Nonpharmacological Interventions for ADHD: Systematic Review and Meta-Analyses of Randomized Controlled Trials of Dietary and Psychological Treatments
Abstract
Objective
Nonpharmacological treatments are available for attention deficit hyperactivity disorder (ADHD), although their efficacy remains uncertain. The authors undertook meta-analyses of the efficacy of dietary (restricted elimination diets, artificial food color exclusions, and free fatty acid supplementation) and psychological (cognitive training, neurofeedback, and behavioral interventions) ADHD treatments.
Method
Using a common systematic search and a rigorous coding and data extraction strategy across domains, the authors searched electronic databases to identify published randomized controlled trials that involved individuals who were diagnosed with ADHD (or who met a validated cutoff on a recognized rating scale) and that included an ADHD outcome.
Results
Fifty-four of the 2,904 nonduplicate screened records were included in the analyses. Two different analyses were performed. When the outcome measure was based on ADHD assessments by raters closest to the therapeutic setting, all dietary (standardized mean differences=0.21–0.48) and psychological (standardized mean differences=0.40–0.64) treatments produced statistically significant effects. However, when the best probably blinded assessment was employed, effects remained significant for free fatty acid supplementation (standardized mean difference=0.16) and artificial food color exclusion (standardized mean difference=0.42) but were substantially attenuated to nonsignificant levels for other treatments.
Conclusions
Free fatty acid supplementation produced small but significant reductions in ADHD symptoms even with probably blinded assessments, although the clinical significance of these effects remains to be determined. Artificial food color exclusion produced larger effects but often in individuals selected for food sensitivities. Better evidence for efficacy from blinded assessments is required for behavioral interventions, neurofeedback, cognitive training, and restricted elimination diets before they can be supported as treatments for core ADHD symptoms.
Attention deficit hyperactivity disorder (ADHD) is a common disorder that, although most frequently diagnosed during the school years, affects individuals across the lifespan (1). It is characterized by symptoms of inattention, overactivity, and/or impulsiveness that are age inappropriate, persistent, and pervasive (2). In the long term, ADHD is associated with a significant risk of educational failure, interpersonal problems, mental illness, and delinquency (3), creating a substantial burden on families as well as on health, social care, and criminal justice systems (4). Multimodal approaches are recommended for the treatment for ADHD (5), which normally begins during the school years. Pharmacological treatments are efficacious (6) and are widely used but may be limited in a number of ways: normalization is rare (6); long-term effectiveness remains to be established (7); adverse effects on sleep, appetite, and growth, although rarely serious, are common (8); and some parents and clinicians have reservations about medication use (9). A variety of nonpharmacological interventions are available to treat ADHD, and evidence for their efficacy has been supported in systematic reviews and meta-analyses (10–14). However, interpreting these reports, specifically in relation to impact on core ADHD symptoms, is complicated by the inclusion of trials using nonrandomized designs, non-ADHD samples, or non-ADHD outcome measures. Furthermore, estimates of efficacy are often based on assessments made by individuals who are likely to be aware of study allocation, which may inflate effect sizes (15).
Our aim was to address these limitations in six meta-analyses of randomized controlled trials to assess the effects of dietary and psychological treatments on ADHD symptoms for patients 3 to 18 years of age who had an ADHD diagnosis or met recognized symptom thresholds. This is the first meta-analysis to include both dietary and psychological domains of ADHD treatments. Our goal was to survey the field to prepare evidence-based clinical guidelines for the nonpharmacological treatment of ADHD. To build evidence-based guidelines, we needed to have a sense of the efficacy of treatments across domains using equivalent and equally stringent inclusion criteria and statistical approaches. Previous reviews have adopted very different approaches for the different domains, reflecting differences in research cultures. While recognizing the importance of other outcomes (e.g., oppositional symptoms) as treatment targets for children with ADHD, analyses of such measures were not viable in this study because an insufficient number of studies across the domains included these outcomes.
Our analyses covered three dietary domains—restricted elimination diets (exclusion of items associated with food hypersensitivity) (16), artificial food color exclusions (10), and free fatty acid supplementation (11)—and three psychological domains—cognitive training incorporating adaptive schedules that are hypothesized to strengthen ADHD-deficient neuropsychological processes (e.g., working memory) (12), neurofeedback using the visualization of brain activity to teach children to increase attention and impulse control (13), and behavioral interventions employing learning principles to target ADHD-related behaviors directly with the child or indirectly via an adult (14, 17). To address the issue of assessment blinding while at the same time allowing comparison with the results of previous reviews that included unblinded studies, we conducted two analyses. The first used a score from the rater (often unblinded) closest to the therapeutic setting. These ratings typically constituted a trial’s own primary outcome measure and were therefore the assessment most available for analysis. They were termed the most proximal assessment. The second analysis was restricted to trials with a probably blinded assessment—either ratings clearly made under blind conditions (e.g., in a placebo-controlled trial) or ratings made by an adult unlikely to be aware of treatment allocation. This second analysis was considered especially important if the person responsible for the most proximal assessment either was involved in the delivery of the treatment—particularly where this involved a major investment of their own personal resources (e.g., it would be only natural for parents who had invested a lot of time and effort in parent training to overemphasize its beneficial effects)—or had strong beliefs about the efficacy of a particular treatment outcome (e.g., parents who believe in the importance of diet in ADHD may be especially likely both to volunteer for dietary trials and to rate the effects of the intervention positively).
Method
The review protocol is registered at PROSPERO (registration number CRD42011001393; http://www.crd.york.ac.uk/prospero/).
Inclusion Criteria
We included randomized controlled trials (including studies with counterbalanced crossover designs) that were published in peer-reviewed journals at any time from the inception of the databases. We limited our search to published trials to ensure a level of methodological adequacy and rigor among included trials and to avoid the inevitable problems with securing access to a full set of unpublished trials and the bias that this would introduce (18). Participants (ages 3 to 18 years) had a diagnosis of ADHD of any subtype (DSM-defined ADHD or ICD-defined hyperkinetic disorder, as well as historic variants; we excluded minimal brain dysfunction) or met accepted criteria for clinical levels of symptoms on validated ADHD rating scales. Studies had to have an appropriate control condition. For studies that used two control conditions, we selected the most stringent, in the following order: sham/placebo, attention/active control, treatment as usual, waiting list. Treatment as usual could include medication, but trials were excluded if the nonpharmacological therapy was an adjunct to medication or if both interventions were combined into one therapeutic arm as part of the study design. For instance, studies evaluating the additional benefit of nonpharmacological therapies to already effective medication were excluded. Because allowing medication in treatment as usual may have reduced effect sizes for the nonpharmacological comparator, we conducted sensitivity analyses to compare effect sizes for those trials with low/no medication. Studies in which enrollment depended on the presence of rare comorbid conditions (e.g., fragile X syndrome) were excluded.
