Individual Treatment of Posttraumatic Stress Disorder Using Mantram Repetition: A Randomized Clinical Trial
Abstract
Objective:
Previous studies suggest that group “mantram” (sacred word) repetition therapy, a non-trauma-focused complementary therapy for posttraumatic stress disorder (PTSD), may be an effective treatment for veterans. The authors compared individually delivered mantram repetition therapy and another non-trauma-focused treatment for PTSD.
Method:
The study was a two-site, open-allocation, blinded-assessment randomized trial involving 173 veterans diagnosed with military-related PTSD from two Veterans Affairs outpatient clinics (January 2012 to March 2014). The mantram group (N=89) learned skills for silent mantram repetition, slowing thoughts, and one-pointed attention. The comparison group (N=84) received present-centered therapy, focusing on currently stressful events and problem-solving skills. Both treatments were delivered individually in eight weekly 1-hour sessions. The primary outcome measure was change in PTSD symptom severity, as measured by the Clinician-Administered PTSD Scale (CAPS) and by self-report. Secondary outcome measures included insomnia, depression, anger, spiritual well-being, mindfulness, and quality of life. Intent-to-treat analysis was conducted using linear mixed models.
Results:
The mantram group had significantly greater improvements in CAPS score than the present-centered therapy group, both at the posttreatment assessment (between-group difference across time, −9.98, 95% CI=−3.63, −16.00; d=0.49) and at the 2-month follow-up (between-group difference, −9.34, 95% CI=−1.50, −17.18; d=0.46). Self-reported PTSD symptom severity was also lower in the mantram group compared with the present-centered therapy group at the posttreatment assessment, but there was no difference at the 2-month follow-up. Significantly more participants in the mantram group (59%) than in the present-centered therapy group (40%) who completed the 2-month follow-up no longer met criteria for PTSD (p<0.04). However, the percentage of participants in the mantram group (75%) compared with participants in the present-centered therapy group (61%) who experienced clinically meaningful changes (≥10-point improvements) in CAPS score did not differ significantly between groups. Reductions in insomnia were significantly greater for participants in the mantram group at both posttreatment assessment and 2-month follow-up.
Conclusions:
In a sample of veterans with PTSD, individually delivered mantram repetition therapy was generally more effective than present-centered therapy for reducing PTSD symptom severity and insomnia.
An estimated 13%–20% of U.S. troops returning from Iraq and Afghanistan may have posttraumatic stress disorder (PTSD) (1), and an estimated 30% of Vietnam-era veterans have lifetime PTSD (2). In randomized trials, trauma-focused cognitive processing therapy, prolonged exposure, and eye movement desensitization and reprocessing have demonstrated clinically meaningful improvements in patients with military-related PTSD (3–7). However, a recent review found that despite strong within-group improvements from prolonged exposure and cognitive processing therapy (Cohen’s d values, 0.78–1.10), approximately two-thirds of study subjects with military-related PTSD still met criteria for PTSD, and many retained clinically significant symptoms at posttreatment assessment (5). Some complementary therapies for PTSD have been developed, but the National Academy of Medicine (formerly the Institute of Medicine) has noted that past trials have had methodological weaknesses, such as small sample sizes and a lack of active controls (8).
The mantram repetition program has been found to mitigate PTSD symptoms and other psychological distress and to improve quality of life in a variety of populations (9). The program teaches people to intentionally slow down thoughts and to practice “one-pointed attention” by silently repeating a personalized (self-selected) mantram, a word or phrase with a spiritual meaning (10). The technique is easily used, and practice can be done inconspicuously. Mantram practice is initially recommended during nonstressful times and nightly before sleep to elicit the relaxation response, develop mindful attention (11), and reduce sleep disturbances (12). Later it is used during, and in anticipation of, triggering events or intrusive imagery to regulate emotions and to calm behavior (13).
Mantram therapy may be a valuable addition to current PTSD treatments because it incorporates some components of evidence-based treatments, yet without the trauma focus that can deter some clients. Quantitative and qualitative studies of mantram therapy delivered as a group intervention in veterans have shown significant efficacy in reducing posttraumatic stress symptom severity (13, 14), managing sleep disturbances (12), increasing mindfulness (13), and increasing levels of self-efficacy for managing PTSD symptoms (15).
Here, we report on the first randomized controlled trial of individually delivered mantram therapy compared with present-centered therapy. Present-centered therapy is a supportive, problem-solving, non-trauma-focused treatment for PTSD that has been shown to be clearly superior to a waiting list control condition (effect sizes ranging from 0.74 to 1.27) (16), and it has been used as an active control for trials of prolonged exposure and cognitive processing therapy (16–18). Our primary hypothesis was that mantram therapy would produce greater improvements in PTSD symptoms than present-centered therapy, as measured by the Clinician-Administered PTSD Scale (CAPS) (19) and the PTSD Checklist–Military (PCL-M) (20). Our secondary hypotheses were that mantram therapy would produce greater reductions in the severity of symptoms frequently associated with PTSD—insomnia, depression, and anger—and greater improvements in spiritual well-being, mindfulness, and quality of life.
Method
Design
A two-arm, two-site randomized trial was conducted at the San Diego and Bedford, Mass., Veterans Affairs Medical Centers from January 2, 2012, through March 31, 2014. Institutional review boards at both sites approved the study. All participants provided written informed consent and were randomly assigned to treatment arms by study coordinators using sealed lists of computer-generated random numbers from the study statistician. Participants taking and not taking medications prescribed for PTSD were randomized in separate blocks. The study used open allocation (participants were informed of assignment at randomization) but blinded assessment before treatment, after treatment (week 9), and at 2-month follow-up (week 17).
