty setting compared with OTP; Baltimore | A: Methadone in office-based setting with 27 take-homes (N=33); B: methadone in OTP with 27 take-homes (N=32); C: usual methadone in OTP (N=27) | Low rates of drug use or failed medication recall; treatment satisfaction high in all groups; methadone patients initiated more new employment and family and social activities than usual methadone | Small sample |
| King et al. (14); same study as King et al. (13) with fewer study participants and 6 months of follow-up | N=73 | Same as above | Same as above | Six months of follow-up; overall, 1% of urine specimens were positive for illicit drugs; no evidence of methadone diversion; low rates of medication misuse | |
| Senay et al. (15) | RCT, N=130; FDA IND approval | Office-based specialty setting; U.S. | A: Medical methadone in office-based setting (N=89); B: usual methadone in OTP (N=41); OTP dispensed methadone for both patient groups | Retention rate, 73% for medical methadone compared with 73% for usual methadone treatment in OTP at 1 year; addiction severity similar in both groups at 1 year; no difference in positive urine toxicology screens | Small sample; dated study |
| Tuchman et al. (16); Tuchman et al. (17) | RCT, N=26; SAMHSA and DEA exceptions | Primary care setting; Santa Fe and Albuquerque, N.M., U.S. | A: Medical methadone in primary care setting (physician office, community pharmacy, and social work) (N=14; analyzed: N=13) compared with B: methadone in OTP (N=12; analyzed: N= 9) | At 12 months, retention was 100% compared with 89%; illicit opioid use was 23% compared with 78%; urine toxicology positive for cocaine was 23% compared with 44%; and urine toxicology positive for benzodiazepines was 8% compared with 44% | Small sample; women only; loss to follow-up; allowed participants to switch conditions following randomization |
| Non-U.S. RCTs | |||||
| Carrieri et al. (18) | RCT, N=221 | Primary care or specialty care setting in France; methadone dispensed at pharmacies for patients in primary care | A: Methadone induction in primary care (N=155); B: methadone induction in specialty care (N=66) | Methadone induction in primary care is feasible and acceptable to physicians and patients and similar to induction in specialized care for abstinence and retention | |
| Lintzeris et al. (19) | RCT, N=139 | Primarily primary care setting (18 general practitioner practice sites and one office-based specialist clinic); Australia | A: Office-based buprenorphine (with pharmacy dispensing); (N=73); B: methadone clinic-based buprenorphine (N=66) | Heroin use; retention similar in both groups | Study focused on initiation of buprenorphine; methadone patients had to be taking <60 mg/day before buprenorphine was initiated |
| U.S.-based observational studies | |||||
| Fiellin et al. (30); qualitative analysis of Fiellin (12) | Clinical chart audit of the 22 patients who received office-based methadone and focus group with six participating physicians providing care in the 2001 RCT of office-based methadone | Evaluation of processes of care during office-based treatment of OUD with methadone | Lapses in care (urine drug monitoring, paperwork completion) and barriers (logistics of dispensing, receipt of urine toxicology results, difficulties arranging psychiatric services, communications with OTP, and nonadherence to medication) identified; physicians recommended dispensing in pharmacies rather than their office | Small sample; no comparison group | |
| Drucker et al. (20); includes pharmacy dispensing | Observational study, uncontrolled retrospective treatment series, N=10; used FDA IND approval from Harris et al. (21) | Office-based specialty setting; Lancaster, Pa. | Evaluation of methadone agonist therapy in an office-based specialty setting with pharmacy dispensing in stabilized patients | Ten patients enrolled in office-based methadone and able to receive methadone in a community pharmacy; 1% (N=2/216) of urine drug tests positive for illicit substances; patients reported increased satisfaction | Small sample; no comparison group |
| Harris et al. (21); includes pharmacy dispensing | Observational study, uncontrolled retrospective treatment series, N=127; FDA IND approval | Office-based specialty setting; New York | Outcomes of office-based medical methadone program (N=127) and comparison with OTP patients (N=3,342); medical methadone patients were employed (or unemployed due to disability or retirement), had no evidence of opioid, cocaine, or benzodiazepine abuse in the past 3 years, and had psychiatric stability; methadone dispensed from a central pharmacy | Patients in office-based methadone medical settings were older than traditional OTP patients (mean age, 52 years compared with 44 years), and more likely to be male (72% compared with 59%) and Caucasian (50% compared with 17%); proportion with urine sample positive for nonprescribed opioids was 0.8% and 0.4% for cocaine | Small sample; office-based group |
| Merrill et al. (22); includes pharmacy dispensing | Observational study uncontrolled retrospective treatment series, N=30; SAMHSA and DEA exceptions | Primary care setting; Seattle | Evaluation of medical methadone therapy in primary care settings in stabilized patients; the hospital pharmacy dispensed the methadone | Retention at 1 year was 93%; positive urine drug screen was 6.7%; improvement in Addiction Severity Index score over time and patient satisfaction were high | Small sample; no comparison group |