Search Strategy
A common search strategy was employed for all treatment domains, using a broad range of electronic databases: Science Citation Index Expanded; Social Sciences Citation Index; Arts and Humanities Citation Index; Conference Proceedings Citation Index–Science; Conference Proceedings Citation Index–Social Sciences and Humanities; Index Chemicus; Current Chemical Reactions; Current Contents Connect; Derwent Innovations Index; Biological Abstracts; BIOSIS Previews; CAB Abstracts and Global Health (both from CABI); Food Science and Technology Abstracts; Inspec; MEDLINE; Zoological Record; Ovid MEDLINE; PsycINFO; EMBASE Classic+EMBASE; Web of Science; ERIC; and CINAHL. Articles written in English, German, Spanish, Dutch, and Chinese were included in the search. Common terms for participants (e.g., all variants of ADHD, hyperkinetic disorder, attention deficit) and study design terms were used across domains. The design terms were randomized controlled trial(s); cluster randomized controlled trial(s); clinical trial; controlled clinical trial; crossover procedure or crossover study; crossover design; double blind procedure; double blind method; double blind study; single blind procedure; single blind method; single blind study; random allocation; randomization; random assignment; and randomized controlled trial. Separate treatment terms were used: 1) restricted elimination diet: few foods diet, elimination diet, oligoantigenic diet, restriction diet, food intolerance, food allergy, and food hypersensitivity; 2) artificial food color elimination: food color, food dye, Feingold diet, Kaiser Permanente diet, K-P diet, tartrazine, azo dye, carmoisine, sunset yellow, brilliant blue, indigotine, allura red, quinoline yellow, and ponceau 4R; 3) free fatty acid supplementation: essential fatty acid, long-chain polyunsaturated fatty acids, omega-3, omega-6, docosahexaenoic acid, eicosapentaenoic acid, and arachidonic acid; 4) cognitive training: cognitive training, attention training, working memory training, cognitive remediation, executive function training, and cognitive control; 5) neurofeedback: neurofeedback, EEG biofeedback, neurotherapy, and slow cortical potentials; and 6) behavioral interventions: contingency management, management techniques, contingency techniques, psychosocial interventions, psychosocial treatment, psychosocial therapy, social skills training, social skills intervention, social skills treatment, problem solving intervention, problem solving treatment, problem solving training, problem solving therapy, behavior modification, cognitive behavior treatment, cognitive behavior therapy, cognitive behavior training, parent training, parent counseling, parent support, school-based, classroom-based, school intervention, classroom intervention, teacher training, after-school or remedial teaching, peer tutoring, computer assistance learning, task modification, curriculum modification, classroom management, education intervention, multimodal intervention, multimodal treatment, multimodal therapy, multimodal intervention, multimodal treatment, multimodal therapy, educational intervention, and verbal self-instruction training. Our search terms for behavioral interventions covered a wide variety of intervention types with the aim of being as thorough as possible. However, in the end all the trials that met our criteria involved some element of behavioral training based on social learning or operant techniques. For the specific syntax and language specific formulations used in different databases, see the published study protocol. Database searches were supplemented by manual searches of published reviews. Two coauthors (S. Cortese and M. Ferrin) separately conducted and cross-checked all searches, which were finalized on April 3, 2012.
Outcome Measure
The outcome measure was pre- to posttreatment change in total ADHD symptom severity measured at the first posttreatment assessment. Results from ADHD-specific symptom scales were used where available (e.g., the DSM-IV ADHD subscale of Conners’ Parent and Teacher Rating Scales) (19). We also permitted questionnaire measures of ADHD-related dimensions (e.g., inattention on Rutter parents’ and teachers’ scales [20]) as well as direct observations.
Study Selection
Trials were blindly double-coded for eligibility. Articles were initially screened on the basis of titles and abstracts, and assessment of articles for final inclusion was based on full text. Disagreements not resolved by coders (N=6) were arbitrated by either of two authors (E. Sonuga-Barke or J. Sergeant) who were independent of the domain specific work groups. The process was independently validated by another author (E. Simonoff) on the basis of “near miss” cases. Study quality was assessed by two independent raters (with disagreements resolved by E. Simonoff) using the standard definitions for randomization, blinding, and treatment of missing data provided by Jadad et al. (21).
Data Extraction
Sample and design information of included trials were entered into RevMan, version 5.0 (http://ims.cochrane.org/revman) to provide a systematic record of study features (22). Data were extracted by a single person in each domain and independently checked by another. See the published protocol for a list of data extracted.
Statistical Analysis
Individual effect sizes (the standardized mean difference) were based on the recommended formula: mean pre- to posttreatment change minus the mean pre- to posttreatment control group change divided by the pooled pretest standard deviation with a bias adjustment (23). Crossover trials were treated as parallel group trials because insufficient data were provided to permit analysis of within-individual change (e.g., there were no correlations of scores between conditions). This is a conservative approach, equivalent to setting the between-condition correlation to zero (24). In this case, the pretest (baseline) standard deviation was used as the denominator in the calculation of the standardized mean difference. When necessary, missing standard deviations were imputed separately for each of the outcome measures. The reported pretest standard deviations for each outcome measure were pooled across trials, and the value at the third quartile was adopted for studies with missing standard deviation values (25). Standardized mean differences for trials in each domain were combined using the inverse-variance method, in which the reciprocal of their variance is used to weight the standardized mean difference from each trial before being combined to give an overall estimate (26). Given the heterogeneity of ADHD assessments, sample characteristics, and implementation of treatments within domains in the included studies, we chose a priori to use random-effects models, as recommended by Field and Gillett (27). The I2 statistic was calculated, a posteriori, as an estimate of between-trial heterogeneity in standardized mean difference, although given the number of trials included, the power to detect heterogeneity in these analyses is relatively low (28).