Participants
Self-selected treatment-seeking Veterans Health Administration patients were recruited through flyers and provider referrals. Participants were at least 18 years of age and had endorsed at least one traumatic experience related to military service. All met DSM-IV-TR criteria for PTSD, and all met symptom severity cut-off scores of ≥45 on the CAPS and ≥50 on the PCL-M. Participants who were taking medications for PTSD had been on a stable dosage (ascertained by chart review and self-report) for at least the previous 6 weeks and were instructed to continue taking their medications as prescribed. Participants were asked to refrain from receiving other psychotherapy or complementary therapy during the study.
Procedures
All participants were initially screened by telephone. Those with PCL-M scores >50 were invited for an in-person assessment. Consenting participants received the CAPS interview and completed clinical measures and demographic and medication questionnaires, and if they met the study criteria, they were enrolled prior to randomization.
Portions of the Mini International Neuropsychiatric Interview were used to exclude individuals with severe suicidal ideation, dementia, schizophrenia spectrum disorders, or untreated bipolar disorder. Participants were also excluded if they scored <25 on the Montreal Cognitive Assessment (21), ≥ 3 (for women) or ≥4 (for men) on the Alcohol Use Disorders Identification Test consumption items (22), or ≥6 on the Drug Abuse Screening Test or if they had practiced complementary therapies (e.g., mindfulness or meditation, self-hypnosis, biofeedback, yoga, tai chi) within the past 6 months. A data monitoring committee assessed the study for safety and recruitment.
Primary Outcome Measures
CAPS scores can range from zero to 136, with higher scores indicating greater severity (19). A reduction of ≥10 points is considered a clinically meaningful improvement (17). Cronbach’s alpha was 0.91. CAPS assessors had at least a master’s degree or equivalent and underwent training to competence with the CAPS senior trainer. A random sample of audio-recorded CAPS interviews was reviewed by the senior trainer and two assessors for interrater reliability. Mean intraclass correlations between raters were 0.99 for total score and 0.99, 0.99, and 0.98 for subscales for criteria B, C, and D, respectively.
Self-reported PTSD symptoms were assessed using the 17-item PCL-M (scores can range from 17 to 85, with higher scores indicating greater severity). Cronbach’s alpha was 0.92.
Secondary Outcome Measures
Insomnia symptoms were measured using the seven-item Insomnia Severity Index (scores can range from 0 to 28, with higher scores indicating greater severity; a score ≥11 traditionally indicates clinically significant insomnia) (23). Cronbach’s alpha was 0.90.
Depression was measured using the Patient Health Questionnaire–9 (scores can range from 0 to 27, with higher scores indicating greater severity) (24). Cronbach’s alpha was 0.86.
Anger was measured using the State-Trait Anger Inventory–Short Form (25) (scores can range from 10 to 40, with higher scores indicating greater severity) on each of two subscales, state anger and trait anger. Cronbach’s alpha was 0.96 for state anger and 0.89 for trait anger.
Spiritual well-being was measured using the Functional Assessment of Chronic Illness Therapy–Spiritual Well-Being questionnaire (scores can range from 0 to 48, with higher scores indicating greater spiritual well-being) (26). Sample items include “I feel peaceful” and “I have a reason for living.” Cronbach’s alpha was 0.86.
Mindfulness was measured using the Five Facet Mindfulness Questionnaire (scores can range from 39 to 195, with higher scores indicating greater mindfulness) (27). A representative item is “I find myself doing things without paying attention.” Cronbach’s alpha was 0.89.
Quality of life was assessed using the World Health Organization Quality of Life brief form (scores can range from 0 to 130; scores of 60 or more indicate higher quality of life) (28). Cronbach’s alpha was 0.87.
Frequency of mantram practice (adherence to one of three skills taught in the mantram program) was measured using self-reported mantram sessions (a session was defined as repeating a mantram at least once) at the posttreatment and follow-up assessments (see Appendix 1 in the online supplement).
Treatment Conditions
Both treatments were delivered one-on-one in eight weekly 1-hour sessions, using standardized manuals and instructor guides (Figure 1). Mantram therapy and present-centered therapy facilitators each facilitated only one treatment type. Facilitators completed 2-day trainings with role-plays and supervision in their respective treatments and received biweekly supervision (from J.E.B., senior mantram therapy expert, or Melissa Wattenberg, who contributed to the development of present-centered therapy).
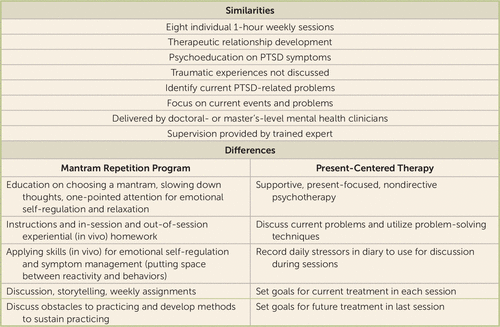
FIGURE 1. Similarities and Differences Between the Mantram Repetition Program and Present-Centered Therapy
Mantram Repetition Program
Mantram therapy is based on the premise that silently repeating a mantram (a spiritually related word or phrase selected by each individual from a recommended list) enables users to train attention, initiate relaxation, and become aware of the present moment. This skill, along with two others that are taught—“slowing down” and “one-pointed attention”—has been shown to reduce stress and increase emotional self-regulation (13–17). Participants were encouraged to practice all three skills as often as possible to interrupt stressful thoughts, feelings, or behaviors and ultimately to manage symptoms such as hyperarousal, anger, irritability, insomnia, flashbacks, and numbing/avoidance.