| Des Jarlais et al. (23); initial patients for Novick et al. series (24–26) | Observational study, uncontrolled retrospective treatment series, N=28 (first 28 patients) at 12-month follow-up; FDA IND approval | Office-based specialty setting; New York (providers with experience in drug abuse treatment) | Evaluation of methadone agonist therapy in an office-based specialty setting in stabilized patients | At 12 months, 89% (N=25/28) retention; one patient successfully detoxified, one required short-acting opioid for surgery and back pain, and one requested transfer back to the methadone clinic; patients reported more mobility and privacy, less anxiety about treatment, improved employment situations, improved self-esteem, and perceived reduction in stigma | Small sample; no comparison group |
| Novick et al. (25) | Patients transferred from Rockefeller University to Beth Israel OTP, N=40 (first 40 participants) | Same as above | Methadone was from the hospital pharmacy and dispensed in the primary care office | 12–55 months of follow-up; 83% remained on medical methadone with a 94% annual retention rate; five returned to OTP because of cocaine use | Same as above |
| Novick et al. (24) | Follow-up data for 3.5–9.25 years (or status at discharge), N=100 | Same as above | Same as above | Retention was 98%, 95%, and 85% at 1, 2, and 3 years, respectively; cumulative proportional survival in treatment was 0.74 at 5 years and 0.56 at 9 years; after 42 to 111 months, 72 patients remained in good standing, 15 had unfavorable discharge, seven voluntarily withdrew in good standing, four died, one transferred to a chronic care facility, and one voluntarily left the program | Same as above |
| Salsitz et al. (26); report on 15 years | N=158 | Same as above | Same as above | 132 patients (84%) were program adherent and treatable within office-based settings; retention was 99%, 96%, and 89% at 1, 2, and 3 years, respectively; 13% died (no overdoses); 16% returned to OTP | Same as above |
| Schwartz et al. (27) | Observational study, uncontrolled retrospective treatment series, N=21; FDA IND approval | Primary care setting; Baltimore | Evaluation of medical methadone therapy in primary care settings in stabilized patients; methadone was dispensed in the primary care office | After 12 years, 29% of patients dropped out, and 0.5% urine samples were positive for drugs; no methadone overdose or diversion; participants reported significant improvement in quality of life | Small sample; no comparison group |
| Non-U.S. observational studies | |||||
| Gossop et al. (28) | Observational study; prospective sample, N=240 | Primary care setting compared with drug clinic setting; U.K. | A: Methadone in general practitioner clinics with dispensing from the office or community pharmacy (N=79) compared with B: methadone in drug clinics with dispensing in the clinic or community pharmacy (N=161) | Reductions in illicit drug use, injecting, sharing injection equipment, psychological and physical health problems, and crime in both groups at 1 and 2 years; patients in general practice settings had less frequent benzodiazepine and stimulant use and fewer psychological health problems | |
| Mullen et al. (29) | Retrospective randomly selected sample of methadone admissions in 1999, 2001, and 2003, N=1,269 | Central methadone treatment list; Ireland | Random sample of new patients receiving methadone treatment from specialty clinics, community medical clinics, and trained physicians in 1999, 2001, and 2003 to assess variables associated with retention in care | Participants were primarily men (69%), with a mean age of 26 years (75% under age 30); 95% received daily dosing with a mean dose of 58 mg/day; doses in primary care were lower (53 mg/day) compared with specialty clinics (60 mg/day); 61% remained in care for more than 1 year; primary cause of leaving in less than 1 year was “treatment failure”; logistic regression suggested retention at 12 months was associated with gender (women were more likely to remain in care); patients in specialty clinics were two times more likely to leave care than those in physician care; patients receiving a daily dose <60 mg/day were three times more likely to leave care than patients receiving doses >60 mg/day | |
| U.S. and non-U.S. pharmacy studies | |||||
| Bowden et al. (31) | Descriptive, uncontrolled retrospective treatment series of OTP patients with pharmacy dispensing, N=96; began prior to FDA regulations | Community pharmacies; San Antonio, Tex. | Description of community pharmacy dispensing of methadone for OUD (N=96); data collection began prior to the 1973 FDA regulations that restrict dispensing to OTPs | Retention was 70% at 1 year; 3% were voluntarily abstinent, 10% using heroin, 9% in jail, prison, or the hospital, 1% dead, 63% employed, and 15% partially employed; proportion arrested in the prior year decreased from 66% to 58% | Small sample; no comparison group |
| Joudrey et al. (4) | Descriptive, cross-sectional analysis of travel time to OTPs and pharmacies, N=7,918; census tracts in five states | OTPs compared with community pharmacies; U.S. | Comparison of drive time to OTP versus community pharmacies | Median drive time longer to OTP than chain pharmacies (19.6 compared with 4.4 minutes); difference greater in increasingly rural census tracts (11.5–35.2 minutes) | |
| Kleinman et al. (5) | Descriptive, cross-sectional analysis of travel time to OTPs and pharmacies, N=72,443; U.S. census tracts | OTPs compared with community pharmacies; U.S. | Comparison of drive time to OTPs (N=1,682) versus community pharmacies (N=69,475) | Mean population-weighted driving time was 20.4 minutes to OTPs and 4.5 minutes to pharmacies; drive times increased in metropolitan and noncore counties | |