The most proximal assessment analysis used a report by the rater closest to the therapeutic setting as the outcome measure (i.e., parent ratings except for teacher-based interventions when teacher ratings or direct observations were used). If ratings of total ADHD symptoms (inattention, hyperactivity, and impulsivity) were not reported, then the next most appropriate available measure was used (e.g., ratings of one ADHD dimension). Ratings of non-ADHD-related dimensions were not included in the analyses. The probably blinded assessment analysis included both placebo- and non-placebo-controlled trials with an ADHD assessment made by an individual likely to be blind to treatment. In trials in which more than one such measure was available, the best blinded measure was selected. In nonplacebo or sham-treatment designs implemented in the home, these were either direct observations by an independent researcher or teacher ratings, as parent ratings were not considered probably blinded assessments. If the intervention was implemented at school, teacher ratings were not considered probably blinded assessments. When two measures were available, we considered independent direct observation as the best probably blinded assessment measure. In placebo or sham-treatment controlled trials, where all measures were likely to have some degree of blinding, parent ratings (home-implemented) and teacher ratings (school-implemented) were considered probably blinded assessments. For home-based interventions, direct observation or teacher ratings (in that order of preference) were considered better probably blinded assessments. Of the included studies, 93% of dietary and 54% of psychological trials had probably blinded assessments. Sensitivity analyses examined the impact of background ADHD medication use in trial samples on probably blinded assessments for which at least three trials in a domain had less than 30% of participants receiving medications (i.e., were no/low medication trials). Random-effects meta-regression was used to test whether lower-quality trials (as represented by total Jadad score) had larger effect sizes. Given the relatively small number of methodologically sound studies, the field is not yet mature enough for the investigation of publication bias using funnel plots—the interpretation of which, moreover, is equivocal when based on a small number of studies (29). In addition, it is problematic to distinguish between the effects of study heterogeneity and publication bias with sparse data (30).
Results
Figure 1 is a combined flow chart describing trial selection. (For domain-specific flow charts and individual justifications for the decision to exclude trials, see section I of the data supplement that accompanies the online edition of this article.) Overall, a higher proportion of behavioral interventions failed to meet the entry criteria for the present study than any other treatment domain, typically because of design limitations. Table 1 provides information about the retained trials, including overall Jadad ratings (for a detailed breakdown of Jadad scores, see section II of the online data supplement). Figures 2 and 3 present forest plots and their associated statistics.
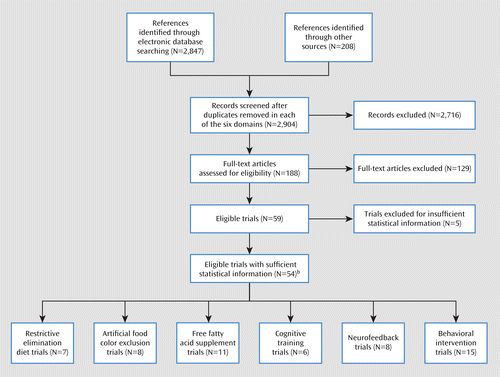
a PRISMA=Preferred Reporting Items for Systematic Reviews and Meta-Analyses (www.prisma-statement.org).
b Data from one three-arm trial are included in both neurofeedback and cognitive training analyses.
| Numbers Randomized | Characteristics | ADHD Measure | |||||||
|---|---|---|---|---|---|---|---|---|---|
| First Author (Reference) | Treatment | Control | Reported Design Qualityb | Treatment | Control | Age (Years; Mean or Range) | Male (%) | Most Proximal Assessment | Probably Blinded Assessment |
| Restricted elimination diets | |||||||||
| Pelsser (16) | Elimination diet | Waiting list | 3 | 50 | 50 | 3–9 | 86 | P-ARS | None |
| Boris (31) | Known antigenic foods | Placebo | 5 | 16 | 16 | 7.5 | 69 | CPRS | CPRS |
| Kaplan (32) | Known antigenic foods | Placebo | 3 | 25 | 25 | 3–6 | 100 | CPRS | CTRS |
| Carter (33) | Specific provoking food | Placebo | 5 | 19 | 19 | 3–12 | 74 | CPRS | Test session observation |
| Egger (34) | Specific provoking food | Placebo | 5 | 31 | 31 | 3–12 | 88 | Psychologist rating | Psychologist rating |
| Pelsser (35) | Elimination diet | Waiting list | 3 | 15 | 12 | 3–9 | 81 | CPRS | None |
| Schmidt (36) | Oligoantigenic diet | Control diet | 4 | 49 | 49 | 7–12 | 96 | CTRS | CTRS |
| Artificial food color exclusions | |||||||||
| Goyette (37)c | Certified food colors | Placebo | 1 | 17 | 17 | 4–12 | n.a. | CPRS | CTRS |
| Goyette (37)d | Certified food colors | Placebo | 1 | 13 | 13 | 3–10 | n.a. | CPRS | CTRS |
| Harley (38) | Certified food colors | Placebo | 4 | 9 | 9 | 9.2 | 100 | CPRS | CTRS |
| Williams (39) | Certified food colors | Placebo | 4 | 29 | 29 | 6–14 | 93 | CPRS | CTRS |
| Conners (40) | Kaiser Permanente diet | Control diet | 4 | 17 | 17 | 6–13 | n.a. | CPRS | CTRS |
| Harley (41) | Feingold diet | Control diet | 3 | 36 | 36 | 6–13 | 100 | CPRS | CTRS |
| Levy (42) | Tartrazine | Placebo | 3 | 8 | 8 | 5.2 | 88 | CPRS | CPRS |
| Adams (43) | Unspecified food colors | Placebo | 3 | 18 | 18 | 4–12 | 83 | Unstandardized parent rating | Unstandardized parent rating |
| Free fatty acid supplementation | |||||||||
| Bélanger (44) | Omega-3 | Placebo | 3 | 19 | 18 | 8.3 | 69 | CPRS | CPRSC |
