Alcohol Use Disorder and Risk of Suicide in a Swedish Population-Based Cohort
Abstract
Objective:
The authors examined the association between alcohol use disorder (AUD) and risk of suicide, before and after accounting for psychiatric comorbidity, and assessed the extent to which the observed association is due to a potentially causal mechanism or genetic and familial environmental confounding factors that increase risk for both.
Methods:
Longitudinal population-wide Swedish medical, criminal, and pharmacy registries were used to evaluate the risk of death by suicide as a function of AUD history. Analyses employed prospective cohort and co-relative designs, including data on 2,229,880 native Swedes born between 1950 and 1970 and observed from age 15 until 2012.
Results:
The lifetime rate of suicide during the observation period was 3.54% for women and 3.94% for men with AUD, compared with 0.29% and 0.76% of women and men, respectively, without AUD. In adjusted analyses, AUD remained robustly associated with suicide: hazard ratios across observation periods ranged from 2.61 to 128.0 among women and from 2.44 to 28.0 among men. Co-relative analyses indicated that familial confounding accounted for some, but not all, of the observed association. A substantial and potentially causal relationship remained after accounting for a history of other psychiatric diagnoses.
Conclusions:
AUD is a potent risk factor for suicide, with a substantial association persisting after accounting for confounding factors. These findings underscore the impact of AUD on suicide risk, even in the context of other mental illness, and implicate the time frame shortly after a medical or criminal AUD registration as critical for efforts to reduce alcohol-related suicide.
Suicide is a major public health concern, accounting for over 47,000 deaths in the United States in 2017 (1), and representing the 18th leading cause of death worldwide in 2016 (2). Risk is multifactorial, attributable to genetic liability (3–7), environmental stressors (8–12), and comorbid conditions, including alcohol use disorder (AUD) (13–16). AUD itself is relatively common, is associated with an array of other psychiatric outcomes (17), and carries a substantial economic burden (18). It is also associated with increased mortality (19–22): alcohol consumption accounted for over 5% of deaths worldwide in 2016 (23).
Given the co-occurrence of AUD with other psychiatric disorders (17), in conjunction with the risk of suicide conferred by affective and psychotic disorders (16), the nature of the association between AUD and suicide has been difficult to establish. The observed associations may be due to a direct causal effect and/or to confounding factors that affect risk for both AUD and suicide. If psychiatric comorbidity is not accounted for, the direct risks attributed to AUD may be inflated. Efforts to address this are complicated by the relative rarity of suicide in the population, necessitating large sample sizes to reliably estimate the relationship between AUD and suicide in population-based samples.
Both AUD (24) and suicide (6, 25) exhibit familial aggregation, in part as a result of genetic mechanisms. By using the co-twin control design (26), causal inference is improved by accounting for familial factors—genetic and environmental in nature—that may act as confounders; residual associations are more likely to be causal in nature, although in observational studies a causal mechanism cannot be known for certain. Findings from such approaches could be informative for risk assessment, and the identification of a potentially causal relationship may signal a target for intervention.
In this study, we used data from Swedish population registries to address two primary research questions. First, we tested whether AUD and death by suicide are associated, before and after accounting for psychiatric comorbidity. Second, we assessed whether the observed association is attributable to confounding familial factors, potentially causal processes, or a combination of mechanisms, through the use of co-relative control models.
Methods
Sample
All native Swedish citizens born between 1950 and 1970 who had not died or emigrated by age 15 were included in our analyses. Observations began at age 15 and ended at death, emigration from Sweden, or in 2012, the last year for which registry data were available. Individuals who died by suicide or had an AUD registration before age 15 were excluded. Those with other psychiatric diagnoses prior to age 15 were retained in the model; for the purposes of time-dependent covariates, these were coded as occurring at age 15. The study was approved by the Regional Ethical Review Board of Lund University, and subject consent was waived.
Swedish population registers with national coverage were used to determine cause of death, diagnostic status for psychiatric predictors and covariates or confounders, and sociodemographic covariates. The availability and content of these registers has been described previously (22, 27). Registers are available for inpatient and outpatient records, including both primary and secondary diagnoses; criminal and suspicion records; prescription records; linking of family members through the Multi-Generation Register; and demographic and socioeconomic data through the Swedish national census and population registers. Records are linked using unique personal identification numbers, which are replaced by anonymous serial numbers to maintain confidentiality.