Present-Centered Therapy
Present-centered therapy is a manualized, supportive, present-focused psychotherapy with demonstrated efficacy for PTSD that has been used as an active comparator in other PTSD trials (18). It focuses on current events and uses techniques such as mirroring participants’ experiences and problem-solving to assist patients in dealing with current stressors. Participants are given a daily diary to record stressors to discuss with their therapists in a supportive, nondirective manner, using problem-solving techniques.
Treatment Fidelity, Credibility, and Expectancy
All treatment sessions were audio-recorded, and 15% were rated by a content expert not involved in treatment delivery using a content checklist (29). Overall, 94% of mantram therapy and 88% of present-centered therapy content items were completed. Treatment credibility and expectancy were assessed at baseline and after treatment using the Credibility/Expectancy Questionnaire (30) (see Appendix 2 in the online supplement).
Data Analysis
To provide 80% power to detect a medium-sized effect for the CAPS at an alpha of 0.05, the target sample size was estimated conservatively at 150 participants per treatment arm (by assuming that outcomes were measured just once after baseline, rather than twice). Interim analyses were not conducted, but the study ended before this sample size was attained because of funding constraints (final N=173). Baseline sociodemographic variables were summarized using means for quantitative variables and proportions for categorical variables. For all outcomes, we computed means and confidence intervals.
The primary analyses compared change in PTSD severity using CAPS and PCL-M scores at the posttreatment and 2-month follow-up assessments. Linear mixed models, using PROC MIXED in the SAS statistical package (SAS Institute, Cary, N.C.), including random intercepts, were fitted to measurements available at each time point to test whether within-subject changes in outcome variables differed by treatment condition at the posttreatment and 2-month follow-up assessments. To reduce the impact of any residual imbalances in patient characteristics, we included all baseline variables in our model, along with study site, assessment time point as a three-level categorical variable, study arm, and the interaction of assessment time with study arm. Time effects were assumed to follow an autoregressive structure to account for time dependence. Effect sizes were computed as Cohen’s d (31). The p values resulting from all primary analyses and a priori secondary analyses accounted for test multiplicity using a false discovery rate adjustment (32, 33).
Two benchmarks of residual PTSD severity were evaluated post hoc by separately examining participants who 1) no longer met PTSD criteria according to the frequency−1/intensity−2 rule for the CAPS, which is used to determine whether symptom severity is still sufficient to fulfill diagnostic criteria for PTSD (19), and 2) demonstrated a clinically meaningful improvement of ≥10 points in CAPS score (17).
Sensitivity analyses were conducted, using linear mixed models and false discovery rate adjustment (32, 33), to examine the change in outcome in specific subsets of the “as randomized” sample. The posttreatment sensitivity analyses were restricted to those individuals for whom both baseline and posttreatment assessments were available for a particular measure; similarly, the 17-week follow-up sensitivity analyses examined only those participants who contributed data at all three assessments (see Appendix 3 in the online supplement).
Results
Descriptive Analyses
We detected no significant differences between the mantram and present-centered therapy groups at baseline on any demographic characteristics, medication use, or clinical measures (Table 1) or regarding the credibility or expectations concerning the treatment (see Appendix 2 in the online supplement). Among study completers, mantram participants attended an average 7.80 of eight 1-hour sessions, and the present-centered therapy participants attended 7.75 of eight 1-hour sessions. Mantram participants who self-reported their mantram practice reported practicing an average of 6 days per week for an average of 10 sessions per day in the last week of treatment (see Appendix 1 in the online supplement). Among mantram participants, differences in self-reported mantram practice frequency over the final week of treatment was not a significant predictor of PTSD symptoms in linear models controlling for baseline measures (β=−1.84, p=0.39).