| Gustafsson (45) | Omega-3 | Placebo | 5 | 46 | 46 | 7–12 | 80 | CPRS | CTRSD |
| Johnson (46) | Omega-3 | Placebo | 5 | 37 | 38 | 8–18 | 85 | P-ARS | P-ARS |
| Stevens (47) | Omega-3 | Placebo | 3 | 25 | 25 | 6–13 | 87 | P-CASQ | T-CASQ |
| Voigt (48) | Omega-3 | Placebo | 5 | 27 | 26 | 6–12 | 78 | CBCL (attention) | CBCL (attention) |
| Aman (49) | Omega-6 | Placebo | 4 | 31 | 31 | 8.9 | 87 | P-RBPC (attention) | CTRS |
| Arnold (50) | Omega-6 | Placebo | 4 | 18 | 18 | 6–12 | 100 | CTRS average | CTRS average |
| Hirayama (51) | Omega-3, -6 | Placebo | 4 | 20 | 20 | 6–12 | 80 | Symptom counte | Symptom counte |
| Manor (52) | Omega-3, -6 | Placebo | 5 | 137 | 63 | 6–13 | 70 | CPRS | CTRS |
| Raz (53) | Omega-3, -6 | Placebo | 4 | 39 | 39 | 7–13 | 60 | P-ARS | CTRS |
| Sinn (54) | Omega-3, -6 | Placebo | 4 | —f | —f | 7–12 | 74 | CPRS | CPRS |
| Cognitive training | |||||||||
| Rabiner (55) | Attention training | Waiting list | 2 | 25 | 25 | n.a. | 69 | CTRS (inattention) | CTRS (inattention) |
| Shalev (56) | Attention training | Computer game | 2 | 20 | 16 | 6–13 | 83 | CPRS | CPRS |
| Steiner (57) | Attention training | Waiting list | 3 | 13 | 15 | 12.4 | 52 | CPRS | CTRS |
| Johnstone (58) | Working memory training | Easy training | 3 | 20 | 20 | 8–12 | 85 | Purpose-designed rating scale, parents | Purpose-designed rating scale, parents |
| Johnstone (59) | Working memory training | Waiting list | 2 | 22 | 20 | 7–12 | 86 | Purpose-designed rating scale, parents | None |
| Klingberg (60) | Working memory training | Easy training | 5 | 26 | 27 | 7–12 | 82 | CPRS | CTRS |
| Neurofeedback | |||||||||
| Steiner (57) | Theta-beta training | Waiting list | 3 | 13 | 15 | 12.4 | 52 | CPRS | CTRS |
| Bakhshayesh (61) | Theta-beta training | EMG biofeedback | 3 | 18 | 17 | 6–14 | 74 | P-FBB-HKS | T-FBB-HKS |
| Beauregard (62) | Theta-beta training | No treatment | 1 | 15 | 5 | 8–12 | 55 | CPRS | None |
| Holtmann (63) | Theta-beta training | Cognitive exercise | 2 | 20 | 14 | 7–12 | 91 | P-FBB-HKS | None |
| Linden (64) | Theta-beta training | Waiting list | 1 | 9 | 9 | 5–15 | n.a. | P-SNAP | None |
| Heinrich (65) | Slow cortical potential training | Waiting list | 2 | 13 | 9 | 7–13 | 95 | P-FBB-HKS | None |
| Gevensleben (66) | Theta-beta and slow cortical potential training | Cognitive exercise | 2 | 64 | 38 | 8–12 | 82 | P-FBB-HKS | T-FBB-HKS |
| Lansbergen (67) | IFBT | Placebo neurofeedback | 4 | 8 | 6 | 8–15 | 93 | P-ARS | P-ARS |
| Behavioral interventions | |||||||||
| Bor (68) | Parent training | Waiting list | 2 | 26 | 37 | 3.6 | 73 | ECBI (inattention) | None |
| Hoath (69) | Parent training | Waiting list | 1 | 9 | 11 | 5–9 | 76 | P-CAPS | T-CAPS |
| Jones (70) | Parent training | Waiting list | 3 | 50 | 29 | 3.8 | 68 | CPRS | None |
| Pisterman (71) | Parent training | Waiting list | 2 | 23 | 22 | 4.1 | 91 | Home observation | Home observation |
| Sonuga-Barke (72) | Parent training | Attention control | 4 | 30 | 28 | 2–4 | 62 | PACS | Home observation |
| Sonuga-Barke (73) | Parent training | Waiting list | 4 | 59 | 30 | 2–4 | n.a. | PACS | None |
| Thompson (74) | Parent training | Waiting list | 5 | 21 | 20 | 2–6 | 73 | PACS | Home observation |
| van den Hoofdakker (75) | Parent training | Treatment as usual | 2 | 48 | 48 | 4–12 | 76 | CPRS | None |
| Evans (76) | Parent and child training | Treatment as usual | 1 | 31 | 18 | 11–13 | 71 | P-ARS | None |
| Fehlings (77) | Parent and child training | Nondirective therapy and/or support | 2 | 13 | 13 | 8–11 | 100 | P-WWAS | None |
| Horn (78) | Parent and child training | Placebo | 2 | 16 | 16 | 7–11 | n.a. | CPRS | None |
| Webster-Stratton (79) | Parent and child training | Waiting list | 3 | 49 | 50 | 6.4 | 75 | CPRS | CTRS |
| Bloomquist (80) | Child, parent, and teacher training | Waiting list | 2 | 20 | 16 | 8.5 | 69 | CTRS | None |
| MTA (81) | Child, parent, and teacher training | Treatment as usual | 3 | 144 | 146 | 8.3 | 80 | P-SNAP | Classroom observation |
| Brown (82) | Child training | Nondirective therapy and/or support | 2 | 10 | 8 | 5–13 | 85 | CPRS (hyperactivity) | ACTRS |
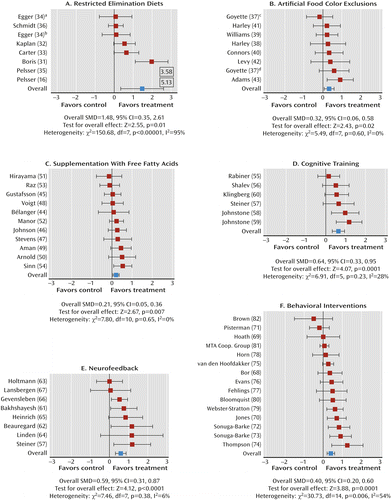
a Younger group in Egger et al. (34).
b Older group in Egger et al. (34).
c Experiment 1 in Goyette et al. (37).
d Experiment 2 in Goyette et al. (37).
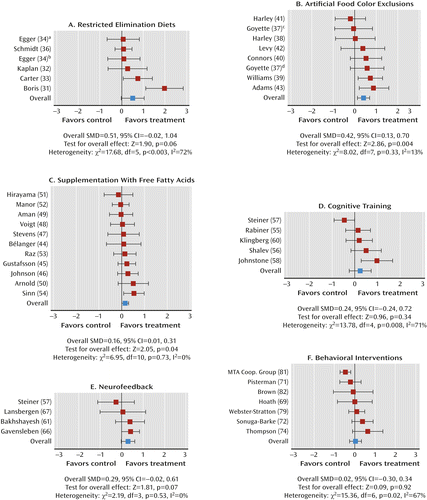
a Younger group in Egger et al. (34).
b Older group in Egger et al. (34).
c Experiment 1 in Goyette (37).
d Experiment 2 in Goyette (37).
Dietary Interventions
Restricted elimination diets.
Seven studies examining restricted elimination diets met inclusion criteria; they included studies of known antigenic foods (31, 32), elimination of specific provoking foods (33, 34), general elimination diets (16, 35), and oligoantigenic diets (36). All were rated 3 (i.e., fair) or above on the Jadad scale. Five had probably blinded assessments. One study provided separate results for older and younger groups (34). Large and statistically significant effects with most proximal assessments (Figure 2A) were reduced substantially in the analysis of probably blinded assessments, which fell just short of statistical significance (Figure 3A; drop in standardized mean difference=0.98). In both analyses, there was statistically significant between-study heterogeneity in standardized mean differences. Sensitivity analysis was not possible, as only two trials with probably blinded assessments had no/low medication.
Artificial food color exclusions.