Outcome and Predictor Variables
The outcome was death by suicide. The predictor of primary interest was AUD. In full models, other psychiatric diagnoses were included as potential confounders. The ICD codes (from ICD-8, ICD-9, and ICD-10) used to determine cause of death, diagnostic status for AUD, and status for other psychiatric covariates are listed in the online supplement and are consistent with previous studies (28, 29). Deaths of undetermined intent were included as suicides to avoid underestimating prevalence (N=3,933, or 25.3% of all suicides), consistent with other studies of the Swedish population (28, 30). A sensitivity analysis was conducted with deaths of undetermined intent excluded, to evaluate the association between AUD and death by suicide among known deaths by suicide (see the online supplement).
Statistical Analysis
Primary analyses.
We used Cox proportional hazards models to test the association between AUD and suicide. AUD was included as a time-varying covariate; from age 15 until the first AUD-related registration, an individual was considered not to have AUD. Beyond the first AUD registration, the individual was considered to have AUD. In full models, psychiatric comorbidity variables were included as time-varying covariates. Analyses were conducted separately by sex. Mean parental education and birth year were included as covariates. Parental education was coded as follows: 1=9 or fewer years of education; 2=10–11 years; 3=12 or more years. Hazard ratios and 95% confidence intervals are reported for all variables. All analyses were conducted in SAS, version 9.4 (SAS Institute, Cary, N.C.), primarily using proc phreg.
Proportionality assumption.
We tested the proportionality assumption of our Cox models by creating dummy-coded variables for increments of observation time and estimating the hazard ratios for those variables. After comparing the Akaike information criterion for models testing 5-year, 10-year, and irregular increments (<1 year, 1–5 years, 5–10 years), we selected the 5-year increment model, in which distinct hazard ratios were estimated for individuals observed for <5 years, 5–10 years, 10–15 years, and so on.
Co-relative analyses.
We identified pairs of same-sex cousins, half siblings, and full siblings born within 10 years of one another for inclusion in co-relative analyses, which control for shared familial factors that may confound the association between AUD and suicide by testing for effects within family strata. If familial factors affect this association, the effect size of AUD is expected to decrease in relatives of increasing genetic resemblance, as confounding factors are increasingly accounted for within pairs. If the association is purely causal, the effect size is not expected to substantively change across analyses of the unselected population and relative pairs of varying genetic relatedness. Pairs of relatives who are discordant in exposure to the putative risk factor (here, AUD) at some point in time are informative. To increase power, mean parental education was not included as a covariate in these analyses because of missing data; furthermore, we combined sexes for co-relative analyses, resulting in the following numbers of informative pairs: cousins, 7,559; half siblings, 1,741; full siblings, 5,054. Unadjusted models were run initially, followed by models accounting for psychiatric comorbidity. A supplementary co-relative analysis was conducted that extrapolated results to discordant monozygotic twin pairs, which we otherwise lacked sufficient statistical power to test (see the online supplement).
Results
The selected birth cohort consisted of 2,229,880 individuals. Table 1 presents the frequency of suicide, AUD, and other covariates. Among women, the suicide rate for those without AUD was 0.29% (N=3,062), and among those with AUD, it was 3.54% (N=1,158). The corresponding rates among men were 0.76% (N=8,079) and 3.94% (N=3,229), respectively. The mean age at AUD registration was 39.99 years (SD=11.70) for women and 39.38 years (SD=11.47) for men. Mean age at suicide death was 36.22 years (SD=11.35) for women and 35.83 years (SD=11.01) for men. Correlations (r) among non-AUD psychiatric diagnoses ranged from 0.42 to 0.87 (see Table S1 in the online supplement), with the strongest estimates between psychotic disorders and AUD or drug abuse.