| Keen et al. (32) | Descriptive, ecological analysis of methadone deaths before and after pharmacy dispensing of methadone as an opioid agonist therapy, N=400 | Primary care setting; U.K. | Evaluation of trends in methadone-associated mortality following implementation of widespread methadone prescribing in primary care; dispensing in community pharmacy | Decrease in methadone deaths in the city following implementation of widespread methadone prescribing in primary care, despite increase in methadone prescribing | |
TABLE 1 Office-based methadone treatment and pharmacy studies in the United States and other highly developed countriesa
U.S. Clinical Trials
The first clinical trial of office-based methadone treatment (medical methadone maintenance) was a 1993 initiative in Chicago that recruited 130 stable patients from 14 OTPs (15). Patients were selected for study inclusion if they had a year or more of methadone treatment and if for the past 6 months had no positive urine screens, were employed, had plans to remain on methadone for the next year, and were adherent to treatment plans. Participants were randomly assigned in a 2:1 ratio to medical methadone (N=87) or continuing care at the OTP (N=43). Medical methadone patients had monthly physician visits and two medication visits per month at their original OTP and received 13 days of take-home medication. The OTP continued to provide counseling services. The comparison group remained in their OTP with two medication visits per week (N=43) (i.e., two or three take-home medications per visit). After 6 months, participants in the comparison group were enrolled in the medical methadone program. The two groups had similar completion rates at six (89% compared with 85%) and 12 months (both groups, 73%), and rates of positive urine screens were less than 1% in both groups (16). All patients were satisfied with the services, and none wanted to return to treatment as usual (two medication visits per week) (15).
In the second trial, conducted in New Haven, Conn., 46 stable methadone patients (i.e., patients were required to have been in an OTP for more than 1 year, have no positive urine screens for opioids or cocaine in the past year, have plans to remain in the OTP for 6 months, have no co-occurring medical, psychiatric, or substance use disorder, and have transportation to the clinic or office and legal income and stable housing) were recruited from an OTP and randomly assigned to either six primary care internists who provided office-based methadone agonist therapy (N=22) (with methadone dispensed in the physician’s office) or to usual care in the OTP (N=24) for 6 months (12). The groups had similar rates of opioid-positive urine screens (9% compared with 11%) and clinical instability (i.e., defined a priori as two consecutive urine drug screens detecting cocaine or opioid metabolites or detecting no methadone) (18% compared with 21%) during the 6-month study period; the office-based patients were more likely to rate the care as excellent (73% compared with 13%) (12). A secondary qualitative analysis (included in Table 1 as an observational study) reviewed the office records and interviewed physicians to identify barriers to office-based methadone treatment. Physicians reported that the urine drug monitoring and extra paperwork required for methadone dispensing were barriers to continued office-based care and recommended that studies be conducted using pharmacies for dispensing (30). Additional barriers were patient access to psychiatric services, communication with the OTP, and patient nonadherence to medication (30).
In a third trial, based in Baltimore, 92 stable methadone patients (i.e., in the past year, the patients had an uninterrupted episode of methadone maintenance, no positive urine screens for any drug, verified employment, no failed methadone medication checks [the patient was recalled to the OTP, where the remaining doses were counted to verify that the medication was being used correctly], and plans to remain in care for the duration of the study) were randomly assigned to one of three groups: 28-day methadone treatment in a physician’s office (office-based, N=32), 28-day methadone maintenance in an OTP (clinic-based, N=33), or regular methadone maintenance in an OTP with one or two visits per week for medication (routine care, N=27) (13). For all study participants, an adaptive treatment model was used that intensified services (additional counseling required) if urine screens were positive for illicit drugs or the weekly medication checks were incorrect (14). After 6 months of the 12-month study period, the three study groups had similar outcomes: 1% of urine screens detected illicit drug use, drug diversion was not observed, methadone misuse was limited, patients were satisfied or very satisfied (patients receiving 28-day supplies of methadone were more satisfied), and patients accepted the treatment intensification (14). At the 12-month follow-up, 77 participants were still in care. Few patients tested positive for illicit drug use or missed medication recalls (the groups did not differ significantly) (13). The three groups also did not differ in the use of treatment intensification (36% of patients), self-reported drug use was minimal, and all patients reported being satisfied or very satisfied with the services. However, patients in both of the 28-day medication groups (office-based and clinic-based) were more satisfied than those in routine care and were more likely to report improved employment and social activities (13).