Eight trials provided sufficient data for a meta-analysis of most proximal assessments, all of which also had probably blinded assessments. Four trials excluded certified food colors (37–39), two implemented Feingold-type diets (40, 41), one excluded tartrazine (42), and one excluded unspecified food colors (43). Six trials (75%) had Jadad ratings of 3 or more. Both approaches to analysis indicated significant positive treatment effects (Figures 2B and 3B). Restricting the probably blinded assessment analysis to the four no/low medication trials reduced the standardized mean difference (0.32) to nonsignificant levels (95% CI=–0.13, 0.77).
Free fatty acid supplementation.
Eleven free fatty acid supplementation trials met inclusion criteria. Five involved omega-3 supplements (44–48), two involved omega-6 supplements (49, 50), and the remainder used both omega-3 and omega-6 supplements (51–54). All had probably blinded assessments and scored 3 or more on the Jadad scale. Treatment effects were significant for both analyses (Figures 2C and 3C). The probably blinded assessment effects remained significant when the analysis was limited to the nine trials with no/low medication (standardized mean difference=0.17; 95% CI=0.01, 0.34).
Psychological Interventions
Cognitive training.
Six trials (three focusing on attention [55–57] and three on working memory training [58–60]) provided sufficient data for the most proximal assessment analysis; all but one had probably blinded assessments. Three were rated 3 or more on the Jadad scale. While significant treatment effects were identified using the most proximal assessments (Figure 2D), these were lost when probably blinded assessments were analyzed (Figure 3D; drop in standardized mean difference=0.40), and this effect remained unaltered when the analysis was restricted to the three no/low medication trials (standardized mean difference=0.26; 95% CI=–0.08, 0.60)].
Neurofeedback.
Of the eight trials with data for most proximal assessments, four reported probably blinded assessments and three had Jadad ratings of 3 or more. Five trials studied theta-beta training (57, 61–64), one used the training of slow cortical potentials (65), one included a combination of both of these (66), and one used individualized frequency band training (67). Significant treatment effects were seen for most proximal assessments (Figure 2E). These were substantially reduced and fell short of statistical significance for probably blinded assessments (Figure 3E; drop in standardized mean difference=0.30). Sensitivity analysis to test for medication effects was not possible because of the small number of no-medication trials.
Behavioral interventions.
Eight trials evaluated behavioral parent training (68–75), four focused on a combination of child and parent training (76–79), and two included a teacher-related component along with child- and parent-related components (80, 81). One trial used child-focused training only (82). Of the 15 trials with sufficient most proximal assessment data, seven had probably blinded assessments and six scored 3 or more on the Jadad scale. The overall standardized mean difference in the analysis of the most proximal assessments was significant (Figure 2F) but reduced to near zero for probably blinded assessments (Figure 3F; drop in standardized mean difference=0.38). Heterogeneity was significant in both analyses. Restricting the probably blinded assessments analysis to the five trials with low/no medication removed the heterogeneity (χ2=4.61; I2=13%; p=0.26) and increased the effect (standardized mean difference=0.15; 95% CI=–0.11, 0.42), which nevertheless still fell short of significance.
Effect of study quality.
Meta-regression did not support the assertion that large effect sizes were more likely in trials with low Jadad ratings, although statistical power to identify such effects was relatively low.
Discussion
Dietary interventions had small beneficial effects on ADHD symptoms. Evidence supporting psychological interventions was strongly influenced by whether the analysis was for most proximal or probably blinded assessments. Nonpharmacological standardized mean differences were substantially smaller than those reported for ADHD medications (around 0.9 for stimulants in meta-analyses of placebo-controlled randomized trials) (83). These results are less supportive of nonpharmacological interventions for ADHD than results of previous meta-analyses have been (10–14). Unlike the present analyses, however, previous analyses have rarely been limited to ADHD case subjects or focused exclusively on ADHD outcomes; nor have they addressed the issue of assessment blinding systematically by including an analysis limited to probably blinded assessments.
All three of the psychological interventions produced statistically significant reductions in symptoms according to the most proximal assessment analyses, using ratings often provided by parents who were not blind to treatment allocation. This finding mirrors those of previous meta-analyses, although the effects reported here are smaller than those reported earlier by Arns et al. for neurofeedback (13) and by Fabiano et al. (14) and Lee et al. (17) for behavioral interventions. This may be a consequence of the more stringent entry criteria used here. Most notably, the standardized mean differences for all psychological interventions dropped considerably, to nonsignificant levels, when analyses were restricted to trials with probably blinded assessments. This was most striking for behavioral interventions, where the value dropped to zero. Some of this attenuation may reflect the lower reliability—and consequently lesser sensitivity to treatment-related change—of some of the probably blinded assessments (e.g., if pre- and posttreatment ratings were supplied by different teachers). However, doubt is cast on this explanation by the fact that the size of the attenuation seen between parent-based most proximal and teacher-based probably blinded assessments differed across treatment domains. In some domains, teacher-based measures were clearly sensitive to change. This effect is therefore perhaps more likely due to the fact that estimates of effects based on most proximal assessments, most of which were based on unblinded assessments, may be inflated significantly because raters have an investment in the treatment being a success. Trials of behavioral interventions may be especially prone to this bias, as the individuals supplying these assessments (e.g., parents) are often directly involved in treatment delivery. Another possibility is that parents’ unblinded most proximal assessments accurately captured treatment effects established in the therapeutic setting but that these effects did not generalize to the settings in which probably blinded assessments were made. If so, we would expect the four behavioral intervention trials that had blind assessments made by independent trained observers within the home-based therapeutic setting to show significant treatment effects. This was not the case, although it is also possible that these assessment themselves lacked ecological validity, as they are based on only a snapshot of the child’s behavior.
A number of caveats are needed in relation to these negative behavioral intervention results. First, there was significant heterogeneity of effects in both the most proximal and probably blinded assessments analyses. The sensitivity analysis suggested that the inclusion of two trials with high levels of ADHD medication was important in this regard. The Multimodal Treatment of ADHD study (81) in particular had high medication levels in its treatment-as-usual arm (over 70% of patients were taking medication for ADHD). The inclusion of this trial may have biased the overall meta-analysis result because of its large size and its negative findings. However, excluding this trial in the no/low medication sensitivity analysis did not change the overall pattern of standardized mean differences for behavioral interventions. In order to rule out completely the possibility that medication exposure during trials biases results against behavioral interventions, future trials should be conducted using medication-naive patients—although this itself may introduce certain biases into analyses. Second, the included trials differed greatly with respect to several important treatment parameters. For instance, the largest standardized mean differences were observed with trials with preschool children—a finding consistent with the proposition that behavioral interventions may be most effective as part of early intervention strategies (84). Third, although not effective for ADHD symptoms themselves, behavioral interventions may result in other positive effects (e.g., reducing oppositional behavior [68]).