| Death by Suicide | ||||
|---|---|---|---|---|
| Yes | No | |||
| Group | N | % | N | % |
| Individuals in cohort | ||||
| Women | 4,220 | 0.39 | 1,080,026 | 99.61 |
| Men | 11,308 | 0.99 | 1,134,326 | 99.01 |
| AUDa | ||||
| Women | 1,158 | 27.44 | 31,546 | 2.92 |
| Men | 3,229 | 28.56 | 78,644 | 6.93 |
| Drug use disorder | ||||
| Women | 829 | 19.64 | 20,472 | 1.90 |
| Men | 2,042 | 18.06 | 36,857 | 3.25 |
| Affective disorder | ||||
| Women | 1,144 | 27.11 | 67,879 | 6.28 |
| Men | 1,669 | 14.76 | 49,439 | 4.36 |
| Psychotic disorder | ||||
| Women | 1,362 | 32.27 | 46,464 | 4.30 |
| Men | 2,953 | 26.11 | 74,511 | 6.57 |
| Personality disorder | ||||
| Women | 661 | 15.66 | 15,693 | 1.45 |
| Men | 1,006 | 8.90 | 15,647 | 1.38 |
| Phobia or anxiety disorder | ||||
| Women | 533 | 12.63 | 48,098 | 4.45 |
| Men | 696 | 6.15 | 34,610 | 3.05 |
| Other psychiatric disorder | ||||
| Women | 529 | 12.54 | 50,266 | 4.65 |
| Men | 598 | 5.29 | 30,054 | 2.65 |
TABLE 1. Frequency of key predictors stratified by gender and suicide outcome in a study of alcohol use disorder (AUD) and suicide risk in a Swedish population-based cohort
Population-Based Analyses
In preliminary Cox regressions in which AUD was the sole predictor and was time-varying, AUD and suicide were strongly associated in both women (hazard ratio=37.53, 95% CI=34.82, 40.45) and men (hazard ratio=16.33, 95% CI=15.60, 17.08). Adjusting for sociodemographic covariates did not substantially alter the effect of AUD (women: hazard ratio=37.10, 95% CI=34.26, 40.18; men: hazard ratio=16.18, 95% CI=15.42, 16.96).
We tested the proportionality assumption by estimating the hazard ratio for AUD, adjusted only for sociodemographic covariates, across individuals for whom the length of observation time differed in 5-year increments. The impact of AUD onset for risk of suicide declined rapidly over time (see Table S2 in the online supplement). We therefore constructed a full model, adjusted for both sociodemographic and time-varying psychiatric covariates, allowing for different hazard ratios across observation periods.
In these full models, AUD was the strongest predictor of suicide death in the first 5 years of observation for both sexes (Table 2). Hazard ratios declined precipitously between the first and second 5-year increments, declining more gradually thereafter (Figure 1). The risk associated with AUD remained comparable to, and sometimes exceeded (although with overlapping confidence intervals), risks associated with psychotic and affective disorders. After 25 years of observation, AUD remained significantly associated with suicide for both women (hazard ratio=2.62, 95% CI=2.16, 3.14) and men (hazard ratio=2.44, 95% CI=2.15, 2.79).
| Months of Observation | ||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| 0–59 | 60–119 | 120–179 | 180–239 | 240–299 | ≥300 | |||||||
| Covariate | Hazard Ratio | 95% CI | Hazard Ratio | 95% CI | Hazard Ratio | 95% CI | Hazard Ratio | 95% CI | Hazard Ratio | 95% CI | Hazard Ratio | 95% CI |
| Women | ||||||||||||
| AUD | 128.0 | 76.1, 215.1 | 16.4 | 9.90, 27.2 | 15.5 | 10.2, 23.7 | 7.36 | 4.99, 10.8 | 8.68 | 5.90, 12.77 | 2.61 | 2.16, 3.14 |
| Other psychiatric disorders | —b | — | 2.06 | 0.68, 6.22 | 2.79 | 1.50, 5.22 | 1.30 | 0.73, 2.31 | 1.35 | 0.88, 2.05 | 1.54 | 1.28, 1.85 |
| Phobia and anxiety disorders | —b | — | —b | — | 1.44 | 0.73, 2.87 | 0.82 | 0.44, 1.52 | 1.17 | 0.77, 1.78 | 1.46 | 1.21, 1.77 |
| Personality disorders | 0.48 | 0.11, 2.15 | 1.59 | 0.87, 2.90 | 1.37 | 0.89, 2.12 | 1.80 | 1.25, 2.60 | 1.66 | 1.19, 2.30 | 1.44 | 1.23, 1.70 |
| Psychotic disorders | 12.35 | 4.00, 38.1 | 18.3 | 10.5, 32.1 | 10.5 | 6.55, 16.8 | 7.22 | 4.46, 11.7 | 3.96 | 2.49, 6.28 | 4.43 | 3.50, 5.62 |
| Affective disorders | 5.40 | 1.08, 27.0 | 6.09 | 3.44, 10.8 | 4.70 | 3.05, 7.26 | 7.73 | 4.99, 12.0 | 5.69 | 3.80, 8.50 | 4.63 | 3.80, 5.64 |
| Drug abuse | 3.06 | 1.07, 8.75 | 3.26 | 1.86, 5.72 | 2.58 | 1.67, 3.99 | 2.06 | 1.38, 3.10 | 1.73 | 1.21, 2.48 | 2.83 | 2.37, 3.38 |