The fourth trial, a pilot study conducted in New Mexico, tested office-based primary care and methadone medical management with dispensing from community pharmacies, and a social worker provided counseling and case coordination. Women (N=26) who were enrolled in an OTP and were stable were randomly assigned to either continued care in the OTP (N=12) or office-based care (N=14) (17). A treatment manual specified roles and responsibilities for the five pharmacists, five medical practitioners (four physicians and one nurse practitioner), and one master’s-level social worker with experience treating drug use disorders. The pharmacies were registered with the U.S. Drug Enforcement Administration (DEA) and dispensed methadone as medication units for the OTPs. The social worker provided clinical coordination and at least monthly psychosocial services (in her office or at the participant’s home) and participated in weekly case conferences. The medical practitioners were listed as OTP staff and met with patients at least monthly for medical and medication management and urine drug screens (16, 17). Patients eligible for participation in the study had at least 6 months of methadone treatment, 6 months of stable methadone dosage, at least two take-home doses per week, and plans to remain on methadone for the 12-month study period. The analysis was restricted to participants who completed the 12-month follow-up period (N=22) (office-based care, N=13; OTP care, N=9). Two office-based care participants were returned to the OTP early in the study period for illicit drug use and mental health problems. Patients in office-based care were less likely to use illicit opioids (23% compared with 78%; χ2=6.4, df=1, p<0.05) during the 1-year study period (16, 17). A qualitative analysis of a satisfaction survey suggested that patients receiving community services were pleased with the services and were treated well (16). The small sample generated imprecise estimates.
Non-U.S. Randomized Trials
There were two non-U.S. randomized trials, one conducted in France and the other in Australia. The French trial (N=221) compared methadone initiation in primary care compared with specialty care; it found that methadone initiation in primary care was feasible and acceptable to physicians and patients, with similar rates of abstinence and retention compared with specialty care induction (18). Office-based methadone treatment is not typically available in France, and this was the first evaluation of office-based care. The Australian randomized trial (N=139) recruited stable methadone patients and active heroin users and randomly assigned participants to receive buprenorphine in a methadone clinic (N=66) compared with buprenorphine in an office-based setting (with pharmacy dispensing) (N=73) (19). Self-reported heroin use and retention in care were similar in both settings (19).
U.S. Observational Studies
Observational studies conducted in the United States echoed results from the clinical trials; stable methadone patients responded to office-based methadone treatment with high levels of retention in care and low rates of drug use (21–27). With one exception (21), the studies described only patients who received office-based methadone treatment and did not include an OTP comparison. Across studies, patients receiving office-based methadone treatment generally had monthly physician visits with observed dosing and urine tests. In most of the studies, patients received take-home medication directly from the physician (pharmacies delivered medication to the office setting the day prior to scheduled appointments).
In 1983, Dr. Marie Nyswander used an Investigational New Drug approval for methadone by the U.S. Food and Drug Administration (FDA) to open the first medical methadone maintenance program for stable methadone patients in New York City; the initial report on the program described 1-year results for 28 patients (23). The study was restricted to patients who met 10 eligibility criteria: 5 years of conventional methadone treatment, 3 years of stable employment, no criminal involvement for the past 3 years, no illicit drug use and no alcohol abuse for the past 3 years, reliable clinic attendance, a need for continued maintenance, no need for psychiatric medication, no social ties to drug users, clinical recommendations to participate, and a willingness to participate in research interviews. Take-home medication was dispensed during the medical visits. Subsequent analyses expanded the size of the program and the duration of follow-up from 40 patients with 12 to 55 months of follow-up (25) to 100 patients with up to 9 years of follow-up (24) and 15 years with 158 study participants (26). Treatment retention rates declined slightly over time, rates of discharge for drug use were low, and over 15 years, 16% of the medical methadone patients were returned to methadone clinics.
A second New York City study, also conducted under an FDA Investigational New Drug protocol, compared patients receiving office-based methadone treatment with patients treated in an OTP (21). Participating patients were employed, had no evidence of illicit drug use in the past 3 years, and were psychiatrically stable. When the medical maintenance patients (N=127) were compared with the OTP patients (N=3,342), patients in the office-based setting were older (mean age, 52 years compared with 44 years) and more likely to be male (72% compared with 59%) and White (59% compared with 17%). Within the medical methadone group, the rate of illicit opioids and cocaine detected in monthly urine drug tests was less than 1%, and unannounced recalls found no evidence of diversion or inappropriate use. Patients received take-home medication in a central pharmacy near the physician’s office (21).
The other studies reported outcomes of patients receiving office-based methadone treatment without comparisons to OTP patients. A Baltimore-based analysis described 21 stable methadone patients enrolled in a medical maintenance program with take-home methadone dispensed in the physician’s office (27). Participating patients were employed and had 5 years of abstinence from illicit drug use, no evidence of alcohol use disorder, and no concurrent psychiatric disorders. Urine drug tests were conducted monthly. After 12 years, 71% of the patients remained in care, with 0.5% urine tests positive for drug use and no methadone overdoses or diversion (27). Participants reported significant improvement in quality of life and ability to travel.