For both neurofeedback and cognitive training, effects were substantially lower for probably blinded than for most proximal assessments, despite attempts in some trials to blind parents to treatment allocation by using sham and/or active control conditions. However, the standardized mean differences for these still relatively novel approaches were higher than those for the more traditional behavioral interventions. Both sets of analyses included trials that used a range of different approaches to treatment. Cognitive training trials addressed either working memory or attention deficits, and neurofeedback trials targeted several different electrophysiological correlates of ADHD. Neither analysis had sufficient power to identify whether any approach was better than the others. Based on these results, the value of psychological approaches that directly target neuropsychological processes should be further investigated.
Artificial food color exclusion had statistically significant but modest effects on ADHD symptoms. The effects for free fatty acid supplementation were also significant but small. Restricting analyses to trials with probably blinded assessments did not change the results—probably because of the use of placebo-controlled designs, which meant that most proximal assessments were often blinded. Restricting the analyses to trials with no/low medication levels reduced the effects on ADHD of artificial food color exclusions but not of free fatty acid supplementation. The standardized mean differences for free fatty acid supplementation reported here are smaller than those reported by Bloch and Qawasmi (11), who included trials with non-ADHD populations. However, the effects were generally similar to those reported recently in a meta-analysis by Gillies et al. (85). The Gillies et al. protocols and the present study differed in important ways in inclusion criteria, the number of studies included, and the statistical model employed, especially in relation to the choice of random- versus fixed-effects models. These differences between values reported in recent reviews highlight the sensitivity of meta-analytical findings to relatively small variations in protocol and the need for caution when interpreting the clinical significance of small effects for the free fatty acid supplementation reported here. The artificial food color exclusion effects were similar in magnitude to those reported by Nigg et al. (10). The restricted elimination diets produced strong effects in the most proximal assessment analysis, which dropped markedly to marginally nonsignificant levels when the analysis was restricted to probably blinded assessments. This change was largely due to the exclusion of two trials with very large effects from the analysis of probably blinded assessments—the first (35) because it was an open-label trial and the second (16) because the reported blind assessment by a pediatrician was based in part on unmasked parental accounts of behavior. Participants in restrictive elimination diets and the artificial food color exclusion trials were often preselected to be adverse responders before entering the controlled phase of the trial, so these effects may be limited to individuals with suspected food sensitivities.
Despite using a common search and selection protocol, our ability to directly compare different nonpharmacological approaches was hindered by methodological variations across domains linked to different research traditions in each area. There were also differences between domains in terms of ratings of reported study quality. The included trials used a range of different control conditions, and these varied considerably in the extent to which they allowed for control of extraneous and potentially biasing factors, such as the effects of nonspecific attention by therapists. While the use of strict placebo control was common only in dietary domains, the best-designed psychological trials included active, attention, or sham comparators. Trials also differed considerably in the intensity and duration of therapy. An analysis of these factors was not possible because of the limited number of trials in each treatment domain. Our exclusion of trials that included individuals with subclinical levels of ADHD and the fact that few trials included analyses of the predictors of treatment response meant that we were unable to test the hypothesis that patients with less severe ADHD are more responsive to psychological interventions (86).
Conclusions
Free fatty acid supplementation and artificial food color exclusions appear to have beneficial effects on ADHD symptoms, although the effect of the former are small and those of the latter may be limited to ADHD patients with food sensitivities. Evidence for the value of behavioral interventions is limited to unblinded ratings made by individuals likely to have an investment in treatment success. While the most proximal assessment data on neurofeedback, cognitive training, and restrictive elimination diets were potentially more positive, evidence of efficacy from blinded assessments is required before they are likely to be supported as ADHD treatments. The challenge for the future is to improve the efficacy of nonpharmacological interventions on the basis of a growing understanding of ADHD pathophysiology and to better integrate these interventions with pharmacological approaches. Properly powered, randomized controlled trials with blinded, ecologically valid outcome measures are urgently needed, especially in the psychological treatment domain. Future trials should focus across a broader range of child-, parent-, and family-related functional outcomes. It is important that implementation of adequately blinded designs in future studies does not compromise the quality of the treatment being evaluated.
1 : Epidemiology of attention-deficit/hyperactivity disorder across the lifespan. Curr Opin Psychiatry 2007; 20:386–392Crossref, Medline, Google Scholar
2 : Attention-deficit hyperactivity disorder and hyperkinetic disorder. Lancet 1998; 351:429–433Crossref, Medline, Google Scholar
3 : Young adult outcome of attention deficit hyperactivity disorder: a controlled 10-year follow-up study. Psychol Med 2006; 36:167–179Crossref, Medline, Google Scholar
4 : The economic impact of attention-deficit/hyperactivity disorder in children and adolescents. J Pediatr Psychol 2007; 32:711–727Crossref, Medline, Google Scholar
5 : European clinical guidelines for hyperkinetic disorder: first upgrade. Eur Child Adolesc Psychiatry 2004; 13(suppl 1):I7–I30Crossref, Medline, Google Scholar
6 : Long-acting medications for the hyperkinetic disorders: a systematic review and European treatment guideline. Eur Child Adolesc Psychiatry 2006; 15:476–495Crossref, Medline, Google Scholar
7 : To stop or not to stop? How long should medication treatment of attention-deficit hyperactivity disorder be extended? Eur Neuropsychopharmacol 2011; 21:584–599Crossref, Medline, Google Scholar