| Men | ||||||||||||
| AUD | 28.0 | 17.7, 44.3 | 9.21 | 7.15, 11.87 | 8.17 | 6.63, 10.1 | 6.59 | 5.34, 8.14 | 5.84 | 4.70, 7.26 | 2.44 | 2.15, 2.79 |
| Other psychiatric disorders | —b | — | 0.31 | 0.02, 3.07 | 0.35 | 0.11, 1.08 | 0.72 | 0.40, 1.32 | 1.13 | 0.79, 1.63 | 1.54 | 1.32, 1.78 |
| Phobia and anxiety disorders | —b | — | 0.98 | 0.19, 4.95 | 1.88 | 1.01, 3.51 | 1.34 | 0.82, 2.19 | 1.11 | 0.79, 1.56 | 1.10 | 0.95, 1.28 |
| Personality disorders | 0.69 | 0.20, 2.36 | 1.56 | 1.10, 2.21 | 1.28 | 1.00, 1.65 | 1.26 | 1.01, 1.57 | 1.15 | 0.94, 1.42 | 1.21 | 1.07, 1.36 |
| Psychotic disorders | 16.34 | 8.24, 32.38 | 11.18 | 8.28, 15.07 | 6.89 | 5.36, 8.86 | 4.05 | 3.20, 5.13 | 3.05 | 2.39, 3.88 | 3.57 | 3.10, 4.11 |
| Affective disorders | 3.68 | 0.89, 15.29 | 3.00 | 1.93, 4.66 | 3.98 | 3.02, 5.25 | 3.94 | 3.12, 4.97 | 3.71 | 3.00, 4.60 | 4.06 | 3.62, 4.56 |
| Drug abuse | 3.13 | 1.38, 7.13 | 3.67 | 2.66, 5.07 | 2.93 | 2.30, 3.73 | 3.39 | 2.71, 4.23 | 3.00 | 2.45, 3.67 | 2.07 | 1.86, 2.31 |
TABLE 2. Adjusted hazard ratios for alcohol use disorder (AUD) and covariates predicting suicide death in a Swedish population-based cohorta
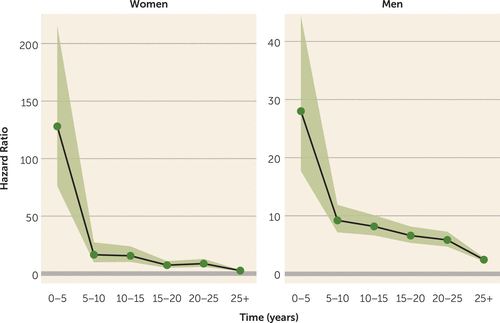
FIGURE 1. Hazard ratios as a function of time beyond alcohol use disorder (AUD) registration in a study of AUD and suicide risk in a Swedish population-based cohorta
a The graphs show hazard ratios (shaded areas indicate 95% confidence intervals) from adjusted models estimating the association between AUD and suicide as a function of time elapsed since AUD registration.
Because of concerns about data sparseness, and because of the relatively modest changes in risk associated with AUD beyond the first 5 years after a registration, secondary analyses estimated hazard ratios averaged across observation time. We tested the association between AUD and suicide among individuals without a registration for other psychiatric diagnoses (944,378 women, 7,701 with AUD; 1,002,880 men, 23,823 with AUD), including sociodemographic covariates, and AUD as a time-varying predictor. The associations were strong, with hazard ratios of 73.74 (95% CI=63.68, 85.37) for women and 20.69 (95% CI=19.07, 22.46) for men.
We then tested whether age at onset of AUD was associated with suicide risk. In a Cox proportional hazards model accounting for birth year, parental education, and time-dependent psychiatric comorbidity, we estimated the effect of age at AUD onset, binning into 10-year increments beginning with <25 years of age. We observed steady decreases in risk, relative to an age at onset <25, for ages 25–35 and in each subsequent age bin (see Table S3 in the online supplement).
Co-Relative Analyses
We next ran parallel models within data sets consisting of same-sex relative pairs of varying levels of genetic resemblance—cousins, half siblings, and full siblings. The results are depicted in Figure 2 and Table 3. In unadjusted models, as the degree of genetic relatedness increased, the magnitude of the AUD-suicide association decreased, although half siblings deviated from this trend, suggesting that familial confounding contributes to the observed association between AUD and death by suicide. In models adjusted for time-dependent psychiatric comorbidity, a markedly different pattern was observed. The estimates were consistent across groups of varying relatedness, suggesting little or no additional familial confounding of the association between AUD and suicide. Half siblings were again outliers, although estimates are known imprecisely; confidence intervals overlapped with all estimates except that from the population-based adjusted model. In a supplemental model in which the hazard ratio for monozygotic twins could be extrapolated, the hazard ratio declined further but remained significantly greater than 1 (hazard ratio=3.69, 95% CI=2.77, 4.90; see the supplemental text and Table S4 in the online supplement).