A small study (N=10) conducted in rural Pennsylvania described the use of a community physician and a community pharmacy to monitor and dispense methadone to stable patients (i.e., with a median of 3 years in OTP care without evidence of current drug use) living 40 miles from the OTP (20). The first pharmacy dispensing occurred in July 2003 (despite objections from the state alcohol and drug authority). All patients were enrolled in a local internal medicine clinic; the clinic’s director was certified in addiction medicine and wrote monthly medication orders that could be filled only at the participating pharmacy. The pharmacy observed one dose and provided weekly or biweekly take-home medication. The primary care practice provided counseling and urine testing. Participating patients paid pharmacy charges out of pocket. Five of 216 (2.3%) urine tests were positive for drugs other than methadone (three for prescribed medications and two for illicit drugs). Study participants felt comfortable in the pharmacy and liked being treated like a customer; they were pleased with the physician and his skills and grateful for the program. Pharmacy staff reported that the bottle return requirement was unnecessary and that the lockbox was stigmatizing (20). Despite the results, the state alcohol and drug authority remained uncomfortable with the program and in July 2005 ordered the patients to return to the original OTP 40 miles away. Most patients switched to buprenorphine and remained in care with the internal medicine clinic (20).
Harborview Medical Center in Seattle partnered with Evergreen Treatment Services (an OTP) and requested SAMHSA and DEA exceptions and state exemptions from opioid treatment regulations (22). The OTP continued to provide counseling, and the hospital provided pharmacy and medical clinic services. The OTP patients were screened for medical maintenance eligibility, and of the 49 individuals who met study eligibility criteria (i.e., at least four take-home medications each week, with reliable attendance, monthly urine screens negative for drug use, no evidence of alcohol use disorder, no legal issues or unpaid program fees, and no psychiatric disorders), 30 agreed to participate (22). Participants picked up methadone medication once or twice per month from the hospital pharmacy, and pharmacists assessed patient stability and primary care needs, collected a monthly urine sample, observed patients take their regular dose, and dispensed take-home doses. Monitoring included random callbacks, which required patients to return to the pharmacy within 24 hours to confirm pill counts. Physician visits were adjusted according to clinical need. When participants entered medical maintenance, their mean age was 45 years, and most were male (70%), White (83%), and employed (83%), with a mean of 12 years on methadone, 7 years of take-home medication privileges, and a mean daily dose of 63 mg of methadone. Eighty percent had Medicaid or other health insurance. In the first 12 months of program participation, less than 1% of urine tests were positive for illicit drugs, callbacks found no discrepancies, and two patients were transferred back to the OTP. Scores on the Addiction Severity Index medical subscale improved, other subscale scores were low and stable, and 87% of patients were very satisfied with the medical maintenance program (22).
Non-U.S. Observational Analyses
The search found two non-U.S. observational analyses: one conducted in England (28) and one in Ireland (29). England’s National Treatment Outcome Research Study compared patients with methadone prescriptions from a general practitioner (N=79) with patients enrolled in specialized drug clinics (N=161) (28). At 12 and 24 months after treatment entry, patients in both groups reported reduced illicit drug use, injecting, syringe sharing, mental health symptoms, medical problems, and criminal activity (28). Finally, a study of a random sample of patients in Ireland’s Central Methadone Treatment List who began care in 1999, 2001, and 2003 (N=1,269) assessed retention in care and patient characteristics associated with retention in care (29). Sixty-one percent of patients remained in care for more than 1 year, and patients in primary care were twice as likely as patients in specialty methadone clinics to be retained for the full year (29).
Pharmacy Dispensing
Four U.S. studies of office-based methadone treatment (three observational studies [20–22] and one clinical trial [17]) used pharmacies as medication units to dispense methadone take-home medication. When compared with studies with office dispensing, outcomes appeared to be similar. A small trial used community pharmacies (with special approvals from the DEA) (17). An observational study described how the hospital pharmacy conducted observed doses and dispensed take-home methadone before business hours (22). A second study used a central pharmacy near the physician offices (21). In the third analysis, a community pharmacy dispensed methadone for rural patients who initially enrolled in an OTP 40 miles from where they lived (20).
A 1970 initiative in San Antonio, Tex., utilized pharmacy dispensing to expand the OTP’s caseload by 30% (31). Each pharmacy purchased, stored, and dispensed its own supply of methadone (1970–1972) until the 1973 FDA regulations required the OTP to purchase, store, and deliver methadone as needed (31). The study described a group of 96 patients who received 12 months of methadone dispensed in pharmacies. The study did not include a comparison group (31). An ecological, before-after study conducted in the United Kingdom found a decrease in methadone deaths following implementation of office-based methadone treatment with pharmacy dispensing, despite increased methadone prescribing (32).
Two analyses using census tract data observed that patients’ travel burden for daily dispensing could be reduced if pharmacies dispensed methadone. The drive time to an OTP was greater than the drive time to a pharmacy (20 minutes compared with 4 minutes); the difference increased in rural communities (4, 5).