8 : European guidelines on managing adverse effects of medication for ADHD. Eur Child Adolesc Psychiatry 2011; 20:17–37Crossref, Medline, Google Scholar
9 : Attitudes toward attention-deficit hyperactivity disorder (ADHD) treatment: parents’ and children’s perspectives. J Child Neurol 2008; 23:1036–1042Crossref, Medline, Google Scholar
10 : Meta-analysis of attention-deficit/hyperactivity disorder or attention-deficit/hyperactivity disorder symptoms, restriction diet, and synthetic food color additives. J Am Acad Child Adolesc Psychiatry 2012; 51:86–97, e8Crossref, Medline, Google Scholar
11 : Omega-3 fatty acid supplementation for the treatment of children with attention-deficit/hyperactivity disorder symptomatology: systematic review and meta-analysis. J Am Acad Child Adolesc Psychiatry 2011; 50:991–1000Crossref, Medline, Google Scholar
12 : Cognitive training for attention, inhibition, and working memory deficits: a potential treatment for ADHD? Advances in ADHD 2009; 3:89–96Google Scholar
13 : Efficacy of neurofeedback treatment in ADHD: the effects on inattention, impulsivity, and hyperactivity: a meta-analysis. Clin EEG Neurosci 2009; 40:180–189Crossref, Medline, Google Scholar
14 : A meta-analysis of behavioral treatments for attention-deficit/hyperactivity disorder. Clin Psychol Rev 2009; 29:129–140Crossref, Medline, Google Scholar
15 : Randomized Controlled Trials: Questions, Answers, and Musings, 2nd ed. London, BMJ Books/Blackwell, 2007Crossref, Google Scholar
16 : Effects of a restricted elimination diet on the behaviour of children with attention-deficit hyperactivity disorder (INCA study): a randomised controlled trial. Lancet 2011; 377:494–503Crossref, Medline, Google Scholar
17 : A meta-analysis of behavioral parent training for children with attention deficit hyperactivity disorder. Res Dev Disabil 2012; 33:2040–2049Crossref, Medline, Google Scholar
18 : Searching for unpublished trials in Cochrane reviews may not be worth the effort. J Clin Epidemiol 2009; 62:838–844, e3Crossref, Medline, Google Scholar
19 : Normative data on revised Conners Parent and Teacher Rating Scales. J Abnorm Child Psychol 1978; 6:221–236Crossref, Medline, Google Scholar
20 : Use and development of the Rutter parents’ and teachers’ scales. Int J Methods Psychiatr Res 1996; 6:63–78Crossref, Google Scholar
21 : Assessing the quality of reports of randomized clinical trials: is blinding necessary? Control Clin Trials 1996; 17:1–12Crossref, Medline, Google Scholar
22 RevMan, version 5.1. Copenhagen, Nordic Cochrane Centre, Cochrane Collaboration, 2011Google Scholar
23 : Estimating effect sizes from pretest-posttest-control group designs. Organizational Research Methods 2008; 11:364–386Crossref, Google Scholar
24 : Meta-analyses involving cross-over trials: methodological issues. Int J Epidemiol 2002; 31:140–149Crossref, Medline, Google Scholar
25 Deeks JJ, Higgins JPT, Statistical Methods Group of The Cochrane Collaboration: Statistical Algorithms in Review Manager 5, August 2010 (http://ims.cochrane.org/revman/documentation/Statistical-methods-in-RevMan-5.pdf)Google Scholar
26 Higgins JPTGreen S (eds): Cochrane Handbook for Systematic Reviews of Interventions, Version 5.1.0. Cochrane Collaboration, March 2011 (http://www.cochrane-handbook.org/)Google Scholar
27 : How to do a meta-analysis. Br J Math Stat Psychol 2010; 63:665–694Crossref, Medline, Google Scholar
28 : The power of statistical tests in meta-analysis. Psychol Methods 2001; 6:203–217Crossref, Medline, Google Scholar
29 : Interpretation of tests of heterogeneity and bias in meta-analysis. J Eval Clin Pract 2008; 14:951–957Crossref, Medline, Google Scholar
30 : Assessing publication bias in meta-analyses in the presence of between-study heterogeneity. J R Stat Soc Ser A Stat Soc 2010; 173:575–591Crossref, Google Scholar
31 : Foods and additives are common causes of the attention deficit hyperactive disorder in children. Ann Allergy 1994; 72:462–468Medline, Google Scholar
32 : Dietary replacement in preschool-aged hyperactive boys. Pediatrics 1989; 83:7–17Medline, Google Scholar
33 : Effects of a few food diet in attention deficit disorder. Arch Dis Child 1993; 69:564–568Crossref, Medline, Google Scholar
34 : Controlled trial of oligoantigenic treatment in the hyperkinetic syndrome. Lancet 1985; 1:540–545Crossref, Medline, Google Scholar
35 : A randomised controlled trial into the effects of food on ADHD. Eur Child Adolesc Psychiatry 2009; 18:12–19Crossref, Medline, Google Scholar
36 : Does oligoantigenic diet influence hyperactive/conduct-disordered children? A controlled trial. Eur Child Adolesc Psychiatry 1997; 6:88–95Medline, Google Scholar
37 : Effects of artificial colors on hyperkinetic children: a double-blind challenge study [proceedings]. Psychopharmacol Bull 1978; 14:39–40Medline, Google Scholar
38 : Synthetic food colors and hyperactivity in children: a double-blind challenge experiment. Pediatrics 1978; 62:975–983Medline, Google Scholar
39 : Relative effects of drugs and diet on hyperactive behaviors: an experimental study. Pediatrics 1978; 61:811–817Crossref, Medline, Google Scholar
40 : Food additives and hyperkinesis: a controlled double-blind experiment. Pediatrics 1976; 58:154–166Medline, Google Scholar
41 : Hyperkinesis and food additives: testing the Feingold hypothesis. Pediatrics 1978; 61:818–828Medline, Google Scholar
42 : Hyperkinesis and diet: a replication study. Am J Psychiatry 1978; 135:1559–1560Link, Google Scholar
43 : Lack of behavioral effects from Feingold diet violations. Percept Mot Skills 1981; 52:307–313Crossref, Medline, Google Scholar
44 : Omega-3 fatty acid treatment of children with attention-deficit hyperactivity disorder: a randomized, double-blind, placebo-controlled study. Paediatr Child Health (Oxford) 2009; 14:89–98Crossref, Google Scholar
45 : EPA supplementation improves teacher-rated behaviour and oppositional symptoms in children with ADHD. Acta Paediatr 2010; 99:1540–1549Crossref, Medline, Google Scholar
46 : Omega-3/omega-6 fatty acids for attention deficit hyperactivity disorder: a randomized placebo-controlled trial in children and adolescents. J Atten Disord 2009; 12:394–401Crossref, Medline, Google Scholar
47 : EFA supplementation in children with inattention, hyperactivity, and other disruptive behaviors. Lipids 2003; 38:1007–1021Crossref, Medline, Google Scholar
48 : A randomized, double-blind, placebo-controlled trial of docosahexaenoic acid supplementation in children with attention-deficit/hyperactivity disorder. J Pediatr 2001; 139:189–196Crossref, Medline, Google Scholar
49 : The effects of essential fatty acid supplementation by Efamol in hyperactive children. J Abnorm Child Psychol 1987; 15:75–90Crossref, Medline, Google Scholar
50 : Gamma-linolenic acid for attention-deficit hyperactivity disorder: placebo-controlled comparison to D-amphetamine. Biol Psychiatry 1989; 25:222–228Crossref, Medline, Google Scholar