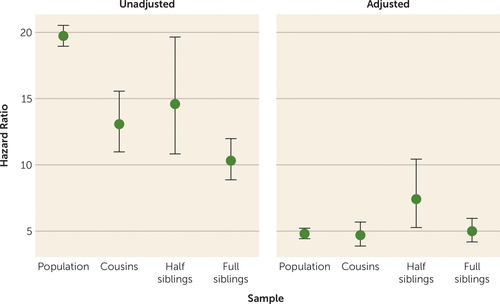
FIGURE 2. Hazard ratios for alcohol use disorder (AUD) in the population and in discordant family pairs in a study of AUD and suicide risk in a Swedish population-based cohorta
a The graphs show hazard ratios (error bars indicate 95% confidence intervals), averaged across observation time, for co-relative pairs discordant for exposure to, or timing of, AUD. The hazard ratio for the overall population is provided for comparison, with sex included as a covariate. Sexes were combined to improve statistical power. Sample sizes are as follows: population, N=2,229,880; cousins, N=1,469,388; half siblings, N=203,594; full siblings, N=896,087. Numbers of informative pairs, by co-relative type, are as follows: cousins, N=5,524; half siblings, N=1,241; full siblings, N=3,741 (see Table 3).
| Unadjusted | Adjustedb | ||||
|---|---|---|---|---|---|
| Sample | Number of Informative Pairs | Hazard Ratio | 95% CI | Hazard Ratio | 95% CI |
| Populationc | 19.73 | 18.95, 20.53 | 4.80 | 4.42, 5.21 | |
| Cousins | 5,524 | 13.07 | 10.98, 15.56 | 4.69 | 3.87, 5.68 |
| Half siblings | 1,241 | 14.59 | 10.82, 19.65 | 7.41 | 5.27, 10.43 |
| Full siblings | 3,741 | 10.31 | 8.87, 11.98 | 4.99 | 4.18, 5.96 |
TABLE 3. Hazard ratios of alcohol use disorder on suicide death across co-relative pairs of varying genetic resemblance in a Swedish population-based cohorta
Discussion
For Swedish individuals born between 1950 and 1970, AUD was associated with a substantially increased risk of death by suicide. In models accounting for psychiatric comorbidity and shifts in risk across observation time, hazard ratios for AUD were 128 for women and 28 for men in the first 5 years after a registration. While risks associated with AUD were substantially attenuated beyond that time frame, they remained elevated (hazard ratio>2 for both sexes) even 25 or more years later. These findings are comparable to those of previous studies of AUD and suicide in Denmark and the United States (16, 31) and with a recent meta-analysis that included samples of diverse national origins (32). They are similarly in line with Swedish studies examining the increased suicide risk associated with eating disorders (33) and obsessive-compulsive disorder (28). We observed a markedly higher initial risk among women, although this difference was reduced in adjusted models. Critically, co-relative analyses indicated a complex etiology underlying the AUD-suicide association: Familial factors that increase risk for both AUD and death by suicide, in conjunction with a pronounced and potentially causal pathway, likely contribute to the observed association.
This is, to our knowledge, the largest population-based study examining the association between alcohol use disorder and death by suicide, accounting for psychiatric comorbidity, and further clarifying the potential familial confounding of the observed association. Previous studies in Scandinavian countries have explored complementary research questions, reporting evidence of familial aggregation of AUD and suicide (34) and comparable magnitudes and patterns of association (31, 35). In the context of the extant research, the present findings provide insight into the potential consequences of AUD on a broad scale.
The effect of AUD was substantially higher among women in unadjusted models, although this discrepancy was attenuated in adjusted models, suggesting that psychiatric comorbidity differentially affects AUD-based risk across the sexes. This may reflect the higher threshold for AUD among women and the higher prevalence of internalizing disorders. Women die by suicide at lower rates than men overall (36); however, data regarding the relationships among AUD, suicide, and sex are relatively scarce, and many studies have been insufficiently powered to directly examine the AUD-suicide association in women given their lower prevalence of both outcomes. This likely contributes to inconsistent findings. Some studies have reported that women have higher alcohol-related risks of suicidal behavior (14, 15), while others have not detected moderation by sex (37). Our findings indicate that psychiatric comorbidity attenuates the AUD-suicide association, particularly among women. Inclusion of these factors in analytic and theoretical models is thus critical in order to accurately estimate risks specific to AUD.