| Measure | Mantram Repetition Therapy (N=89) | Present-Centered Therapy (N=84) | ||
|---|---|---|---|---|
| N | % | N | % | |
| Male | 73 | 82 | 74 | 88 |
| Hispanic | 13 | 15 | 17 | 20 |
| Race (self-reported) | ||||
| White | 60 | 67 | 51 | 61 |
| African American | 14 | 16 | 11 | 13 |
| American Indian or Alaska Native | 2 | 2 | 4 | 5 |
| Native Hawaiian/Pacific Islander | 1 | 1 | 6 | 7 |
| Asian | 4 | 4 | 2 | 2 |
| More than one race | 8 | 10 | 10 | 12 |
| Married or partnered | 30 | 34 | 28 | 33 |
| Education | ||||
| High school or less | 23 | 26 | 20 | 24 |
| Some college | 41 | 46 | 51 | 61 |
| Bachelor’s degree or higher | 25 | 28 | 13 | 15 |
| Employment | ||||
| Full-time | 14 | 16 | 13 | 15 |
| Part-time | 4 | 4 | 9 | 11 |
| Unemployed | 71 | 80 | 62 | 74 |
| Income | ||||
| ≤$20,000 | 27 | 30 | 34 | 41 |
| $20,001–$40,000 | 35 | 40 | 22 | 26 |
| ≥$40,001 | 27 | 30 | 28 | 33 |
| Receiving medications for PTSD | 59 | 66 | 54 | 64 |
| Treatment dropoutsb | 20 | 22 | 12 | 14 |
| Mean | SD | Mean | SD | |
| Age (years) | 48.30 | 14.63 | 49.50 | 14.50 |
| Clinician-Administered PTSD Scale | 77.46 | 16.48 | 75.61 | 16.83 |
| PTSD Checklist–Military | 59.23 | 12.09 | 57.57 | 11.56 |
| Insomnia Severity Index | 18.33 | 6.59 | 16.35 | 6.43 |
| Patient Health Questionnaire–9 (depression) | 15.42 | 5.89 | 15.15 | 5.56 |
| State-Anger Inventoryc | 23.43 | 9.78 | 23.00 | 10.19 |
| Trait-Anger Inventoryc | 22.34 | 7.16 | 21.89 | 6.07 |
| Functional Assessment of Chronic Illness Therapy–Spiritual Well-Being questionnaire, 12-item scale | 21.94 | 9.79 | 22.01 | 10.89 |
| Five Facet Mindfulness Questionnaire | 116.76 | 19.56 | 118.39 | 17.33 |
| World Health Organization Quality of Life, brief form | 75.47 | 13.07 | 75.71 | 12.69 |
| Treatment credibilityd | 0.22 | 2.46 | –0.03 | 2.96 |
| Treatment expectancyd | 0.99 | 2.66 | –0.07 | 3.03 |
TABLE 1. Baseline Demographic and Clinical Characteristics of Participants in a Randomized Controlled Study of Mantram Repetition Therapy (N=173)a
Attrition after randomization did not differ significantly between the treatment arms, although participants in the mantram group had numerically higher rates of attrition than those in the present-centered therapy group at the posttreatment assessment (22% compared with 14%; χ2=1.92, p=0.16) and at the follow-up assessment (26% compared with 15%; χ2=3.93, p=0.07) (Figure 2). There were no significant baseline differences between treatment groups in baseline characteristics among participants who did not complete the study except for age (see Appendix 4 in the online supplement). Age and baseline CAPS scores also differed significantly between participants in the mantram arm who completed the treatment and those who did not (see Appendix 4). Younger age was associated with greater likelihood of dropout. There were four adverse events, all judged to be unrelated to the study protocol (e.g., substance abuse relapse and inpatient detoxification).
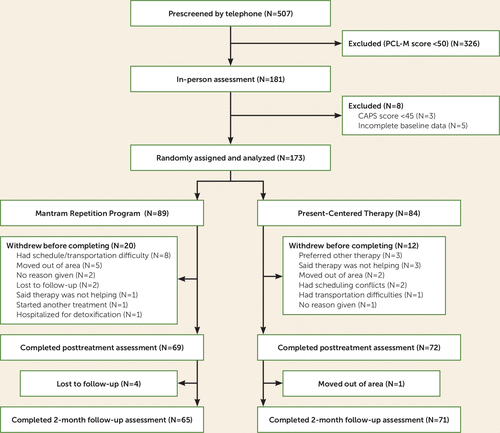
FIGURE 2. Participant Flow Diagram for a Randomized Controlled Study of Mantram Repetition Therapya
a CAPS=Clinician-Administered PTSD Scale; PCL-M=PTSD Checklist–Military.
Primary Outcome Measure
The linear mixed model, adjusted for baseline characteristics, demonstrated that participants in the mantram group had significantly greater improvements in total CAPS score at the posttreatment assessment (between-group difference across time, −9.98, 95% CI=−3.63, −16.00; false discovery rate–adjusted p=0.006, d=0.49) and at the 2-month follow-up (between-group difference across time, −9.34, 95% CI=−1.50, −17.18; false discovery rate–adjusted p=0.04, d=0.46) (Figure 3 and Table 2).
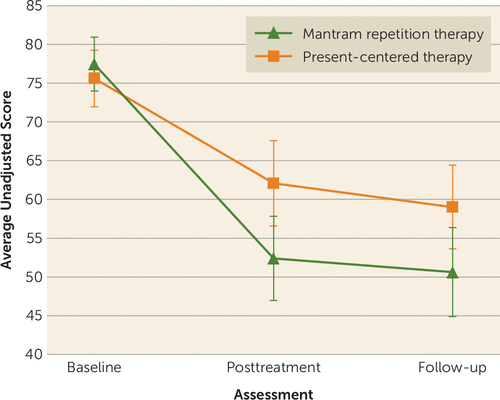
FIGURE 3. Scores Over Time on the Clinician-Administered PTSD Scale, by Group, in a Randomized Controlled Study of Mantram Repetition Therapya
a Ns at the baseline, posttreatment, and follow-up assessments, respectively, were 89, 69, and 65 for the mantram therapy group and 84, 72, and 71 for the present-centered therapy group.