Discussion
Studies on office-based methadone treatment were consistent in finding that stable methadone patients responded to office-based care with higher treatment retention rates and greater treatment satisfaction, employment, and engagement in family and social activities (12–14, 22, 27). The operationalization of “stable patient” varied but typically required participants to have a year or more of urine drug tests negative for illicit drugs, have reliable clinic attendance, and be housed and employed. There was no evidence of methadone diversion, although only three of the studies included recalls to assess appropriate use of take-home medication (13, 21, 22).
The initial U.S. studies required Investigational New Drug approvals from the FDA for an exemption from U.S. regulations limiting methadone treatment to OTPs. Subsequent studies, however, were conducted with DEA and SAMHSA exemption requests for office-based practices affiliated with an OTP (8). Pharmacies can also be approved as OTP medication units specifically to dispense methadone with a formal OTP affiliation. These mechanisms, however, have not been used widely to promote access to methadone, despite increases in opioid use disorder and opioid overdoses.
One influence on the limited routine use of office-based methadone treatment may be the economics and financing of OTPs. Stable patients are more likely to be employed, with more income, and consequently pay higher fees when sliding fee scales are applied to the cost of patient care (33). In the current system of OTP care, there is no economic incentive for OTPs to transfer patients to primary care practices. Traditionally, third-party payers often required OTPs to provide in-person care in order to receive reimbursement. The recent introduction of relaxed restrictions on take-home medication and permission to use telemedicine because of the COVID-19 pandemic (34) have begun to alter the payment structures for OTPs and may create incentives to expand caseloads by transferring stable patients to OTP-affiliated physicians (e.g., in a hub-and-spoke model).
Limitations
The U.S. randomized trials were unblinded, with small samples in most of the studies that may have been underpowered to detect differences in outcomes. Study samples were also too small to detect infrequent adverse events, and follow-up periods varied across the studies. The observational studies were primarily descriptive, and most did not control for possible confounding characteristics or include comparison groups. Few studies, moreover, have been conducted in the past 20 years; results, therefore, are dated and may not generalize to the current environment. Nonetheless, the studies provide evidence that stable methadone patients benefit from office-based care.
However, patients were carefully selected, and although the operationalization of “stable patient” varied, at least 6 months of OTP care was required, along with no evidence of drug use. No U.S. studies tested office-based care with patients new to care. In the French study, however, methadone patients successfully initiated methadone and were stabilized in office-based settings. Finally, while office-based methadone treatment is relatively common in other countries, the international studies relied on retrospective analyses using historical data, and the clinical trials tested facets of methadone services (i.e., switching to buprenorphine) that may be of limited applicability to U.S. settings.
Practice and Policy Implications
The association between access to opioid agonist therapy and improved patient outcomes is well described in the literature. Our findings suggest that modifications to current methadone policies to allow for health services delivery changes (specifically, office-based prescribing of methadone for stabilized patients) could enhance access to care. Pharmacy dispensing of methadone would further facilitate access to effective treatment for opioid use disorder, especially in rural communities. Pharmacies are an integral part of methadone treatment in Canada and Europe. U.S. pharmacies already dispense methadone when it is prescribed for pain, and there are no obvious barriers to using pharmacies in the United States, aside from current DEA regulations that prohibit physicians from prescribing methadone for opioid use disorder and pharmacists from filling methadone prescriptions for opioid use disorder. Recent analyses highlight the distance many patients in rural areas travel to access methadone services and advocate for the use of rural pharmacies as medication units (3, 5).
An expansion of methadone services may also begin to address persistent racial disparities in care, which are observed in the current design of the opioid agonist treatment system (35, 36). Black patients, for example, are less likely to have access to and receive office-based care with buprenorphine (37). Implementation of office-based methadone treatment should include a critical assessment of its impact on access, with intentional efforts to increase access to minoritized populations.
Some physicians, moreover, appear to be interested in caring for their patients using methadone for opioid use disorder. Interviews with 71 primary care and HIV providers in 11 New York City practices determined that most (85%) had provided medical care for methadone patients, 70% were comfortable managing medical care for drug users in the primary care setting, and 66% were willing to prescribe methadone for OTP patients in their caseload if training and support were available. However, half the respondents were concerned that methadone patients often have multiple needs that could be difficult to address in their practice setting (38). It should be noted, however, that relatively few physicians have the DATA 2000 waiver to prescribe buprenorphine for opioid use disorder and that among those who have the waiver, many do not use it. There is widespread hesitancy to address opioid use disorder in clinical practice.
Future Research
It is noteworthy that aside from recent modeling studies of drive time to pharmacies compared with OTPs and two international analyses, all of the studies were published in the 1980s, the 1990s, and the first decade of the 21st century. New trials of office-based methadone treatment using contemporary patients with opioid use disorder would help verify the continued applicability of office-based methadone treatment.