In this study, hazard ratios were even more pronounced among individuals with AUD who did not have registrations for other psychiatric conditions. In those without a registration for other psychopathology, a group that constituted the majority (87.3%) of the full sample but only 27.5% of those with AUD, the very large increase in suicide risk associated with AUD makes these individuals an obvious focus for interventions in what might mistakenly be considered a low-risk group.
The co-relative models demonstrate two key findings. First, familial confounders account for a substantial proportion of the association between AUD and suicide. As increasing degrees of familial factors are accounted for across co-relative pairs, the association between AUD and suicide declines in the unadjusted models. This suggests that AUD is indexing a variety of dispositional features that influence risk of both AUD and suicide. Second, even after adjusting for psychiatric comorbidity, a likely source of the familial confounding described above, there remains a substantial risk of suicide following an AUD registration. The relative stability in hazard ratio estimates across relative pairs (Figure 2, adjusted panel) indicates that this residual association is consistent with a causal mechanism (26). Thus, the pronounced associations observed in the preliminary model unadjusted for psychiatric comorbidity and averaged across observation time, where we observed 16- to 37-fold increased risk, may in part be due to an array of correlated factors indexed by AUD (e.g., propensity toward impulsiveness, genetic loading for mental illness, etc.) and to a causal effect of AUD. The latter may take the form of stressful circumstances or events attributable to the disorder (9, 10, 38), substance-induced depression (39, 40), social isolation (41), acute intoxication (14), or other factors, many of which we are unable to address using registry-based data. Overall, our findings are consistent with previous evidence of familial confounding in related outcomes, such as drug abuse and mortality (42) and AUD and mortality (22).
We note an elevated suicide risk among half siblings discordant for AUD (or timing of death by suicide), which deviates from the otherwise consistent hazard ratios across co-relative pairs. Relative to full sibling and cousin pairs, members of these pairs have more often been exposed to parental marital disruption, and rates of externalizing psychopathology are substantially higher in their parents (43, 44). The rate of suicide is higher among half siblings in this sample (1.2% for men, 0.52% for women). There are likely to be confounders relevant to risk among half siblings that are not relevant, or are less relevant, to other co-relative pairs. Although identifying those factors would be speculative using only registry data, previous evidence suggests that children of divorced parents are at increased risk for depression recurrence (45), smoking (46), suicidal behavior (47), and alcohol misuse (48), as well as measures of social functioning such as lower educational achievement (49) and adult socioeconomic status (50).
The violation of the proportionality assumption highlights the dynamic nature of suicide risk and indicates that it decreases as time elapses from the first AUD registration. In addition, this finding supports the assertion that AUD causally affects risk: If the observed AUD-suicide association were merely attributable to stable confounding factors (e.g., personality, genetic liability to psychiatric disorders), we would not expect to observe such a marked dissipation of risk over time. While the goal of testing this model was to provide context for our primary findings, these results raise the possibility that the time frame shortly after AUD registration may represent a critical period during which risk of suicide is most pronounced. A previous study of suicide risk in the wake of a nonfatal self-harm incident provides further support for this possibility (51). Another possibility is that the observed association of declining risk over time is due in part to individuals whose AUD remits after their initial registration, among whom risk of suicide may then diminish.
In addition, we observed that earlier onset of AUD—which is posited to be an indicator of severity, propensity toward externalizing behavior (52, 53), and genetic liability (54–56)—is associated with increased suicide risk. The implications of these findings are twofold. First, prevention and intervention efforts may be most effective when directed toward individuals facing a relatively recent AUD-related incident. Second, these efforts may be especially fruitful for those with early onset of AUD. Further studies aimed at dissecting the time-sensitive nature of risk are essential.
Our findings must be considered in the context of our use of registry data. AUD registration corresponds to a high threshold for AUD, as it requires that an individual come to the attention of the medical or criminal justice system. Some individuals who meet diagnostic criteria will escape detection. Therefore, conservatively, the present findings should be considered most relevant to severe AUD. The mean age at first AUD registration is somewhat older than mean onset ages reported in studies that do not rely on registry data and is in part a function of cohort selection: As earlier cohorts are observed later into life, they present more opportunities for late-stage AUD-related registrations (e.g., those derived from alcohol-related medical conditions) to be identified. Our previous study of Swedish adoptees, which included those born as late as 1993, found a mean onset age of 33.9 years for AUD (38.2 years among women, 32.3 years among men) (27). Given that the mean age at death by suicide precedes the mean age at first AUD registration in the present cohort, it is possible that some suicide decedents suffered from as-yet-unrecognized AUD. Such a misclassification error could lead to an underestimation of the risks associated with AUD. Despite these drawbacks, the registry-based approach we used here is objective and not subject to self-report bias; furthermore, a high degree of correspondence among AUD registration sources (odds ratios, 9.6–74.8 [27]) indicates that the measure is valid.