| Unadjusted Outcomes | Adjusted Outcomesb | |||||||
|---|---|---|---|---|---|---|---|---|
| Mantram Repetition Therapy (N=89) | Present-Centered Therapy (N=84) | Cohen’s d | Change from Baseline in Mantram Group Compared With Present-Centered Therapy Group (N=173) | |||||
| Measure and Assessment Pointa | Mean | 95% CI | Mean | 95% CI | Mean | 95% CI | pc | |
| Clinician-Administered PTSD Scale | ||||||||
| Baseline | 77.46 | 73.99, 80.93 | 75.61 | 71.96, 79.26 | ||||
| Posttreatment assessment | 52.39 | 46.91, 57.82 | 62.07 | 56.56, 67.57 | 0.49 | –9.98 | –3.63, –16.00 | 0.006 |
| 2-month follow-up assessment | 50.61 | 44.86, 56.37 | 59.00 | 53.61, 64.39 | 0.46 | –9.34 | –1.50, –17.18 | 0.04 |
| PTSD Checklist–Military | ||||||||
| Baseline | 59.23 | 56.52, 61.84 | 57.57 | 54.98. 60.16 | ||||
| Posttreatment assessment | 45.32 | 41.63, 49.02 | 50.20 | 46.88, 53.52 | 0.43 | –5.83 | –1.73, –9.93 | 0.04 |
| 2-month follow-up assessment | 44.74 | 41.00, 48.47 | 48.42 | 44.76, 52.09 | 0.33 | –4.51 | 0.70, –9.72 | 0.25 |
| Insomnia Severity Index | ||||||||
| Baseline | 18.33 | 16.93, 19.74 | 16.35 | 14.94, 17.75 | ||||
| Posttreatment assessment | 14.22 | 12.40, 16.05 | 16.62 | 15.06, 18.17 | 0.59 | –4.13 | –2.19, –6.07 | 0.002 |
| 2-month follow-up assessment | 12.74 | 10.71, 14.76 | 15.92 | 14.22, 17.64 | 0.69 | –4.81 | –2.30, –7.32 | 0.004 |
| Patient Health Questionnaire–9, depression | ||||||||
| Baseline | 15.42 | 14.17, 16.67 | 15.15 | 13.92, 16.38 | ||||
| Posttreatment assessment | 10.68 | 9.16, 12.20 | 12.81 | 11.53, 14.09 | 0.31 | –1.85 | –0.32, –3.38 | 0.10 |
| 2-month follow-up assessment | 10.51 | 8.87, 12.14 | 12.18 | 10.69, 13.67 | 0.21 | –1.26 | 0.74, –3.26 | 0.49 |
| State angerd | ||||||||
| Baseline | 23.43 | 21.34, 25.51 | 23.00 | 20.76, 25.24 | ||||
| Posttreatment assessment | 21.21 | 19.12, 23.30 | 22.20 | 19.81, 24.58 | 0.11 | –1.02 | 2.37, –4.41 | 0.77 |
| 2-month follow-up assessment | 21.22 | 18.85, 23.59 | 21.27 | 19.28, 23.27 | 0.03 | –0.30 | 3.62, –4.22 | 0.99 |
| Trait angerd | ||||||||
| Baseline | 22.34 | 20.82, 23.87 | 21.89 | 20.57, 23.22 | ||||
| Posttreatment assessment | 20.90 | 19.20, 22.59 | 20.37 | 18.89, 21.84 | 0.03 | –0.17 | 1.44, –1.78 | 0.98 |
| 2-month follow-up assessment | 19.53 | 17.78, 21.29 | 18.62 | 17.24, 20.01 | 0.06 | –0.38 | 1.76, –2.52 | 0.93 |
| FACIT-SP-12e total score | ||||||||
| Baseline | 21.94 | 19·84, 24·04 | 22.01 | 19.59, 24.44 | ||||
| Posttreatment assessment | 25.56 | 23.29, 27.83 | 23.29 | 21.09, 25.48 | 0.24 | 2.39 | 4.92, –0.14 | 0.19 |
| 2-month follow-up assessment | 25.68 | 23.19, 28.17 | 24.75 | 22.12, 27.39 | 0.10 | 1.04 | 4.39, –2.31 | 0.77 |
| FFMQ total scoref | ||||||||
| Baseline | 116.76 | 112.59, 120.93 | 118.39 | 114.58, 122.20 | ||||
| Posttreatment assessment | 121.34 | 116.31, 126.37 | 119.00 | 114.31, 123.69 | 0.13 | 2.34 | 6.81, –2.13 | 0.59 |
| 2-month follow-up assessment | 120.43 | 114.9, 125.97 | 121.29 | 116.18, 126.41 | 0.001 | 0.02 | 5.98, –5.94 | 0.99 |
| WHOQOL-BREFg | ||||||||
| Baseline | 75.02 | 71.71, 78.32 | 75.24 | 71.94, 78.54 | ||||
| Posttreatment assessment | 80.87 | 77.39, 84.34 | 76.92 | 73.41, 80.43 | 0.31 | 3.95 | 7.26, 0.64 | 0.10 |
| 2-month follow-up assessment | 80.18 | 76.82, 83.55 | 77.71 | 73.73, 81.68 | 0.24 | 3.01 | 7.36, –1.34 | 0.45 |
TABLE 2. Unadjusted Means, Confidence Intervals, Effect Sizes, and Main Analyses of Change From Baseline in Mantram Repetition Program Compared With Present-Centered Therapy (N=173)
For self-reported PTSD symptoms on the PCL-M, a significant difference between treatment groups was observed at the posttreatment assessment (−5.83, 95% CI=−1.73, −9.93; false discovery rate–adjusted p=0.04, d=0.43) but not at the 2-month follow-up assessment (−4.51, 95% CI=0.70, −9.72; false discovery rate–adjusted p=0.25, d=0.25) (Table 2). A significant difference favoring mantram therapy was observed among participants who completed the 2-month follow-up assessment and no longer met criteria for PTSD (59% of the mantram group [N=36] compared with 40% of the present-centered therapy group [N=26]; χ2=4.55, p<0.04). No significance difference was observed immediately after treatment (48% of the mantram group [N=32] compared with 35% of the present-centered therapy group [N=24]; χ2=2.16, p<0.14). The percentage of participants who experienced clinically meaningful improvements of ≥10 points in CAPS score did not differ significantly between treatment groups (75% of the mantram group [N=49] compared with 61% of the present-centered therapy group [N=43]; odds ratio=1.67, 95% CI=0.73, 3.81).