In addition, all of the U.S. studies were limited to stable OTP patients. As a result, the lack of data on patients new to care is a major gap in the research literature. There are no data on the risks and benefits of office-based methadone treatment for patients new to care. While clinical evidence suggests that patients continue to use drugs while new to care, the evidence also suggests that for many patients, opioid agonist therapy helps them to stabilize; they respond well to care, and their drug use dissipates over time. It is likely that some federally qualified health centers have the resources and skills to work effectively with methadone patients who are new to care. Given the need for more access to methadone services in nonmetropolitan communities, it is critical to test office-based methadone treatment for patients seeking treatment for opioid use disorder. One option would be to extend the buprenorphine hub-and-spoke model to include methadone patients (patients are stabilized on medication in an OTP and transferred to office-based practices when stable [39–41]).
Despite the potential advantages of methadone dispensing in pharmacies, the research on it is limited. Our search found only five studies that used pharmacy dispensing, and one study was initiated prior to the 1973 methadone regulations (31); in two studies, the pharmacies operated as medication units (17, 22). Qualitative implementation research would be useful to understand perceived barriers to the use of pharmacies to dispense methadone and development of strategies to address potential barriers. Clinical trials and other studies evaluating clinical or administrative data are needed to document the safety of pharmacy dispensing and potential effects on reducing burdens on patients, particularly for those located in areas requiring lengthy travel to an OTP. Additional research could inform changes to regulations to encourage greater use of pharmacies for methadone dispensing.
Another strategy to increase access to methadone is use of mobile medication units: methadone vans. Since 2006, the DEA has not approved new mobile medication units. Aside from a handful of studies (42, 43), little systematic research has been conducted to test facets of mobile medication units. In February 2020, the DEA released a draft of changes in regulations that would permit a resumption of approvals. Renewed approvals will provide opportunities for implementation research on the development and use of mobile medication units.
Conclusions
In stable patients, office-based methadone treatment appears to be associated with similar retention, drug use, and other outcomes found in stable OTP patients and may enhance quality of life and satisfaction with care. Research is needed on office-based methadone treatment for patients new to care. Office-based methadone treatment and pharmacy dispensing could enhance access to methadone treatment for patients with opioid use disorder. Because of the complexity of chapter 42 CFR, part 8, a comprehensive review of OTP regulations may be useful, including an update of the 1995 Institute of Medicine review of methadone regulations (44).
1.
2. : Characterizing variability in state-level regulations governing opioid treatment programs. J Subst Abuse Treat 2020; 115:108008Crossref, Medline, Google Scholar
3. : Drive times to opioid treatment programs in urban and rural counties in 5 US states. JAMA 2019; 322:1310–1312Crossref, Medline, Google Scholar
4. : Pharmacy-based methadone dispensing and drive time to methadone treatment in five states within the United States: a cross-sectional study. Drug Alcohol Depend 2020; 211:107968Crossref, Medline, Google Scholar
5. : Comparison of driving times to opioid treatment programs and pharmacies in the US. JAMA Psychiatry 2020; 77:1163–1171Crossref, Medline, Google Scholar
6. : Methadone in primary care: one small step for Congress, one giant leap for addiction treatment. N Engl J Med 2018; 379:7–8Crossref, Medline, Google Scholar
7. : Global opioid agonist treatment: a review of clinical practices by country. Addiction 2020; 115:2243–2254Crossref, Medline, Google Scholar
8. Substance Abuse and Mental Health Services Administration: Dear colleague letter on methadone medical maintenance. Rockville, Md, Substance Abuse and Mental Health Services Administration, 2000. https://www.samhsa.gov/sites/default/files/programs_campaigns/medication_assisted/dear_colleague_letters/2000-colleague-letter-methadone-medical-maintenance.pdfGoogle Scholar
9. : Progress notes: methods for research evidence synthesis: the scoping review approach. J Hosp Med 2019; 14:416–418Crossref, Medline, Google Scholar
10. : Systematic review or scoping review? Guidance for authors when choosing between a systematic or scoping review approach. BMC Med Res Methodol 2018; 18:143Crossref, Medline, Google Scholar
11. : Methadone treatment regulations in the United States: ci, current status, evidence, and policy considerations. Portland, Northwest Evidence-Based Practice Center, Oregon Health and Science University, 2020Google Scholar
12. : Methadone maintenance in primary care: a randomized controlled trial. JAMA 2001; 286:1724–1731Crossref, Medline, Google Scholar
13. : A 12-month controlled trial of methadone medical maintenance integrated into an adaptive treatment model. J Subst Abuse Treat 2006; 31:385–393Crossref, Medline, Google Scholar