There are several notable limitations to this study. First, the start date of data availability differs across registries. We made every effort to select a cohort to maximize coverage; however, data will be consistently available across all registries for younger cohorts, and as these cohorts age into risk periods for AUD and suicide, our ability to further elucidate the mechanisms underlying observed associations will improve. Our use of registries also reduces our ability to identify less severe cases of AUD; relatedly, we may miss episodes of relapse that are not recorded in registers but that contribute to suicide risk years after the initial AUD diagnosis as individuals proceed through remissions and relapses. Second, exclusion of deaths of undetermined intent reduced the adjusted effect of AUD (see Table S5 in the online supplement); this may be due to difficulties determining whether alcohol-related deaths were intentional, particularly given the relationship between alcohol misuse and impulsive behavior (12, 57–59).
While co-relative analyses account for a range of potential familial confounders, including genetic liability shared by AUD and suicide, they do not account for individual-level environmental factors that may jointly influence risk of both AUD and suicide. Such influences may contribute to increased risks attributed to AUD in co-relative models, leading to an overestimation of AUD’s putatively causal effect.
Finally, the findings may not be generalizable to other populations: Native-born Swedes may represent a more homogeneous culture than exists in more ethnically diverse countries such as the United States. However, as a robust association between AUD and suicidal behavior has been observed in the United States (16), any discrepancies may be quantitative rather than qualitative.
This study represents a well-powered analysis of the relationship between AUD and suicide, which is of substantial public health relevance. We present evidence, using complementary population-based, longitudinal, and co-relative analytic designs, that is consistent with the hypothesis that a substantial component of the association between AUD and suicide risk is potentially due to a causal mechanism, even after accounting for psychiatric comorbidity. Notably, this relationship is more prominent among women, among individuals with a recent AUD registration, and among those with an earlier onset of AUD. Our results have potential clinical relevance, as they indicate that AUD, even outside the context of psychiatric comorbidity, is a potent risk factor for suicide. While this association is strongest during the period close to an AUD registration, the effect persists for decades. Women, among whom death by suicide is less common overall, exhibit AUD-related risk comparable to men. These findings underscore the nuanced role of AUD in suicide risk and have implications for efforts aimed at reducing suicide and characterizing risk potential as a function of coexisting conditions.
1 Centers for Disease Control and Prevention: Leading Causes of Death Reports, 1981–2017, WISQARS database [online]. https://webappa.cdc.gov/sasweb/ncipc/leadcause.htmlGoogle Scholar
2 : Suicide data, 2016 [online]. https://www.who.int/mental_health/prevention/suicide/suicideprevent/en/Google Scholar
3 : Familial aggregation and coaggregation of suicide attempts and comorbid mental disorders in adults. JAMA Psychiatry (Epub ahead of print, March 27, 2019)Google Scholar
4 : Genetics of suicide attempts in individuals with and without mental disorders: a population-based genome-wide association study. Mol Psychiatry (Epub ahead of print, August 16, 2018)Google Scholar
5 : GWAS of suicide attempt in psychiatric disorders and association with major depression polygenic risk scores. Am J Psychiatry 2019; 176:651–660Link, Google Scholar
6 : Family genetic studies, suicide, and suicidal behavior. Am J Med Genet C Semin Med Genet 2005; 133C:13–24Crossref, Medline, Google Scholar
7 : Familial transmission of suicidal behavior. Psychiatr Clin North Am 2008; 31:157–177Crossref, Medline, Google Scholar
8 : Childhood adversity and risk of suicide: cohort study of 548 721 adolescents and young adults in Sweden. BMJ 2017; 357:j1334Crossref, Medline, Google Scholar
9 : Stressful life events and suicidal behavior in adults with alcohol use disorders: role of event severity, timing, and type. Drug Alcohol Depend 2012; 120:155–161Crossref, Medline, Google Scholar