Secondary Outcome Measures
There were significant group-by-time improvements in Insomnia Severity Index score in the mantram group compared with the present-centered therapy group at the posttreatment assessment (false discovery rate–adjusted p<0.05, Cohen’s d=0.59) and at the 2-month follow-up assessment (false discovery rate–adjusted p<0.001, d=0.69) (Table 2). Both the mantram and present-centered therapy groups improved on all remaining outcome measures, with no significant between-group differences (Table 2).
Sensitivity analyses examining outcomes among participants with assessments both at baseline and after treatment, or at all three assessments, are presented in Appendix 3 in the online supplement.
Discussion
In this randomized trial of 173 veterans receiving non-trauma-focused interventions, mantram repetition therapy was associated with greater reductions in the clinician-rated primary outcome measure (the CAPS) at the posttreatment and 2-month follow-up assessments than present-centered therapy, with a moderate effect size at both time points. Mantram therapy was also associated with greater reductions in self-reported PTSD symptom severity (on the PCL-M) at the posttreatment assessment but not at the 2-month follow-up assessment. More mantram participants no longer met criteria for a PTSD diagnosis at the 2-month follow-up. The proportion of participants with a reduction of ≥10 points in CAPS score did not differ between treatment arms. Finally, mantram therapy was associated with moderate effect-size reductions in insomnia at both time points.
This is the first randomized trial to demonstrate the efficacy of mantram therapy delivered individually compared with an active comparison treatment. Mantram therapy delivered individually appears to be more effective than the group format used in previous studies (12–14). This finding is consistent with a meta-analysis showing that, for veterans, group-only formats tend to perform worse than individual treatment formats for PTSD treatment (34).
This trial’s design addressed frequent criticisms of complementary therapy research, including the absence of an active comparison arm to control for nonspecific effects of therapy. Our findings add to the literature showing that non-trauma-focused therapies for PTSD can yield substantial improvements in PTSD symptoms (16, 35). Mantram therapy is also briefer than some other PTSD psychotherapies, and we observed a 78% retention rate during active mantram treatment. Previous studies suggest that mantram therapy may help individuals with PTSD by reducing reactivity and initiating relaxation (14). Mantram therapy also includes a spiritual component; however, we observed no significant differences in the total scores of our spirituality or mindfulness measures when mantram therapy was compared with present-centered therapy, which suggests that mantram therapy’s benefits in this trial may stem from other aspects of the treatment.
Study strengths included clinician-blinded ratings of PTSD using a gold-standard assessment measure (the CAPS), patient-reported ratings of PTSD using a psychometrically strong questionnaire, clinically important secondary analyses (anger, quality of life, and insomnia—sleep problems are among the top reasons returning troops seek PTSD treatment) (36), adjustment for multiple comparisons for both the primary and secondary outcome analyses, stratification of our randomization by medication use for PTSD, the inclusion of covariates in the linear mixed models to address even modest imbalances in baseline characteristics, collection of data concerning treatment credibility/expectancy and frequency of mantram practice, and treatments of equal length (eight sessions) and therapist time (1-hour sessions) using standardized guidelines. In fact, because slightly fewer participants completed mantram therapy than present-centered therapy, average total time spent with a therapist would be expected to be slightly greater for the present-centered therapy group.
Study limitations include a smaller sample size than our original goal, self-report ratings for some endpoints (e.g., insomnia), the possibility that participants had received prolonged exposure or other trauma-focused therapy prior to enrollment, the lack of a measure of therapist alliance, and assessment of outcomes at only two postrandomization time points. Thus, inferences concerning longer-term improvements in PTSD symptoms cannot be made. Our assessment of fidelity (only 15% of treatment sessions, reviewed by a single rater) was also limited compared with some other studies, and fidelity was slightly greater for mantram therapy content (94%) than for present-centered therapy content (88%). Our data on mantram practice were collected in the last week of treatment (see Appendix 1 in the online supplement) and were restricted to subsets of participants who completed treatment and completed the study; future research might more intensively investigate practice frequency over time and examine how mantram practice is related to outcomes.
Because our study did not have a waiting list control condition, it is not possible to exclude the possibility that, even though present-centered therapy has an evidence base as an effective treatment for PTSD (16), it might have been delivered in this study in a manner that unintentionally provided less effective PTSD symptom relief. We sought to minimize this possibility by using facilitators who exclusively delivered present-centered therapy and who received supervision from a present-centered therapy expert. However, while present-centered therapy has been found in multiple trials to be superior to a waiting list condition, these studies have examined present-centered therapy delivered over longer periods than the eight 1-hour session format used here (37, 38). Present-centered therapy participants in our trial did experience a posttreatment improvement in CAPS score (mean decrease, 13.5 points; see Table 2). However, this change is less than the 20.5- to 22.2-point decreases in CAPS score observed in trials where present-centered therapy was demonstrated to be superior to a waiting list control condition (37, 38) and the 15.2- to 17.8-point decreases in CAPS score observed for present-centered therapy when it was used as an active comparator in studies of cognitive processing therapy or prolonged exposure (18, 39).