14. : A multicenter randomized evaluation of methadone medical maintenance. Drug Alcohol Depend 2002; 65:137–148Crossref, Medline, Google Scholar
15. : Medical maintenance: a pilot study. J Addict Dis 1993; 12:59–76Crossref, Medline, Google Scholar
16. : A model-guided process evaluation: office-based prescribing and pharmacy dispensing of methadone. Eval Program Plann 2008; 31:376–381Crossref, Medline, Google Scholar
17. : Safety, efficacy, and feasibility of office-based prescribing and community pharmacy dispensing of methadone: results of a pilot study in New Mexico. Addict Disord Their Treat 2006; 5:43–51Crossref, Google Scholar
18. : Methadone induction in primary care for opioid dependence: a pragmatic randomized trial (ANRS Methaville). PLoS One 2014; 9:e112328Crossref, Medline, Google Scholar
19. : Implementing buprenorphine treatment in community settings in Australia: experiences from the Buprenorphine Implementation Trial. Am J Addict 2004; 13(Suppl 1):S29–S41Crossref, Medline, Google Scholar
20. : The Lancaster office based opiate treatment program: a case study and prototype for community physicians and pharmacists providing methadone maintenance treatment in the United States. Addict Disord Their Treat 2007; 6:121–135Crossref, Google Scholar
21. : A 5-year evaluation of a methadone medical maintenance program. J Subst Abuse Treat 2006; 31:433–438Crossref, Medline, Google Scholar
22. : Methadone medical maintenance in primary care: an implementation evaluation. J Gen Intern Med 2005; 20:344–349Crossref, Medline, Google Scholar
23. : Medical maintenance feasibility study. NIDA Res Monogr 1985; 58:101–110Medline, Google Scholar
24. : Outcomes of treatment of socially rehabilitated methadone maintenance patients in physicians’ offices (medical maintenance): follow-up at three and a half to nine and a fourth years. J Gen Intern Med 1994; 9:127–130Crossref, Medline, Google Scholar
25. : Methadone maintenance patients in general medical practice: a preliminary report. JAMA 1988; 259:3299–3302Crossref, Medline, Google Scholar
26. : Methadone medical maintenance (MMM): treating chronic opioid dependence in private medical practice: a summary report (1983–1998). Mt Sinai J Med 2000; 67:388–397Medline, Google Scholar
27. : A 12-year follow-up of a methadone medical maintenance program. Am J Addict 1999; 8:293–299Crossref, Medline, Google Scholar
28. : Methadone treatment for opiate dependent patients in general practice and specialist clinic settings: outcomes at 2-year follow-up. J Subst Abuse Treat 2003; 24:313–321Crossref, Medline, Google Scholar
29. : A national study of the retention of Irish opiate users in methadone substitution treatment. Am J Drug Alcohol Abuse 2012; 38:551–558Crossref, Medline, Google Scholar
30. : Processes of care during a randomized trial of office-based treatment of opioid dependence in primary care. Am J Addict 2004; 13(suppl 1):S67–S78Crossref, Medline, Google Scholar
31. : Methadone dispensing by community pharmacies. Am J Drug Alcohol Abuse 1976; 3:243–254Crossref, Medline, Google Scholar
32. : Methadone maintenance treatment can be provided in a primary care setting without increasing methadone-related mortality: the Sheffield experience 1997–2000. Br J Gen Pract 2002; 52:387–389Medline, Google Scholar
33. : Medical maintenance in methadone care: a clinical pharmacy practice opportunity. J Pharm Pract 1997; 10:346–351Crossref, Google Scholar
34. : Reduction in Oregon’s methadone dosing visits following the SARS-CoV-2 restrictions on take-home medication. J Addict Med (Online ahead of print, February 5, 2021)Google Scholar
35. : Two tiers of biomedicalization: methadone, buprenorphine, and the racial politics of addiction treatment. Adv Med Sociol 2012; 14:79–102Crossref, Google Scholar
36. : Variation in use of buprenorphine and methadone treatment by racial, ethnic, and income characteristics of residential social areas in New York City. J Behav Health Serv Res 2013; 40:367–377Crossref, Medline, Google Scholar
37. : Buprenorphine treatment divide by race/ethnicity and payment. JAMA Psychiatry 2019; 76:979–981Crossref, Medline, Google Scholar
38. : Office-based methadone prescribing: acceptance by inner-city practitioners in New York. J Urban Health 2000; 77:96–102Crossref, Medline, Google Scholar
39. : Assessment of medication for opioid use disorder as delivered within the Vermont hub and spoke system. J Subst Abuse Treat 2019; 97:84–90Crossref, Medline, Google Scholar
40. : Implementation of the hub and spoke model for opioid use disorders in California: rationale, design, and anticipated impact. J Subst Abuse Treat 2020; 108:20–25Crossref, Medline, Google Scholar
41. : Multi-model implementation of evidence-based care in the treatment of opioid use disorder in Pennsylvania. J Subst Abuse Treat 2019; 106:58–64Crossref, Medline, Google Scholar
42. : Patient retention in mobile and fixed-site methadone maintenance treatment. Drug Alcohol Depend 1996; 42:125–131Crossref, Medline, Google Scholar
43. : Mobile opioid agonist treatment and public funding expands treatment for disenfranchised opioid-dependent individuals. J Subst Abuse Treat 2014; 46:511–515Crossref, Medline, Google Scholar
44. Rettig RA, Yarmolinsky A (eds): Federal Regulation of Methadone Treatment. Washington, DC, National Academy Press, 1995Google Scholar