51 : Effect of docosahexaenoic acid-containing food administration on symptoms of attention-deficit/hyperactivity disorder: a placebo-controlled double-blind study. Eur J Clin Nutr 2004; 58:467–473Crossref, Medline, Google Scholar
52 : The effect of phosphatidylserine containing omega3 fatty-acids on attention-deficit hyperactivity disorder symptoms in children: a double-blind placebo-controlled trial, followed by an open-label extension. Eur Psychiatry 2012; 27:335–342Crossref, Medline, Google Scholar
53 : The influence of short-chain essential fatty acids on children with attention-deficit/hyperactivity disorder: a double-blind placebo-controlled study. J Child Adolesc Psychopharmacol 2009; 19:167–177Crossref, Medline, Google Scholar
54 : Effect of supplementation with polyunsaturated fatty acids and micronutrients on learning and behavior problems associated with child ADHD. J Dev Behav Pediatr 2007; 28:82–91Crossref, Medline, Google Scholar
55 : A randomized trial of two promising computer-based interventions for students with attention difficulties. J Abnorm Child Psychol 2010; 38:131–142Crossref, Medline, Google Scholar
56 : Computerized progressive attentional training (CPAT) program: effective direct intervention for children with ADHD. Child Neuropsychol 2007; 13:382–388Crossref, Medline, Google Scholar
57 : Computer-based attention training in the schools for children with attention deficit/hyperactivity disorder: a preliminary trial. Clin Pediatr (Phila) 2011; 50:615–622Crossref, Medline, Google Scholar
58 : A pilot study of combined working memory and inhibition training for children with AD/HD. Atten Defic Hyperact Disord 2010; 2:31–42Crossref, Medline, Google Scholar
59 : Neurocognitive training for children with and without AD/HD. Atten Defic Hyperact Disord 2012; 4:11–23Crossref, Medline, Google Scholar
60 : Computerized training of working memory in children with ADHD: a randomized, controlled trial. J Am Acad Child Adolesc Psychiatry 2005; 44:177–186Crossref, Medline, Google Scholar
61 : Neurofeedback in ADHD: a single-blind randomized controlled trial. Eur Child Adolesc Psychiatry 2011; 20:481–491Crossref, Medline, Google Scholar
62 : Functional magnetic resonance imaging investigation of the effects of neurofeedback training on the neural bases of selective attention and response inhibition in children with attention-deficit/hyperactivity disorder. Appl Psychophysiol Biofeedback 2006; 31:3–20Crossref, Medline, Google Scholar
63 : Spezifische Wirksamkeit von Neurofeedback auf die Impulsivität bei ADHS (Specific effects of neurofeedback on impulsivity in ADHD). Kindheit und Entwicklung 2009; 18:95–104Crossref, Google Scholar
64 : A controlled study of the effects of EEG biofeedback on cognition and behavior of children with attention deficit disorder and learning disabilities. Biofeedback Self Regul 1996; 21:35–49Crossref, Medline, Google Scholar
65 : Training of slow cortical potentials in attention-deficit/hyperactivity disorder: evidence for positive behavioral and neurophysiological effects. Biol Psychiatry 2004; 55:772–775Crossref, Medline, Google Scholar
66 : Is neurofeedback an efficacious treatment for ADHD? A randomised controlled clinical trial. J Child Psychol Psychiatry 2009; 50:780–789Crossref, Medline, Google Scholar
67 : ADHD and EEG-neurofeedback: a double-blind randomized placebo-controlled feasibility study. J Neural Transm 2011; 118:275–284Crossref, Medline, Google Scholar
68 : The effects of the Triple P-Positive Parenting Program on preschool children with co-occurring disruptive behavior and attentional/hyperactive difficulties. J Abnorm Child Psychol 2002; 30:571–587Crossref, Medline, Google Scholar
69 : A feasibility study of enhanced group Triple P: Positive Parenting Programme for parents of children with attention deficit/hyperactivity disorder. Behav Change 2002; 4:191–206Crossref, Google Scholar
70 : Efficacy of the Incredible Years Programme as an early intervention for children with conduct problems and ADHD: long-term follow-up. Child Care Health Dev 2008; 34:380–390Crossref, Medline, Google Scholar
71 : The role of parent training in treatment of preschoolers with ADDH. Am J Orthopsychiatry 1992; 62:397–408Crossref, Medline, Google Scholar
72 : Parent-based therapies for preschool attention-deficit/hyperactivity disorder: a randomized, controlled trial with a community sample. J Am Acad Child Adolesc Psychiatry 2001; 40:402–408Crossref, Medline, Google Scholar
73 : Parent training for attention deficit/hyperactivity disorder: is it as effective when delivered as routine rather than as specialist care? Br J Clin Psychol 2004; 43:449–457Crossref, Medline, Google Scholar
74 : A small-scale randomized controlled trial of the revised New Forest Parenting Programme for preschoolers with attention deficit hyperactivity disorder. Eur Child Adolesc Psychiatry 2009; 18:605–616Crossref, Medline, Google Scholar
75 : Effectiveness of behavioral parent training for children with ADHD in routine clinical practice: a randomized controlled study. J Am Acad Child Adolesc Psychiatry 2007; 46:1263–1271Crossref, Medline, Google Scholar
76 : Effectiveness of the Challenging Horizons After-School Program for young adolescents with ADHD. Behav Ther 2011; 42:462–474Crossref, Medline, Google Scholar
77 : Attention deficit hyperactivity disorder: does cognitive behavioral therapy improve home behavior? J Dev Behav Pediatr 1991; 12:222–228Crossref, Google Scholar
78 : Additive effects of psychostimulants, parent training, and self-control therapy with ADHD children. J Am Acad Child Adolesc Psychiatry 1991; 30:233–240Crossref, Medline, Google Scholar
79 : Combining parent and child training for young children with ADHD. J Clin Child Adolesc Psychol 2011; 40:191–203Crossref, Medline, Google Scholar
80 : Effects of a school-based cognitive-behavioral intervention for ADHD children. J Abnorm Child Psychol 1991; 19:591–605Crossref, Medline, Google Scholar
81 : A 14-month randomized clinical trial of treatment strategies for attention-deficit/hyperactivity disorder. Arch Gen Psychiatry 1999; 56:1073–1086Crossref, Medline, Google Scholar
82 : Methylphenidate and cognitive therapy in children with attention deficit disorder: a double-blind trial. J Dev Behav Pediatr 1986; 7:163–174Crossref, Medline, Google Scholar
83 : Comparing the efficacy of medications for ADHD using meta-analysis. MedGenMed 2006; 8:4Medline, Google Scholar
84 : Developmental phenotypes and causal pathways in attention deficit/hyperactivity disorder: potential targets for early intervention? J Child Psychol Psychiatry 2010; 51:368–389Crossref, Medline, Google Scholar
85 : Polyunsaturated fatty acids (PUFA) for attention deficit hyperactivity disorder (ADHD) in children and adolescents. Cochrane Database Syst Rev 2012; 7:CD007986Medline, Google Scholar
86 : Refining the diagnoses of inattention and overactivity syndromes: a reanalysis of the Multimodal Treatment study of attention deficit hyperactivity disorder (ADHD) based on ICD-10 criteria for hyperkinetic disorder. Clin Neurosci Res 2005; 5:307–314.Crossref, Google Scholar