Few trials have identical attrition between study arms, and while our attrition was not significantly different between treatments, attrition during treatment was somewhat greater in the mantram group (22%) than in the present-centered therapy group (14%). Our linear mixed models used only data on participants who completed treatment, which was all the data available in the study, so if individuals who responded less well to treatment were more likely to stop treatment, this may have biased results to an uncertain extent in favor of mantram therapy. Based on expressed reasons for study noncompletion (see Figure 2), it did not appear that more participants were dropping out of mantram therapy for a lack of treatment response (e.g., only one individual, compared with three in the present-centered therapy arm, cited “lack of treatment response”). Baseline CAPS scores for those who did not complete mantram therapy were significantly higher than for those who did.
While the study included an active control condition, it did not compare mantram therapy with cognitive processing therapy or prolonged exposure, two evidence-based psychotherapies currently used by the Veterans Health Administration for PTSD treatment. The effect size for the baseline-to-posttreatment change in CAPS for the 8-week course of mantram therapy compared with present-centered therapy examined in this trial (d=0.49) is generally similar to or greater than the effect sizes observed for prolonged exposure and cognitive processing therapy when compared with present-centered therapy (see Appendix 5 in the online supplement). However, there are a number of differences between our trial and those trials (see above and Appendix 5), including the duration of present-centered therapy treatment delivered and different participant populations (e.g., the participant groups for those other studies were predominantly female). It would be premature to draw any conclusions about the efficacy of mantram therapy compared with these established treatments, or other treatments, without head-to-head trials.
Finally, our veteran sample was self-selected, reported limited substance abuse, and was drawn from only two centers, located in the East and West Coast areas of the United States. The study findings may not generalize to different veteran samples, nonmilitary samples, or other geographical locations where religious and cultural beliefs may differ. In the future, studies of broader patient samples or varying designs could be considered (see Appendix 6 in the online supplement).
Conclusions
The individually delivered mantram repetition program demonstrated greater reductions in PTSD symptom severity and insomnia for veterans compared with present-centered therapy. Further assessment of mantram therapy in trials and real-world settings is clearly desirable, especially because mantram therapy may appeal to some veterans who may prefer therapies that are not trauma-focused, that include some element of spirituality, or that reduce sleep disturbances.
Patient Perspectives
One participant’s comment on repeating a mantram to deal with a trauma-related incident: “[Mantram repetition] provides more of a calming sensation than anything else. Mantram repetition took the edge off of the feelings that I had about the incident and caused me to reflect on it more, and it kind of saved me from a heart attack, that situation, really. You can get, you know, so tied into these things to where they build up and build up and build up, and the mantram helps me take the edge off of it and wipe the situation back down so it’s not as disturbing to my system, not only emotionally but physically as well.”
Another participant reported using mantram repetition for insomnia: “On days I don’t use my sleep medication, those are the days when I use my mantram, and that’s when I wake up at night . . . on those frequent nights, which is a couple times a week . . . I will use the mantram and it works.”
A participant who was assigned to the mantram intervention and decided to drop out after attending three sessions stated: “I’ve been trying to come up with a mantram but I just can’t get myself to do this. I have so many other appointments … and I’m feeling really overwhelmed. I just don’t see how mantram is going to help me.”
1 : Returning Home from Iraq and Afghanistan: Assessment of Readjustment Needs of Veterans, Service Members, and their Families. Washington, DC, National Academies Press, 2013Google Scholar
2 : Trauma and the Vietnam War Generation: Report of Findings From the National Vietnam Veterans Readjustment Study. New York, Brunner/Mazel, 1990Google Scholar
3 : Psychological therapies for chronic post-traumatic stress disorder (PTSD) in adults. Cochrane Database Syst Rev 2013; (12):CD003388Medline, Google Scholar
4 : Psychological treatments for adults with posttraumatic stress disorder: a systematic review and meta-analysis. Clin Psychol Rev 2016; 43:128–141Crossref, Medline, Google Scholar
5 : Psychotherapy for military-related PTSD: a review of randomized clinical trials. JAMA 2015; 314:489–500Crossref, Medline, Google Scholar
6 : A randomized controlled trial of 7-day intensive and standard weekly cognitive therapy for PTSD and emotion-focused supportive therapy. Am J Psychiatry 2014; 171:294–304Link, Google Scholar
7 : A multisite randomized controlled effectiveness trial of cognitive processing therapy for military-related posttraumatic stress disorder. J Anxiety Disord 2012; 26:442–452Crossref, Medline, Google Scholar
8 : Treatment for Posttraumatic Stress Disorder in Military and Veteran Populations: Initial Assessment. Washington, DC, National Academies Press, 2012Google Scholar
9 : Mantram repetition, in Annual Review of Nursing Research: Military and Veteran Innovations of Care, 32. Edited by Kasper K, Kelley PW. New York, Springer, 2014, pp 79–108Google Scholar
10 : Strength in the Storm. Tomales, Calif, Nilgiri Press, 2013Google Scholar
11 : Mindful attention increases and mediates psychological outcomes following mantram repetition practice in veterans with posttraumatic stress disorder. Med Care 2014; 52(12 suppl 5):S13–S18Crossref, Medline, Google Scholar
12 : Efficacy of the mantram repetition program for insomnia in veterans with posttraumatic stress disorder: a naturalistic study. ANS Adv Nurs Sci 2017; 40:E1–E12Crossref, Medline, Google Scholar
13 : Responses to mantram repetition program from veterans with posttraumatic stress disorder: a qualitative analysis. J Rehabil Res Dev 2013; 50:769–784Crossref, Medline, Google Scholar
14 : Meditation-based mantram intervention for veterans with posttraumatic stress disorder: a randomized trial. Psychol Trauma 2013; 5:259–267Crossref, Google Scholar
15 : Mantram repetition fosters self-efficacy in veterans for managing PTSD: a randomized trial. Psychol Relig Spiritual 2015; 7:34–45Crossref, Google Scholar
16 : The evidence for present-centered therapy as a treatment for posttraumatic stress disorder. J Trauma Stress 2014; 27:1–8Crossref, Medline, Google Scholar
17 : Randomized trial of trauma-focused group therapy for posttraumatic stress disorder: results from a Department of Veterans Affairs cooperative study. Arch Gen Psychiatry 2003; 60:481–489Crossref, Medline, Google Scholar
18 : Cognitive behavioral therapy for posttraumatic stress disorder in women: a randomized controlled trial. JAMA 2007; 297:820–830Crossref, Medline, Google Scholar
19 : Clinician-Administered PTSD Scale: a review of the first ten years of research. Depress Anxiety 2001; 13:132–156Crossref, Medline, Google Scholar
20 : PTSD Checklist (PCL): reliability, validity, and diagnostic utility. Proceedings of the 9th Annual Conference of the International Society for Traumatic Stress Studies. Chicago, 1993Google Scholar
21 : The Montreal Cognitive Assessment, MoCA: a brief screening tool for mild cognitive impairment. J Am Geriatr Soc 2005; 53:695–699Crossref, Medline, Google Scholar
22 : The Alcohol Use Disorders Identification Test (AUDIT) as a screen for at-risk drinking in primary care patients of different racial/ethnic backgrounds. Addiction 1997; 92:197–206Crossref, Medline, Google Scholar
23 : The Insomnia Severity Index: psychometric indicators to detect insomnia cases and evaluate treatment response. Sleep (Basel) 2011; 34:601–608Crossref, Medline, Google Scholar
24 : The PHQ-9: validity of a brief depression severity measure. J Gen Intern Med 2001; 16:606–613Crossref, Medline, Google Scholar
25 : Assessment of anger: the state-trait anger scale, in Advances in Personality Assessment, vol 2. Edited by Butcher JN, Spielberger CD. Hillsdale, NJ, Lawrence Erlbaum Associates, 1983, pp 159–187Google Scholar
26 : Validation of the Functional Assessment of Chronic Illness Therapy–Spiritual Well-Being scale in veterans with PTSD. Spiritual Clin Pract 2015; 2:25–35Crossref, Google Scholar
27 : Using self-report assessment methods to explore facets of mindfulness. Assessment 2006; 13:27–45Crossref, Medline, Google Scholar
28 : The World Health Organization’s WHOQOL-BREF quality of life assessment: psychometric properties and results of the international field trial: a report from the WHOQOL group. Qual Life Res 2004; 13:299–310Crossref, Medline, Google Scholar
29 : Testing the integrity of a psychotherapy protocol: assessment of adherence and competence. J Consult Clin Psychol 1993; 61:620–630Crossref, Medline, Google Scholar
30 : Psychometric properties of the Credibility/Expectancy Questionnaire. J Beh Ther Exp Psychiatry 2000; 31:73–86Crossref, Medline, Google Scholar
31 : Statistical Power Analysis for the Behavioral Sciences, 2nd ed. Hillsdale, NJ, Erlbaum, 1988Google Scholar
32 : Controlling the false discovery rate: a practical and powerful approach to multiple testing. J R Stat Soc B 1995; 57:289–300Google Scholar
33 : False discovery rate control is a recommended alternative to Bonferroni-type adjustments in health studies. J Clin Epidemiol 2014; 67:850–857Crossref, Medline, Google Scholar
34 : Treatment of posttraumatic stress disorder in US combat veterans: a meta-analytic review. Psychol Rep 2011; 109:573–599Crossref, Medline, Google Scholar
35 : Is exposure necessary? A randomized clinical trial of interpersonal psychotherapy for PTSD. Am J Psychiatry 2015; 172:430–440Link, Google Scholar
36 : Presenting concerns of veterans entering treatment for posttraumatic stress disorder. J Trauma Stress 2013; 26:640–643Crossref, Medline, Google Scholar
37 : Randomized trial of cognitive-behavioral therapy for chronic posttraumatic stress disorder in adult female survivors of childhood sexual abuse. J Consult Clin Psychol 2005; 73:515–524Crossref, Medline, Google Scholar
38 : A randomized clinical trial comparing affect regulation and social problem-solving psychotherapies for mothers with victimization-related PTSD. Behav Ther 2011; 42:560–578Crossref, Medline, Google Scholar
39 : A randomized clinical trial of cognitive processing therapy for veterans with PTSD related to military sexual trauma. J Trauma Stress 2013; 26:28–37Crossref, Medline, Google Scholar