10 : Interpersonal stressors, substance abuse, and suicide. J Nerv Ment Dis 1993; 181:80–85Crossref, Medline, Google Scholar
11 : Impulsivity, painful and provocative events, and suicide intent: testing the interpersonal theory of suicide. Suicide Life Threat Behav 2019; 49:1187–1195Crossref, Medline, Google Scholar
12 : Suicide risk associated with experience of violence and impulsivity in alcohol dependent patients. Sci Rep 2016; 6:19373Crossref, Medline, Google Scholar
13 : Alcohol-related risk of suicidal ideation, suicide attempt, and completed suicide: a meta-analysis. PLoS One 2015; 10:
14 : Alcohol consumption as a risk factor for suicidal behavior: a systematic review of associations at the individual and at the population level. Arch Suicide Res 2016; 20:489–506Crossref, Medline, Google Scholar
15 : Association of alcohol and drug use disorders and completed suicide: an empirical review of cohort studies. Drug Alcohol Depend 2004; 76(suppl):S11–S19Crossref, Medline, Google Scholar
16 : Predicting suicidal behavior from longitudinal electronic health records. Am J Psychiatry 2017; 174:154–162Link, Google Scholar
17 : Epidemiology of DSM-5 alcohol use disorder: results from the National Epidemiologic Survey on Alcohol and Related Conditions III. JAMA Psychiatry 2015; 72:757–766Crossref, Medline, Google Scholar
18 : Economic costs of excessive alcohol consumption in the US, 2006. Am J Prev Med 2011; 41:516–524Crossref, Medline, Google Scholar
19 : Global and regional mortality from 235 causes of death for 20 age groups in 1990 and 2010: a systematic analysis for the Global Burden of Disease Study 2010. Lancet 2012; 380:2095–2128Crossref, Medline, Google Scholar
20 : Alcohol use disorders and mortality: a systematic review and meta-analysis. Addiction 2013; 108:1562–1578Crossref, Medline, Google Scholar
21 : Risk of all-cause mortality in alcohol-dependent individuals: a systematic literature review and meta-analysis. EBioMedicine 2015; 2:1394–1404Crossref, Medline, Google Scholar
22 : Alcohol use disorder and mortality across the lifespan: a longitudinal cohort and co-relative analysis. JAMA Psychiatry 2016; 73:575–581Crossref, Medline, Google Scholar
23 : Global Status Report on Alcohol and Health, 2018. Luxembourg, World Health Organization, 2018 (https://www.who.int/substance_abuse/publications/global_alcohol_report/en/)Google Scholar
24 : The heritability of alcohol use disorders: a meta-analysis of twin and adoption studies. Psychol Med 2015; 45:1061–1072Crossref, Medline, Google Scholar
25 : Genetic and familial environmental effects on suicide: an adoption study of siblings. PLoS One 2013; 8:
26 : Smoking and major depression: a causal analysis. Arch Gen Psychiatry 1993; 50:36–43Crossref, Medline, Google Scholar
27 : An extended Swedish national adoption study of alcohol use disorder. JAMA Psychiatry 2015; 72:211–218Crossref, Medline, Google Scholar
28 : Suicide in obsessive-compulsive disorder: a population-based study of 36 788 Swedish patients. Mol Psychiatry 2017; 22:1626–1632Crossref, Medline, Google Scholar
29 : Clinical features of registry-ascertained alcohol use disorders that reflect familial risk. Drug Alcohol Depend 2016; 164:135–142Crossref, Medline, Google Scholar
30 : Method of attempted suicide as predictor of subsequent successful suicide: national long term cohort study. BMJ 2010; 341:c3222Crossref, Medline, Google Scholar
31 : Alcohol use disorders increase the risk of completed suicide, irrespective of other psychiatric disorders: a longitudinal cohort study. Psychiatry Res 2009; 167:123–130Crossref, Medline, Google Scholar
32 : Metaanalysis of mood and substance use disorders in proximal risk for suicide deaths. Suicide Life Threat Behav 2019; 49:278–292Crossref, Medline, Google Scholar
33 : Familial liability for eating disorders and suicide attempts: evidence from a population registry in Sweden. JAMA Psychiatry 2016; 73:284–291Crossref, Medline, Google Scholar
34 : Familial clustering of suicide risk: a total population study of 11.4 million individuals. Psychol Med 2011; 41:2527–2534Crossref, Medline, Google Scholar
35 : Risk of suicide after suicide attempt according to coexisting psychiatric disorder: Swedish cohort study with long term follow-up. BMJ 2008; 337:a2205Crossref, Medline, Google Scholar
36 : Sociodemographic, psychiatric, and somatic risk factors for suicide: a Swedish national cohort study. Psychol Med 2014; 44:279–289Crossref, Medline, Google Scholar
37 : Moderators of the relationship between alcohol dependence and suicide and medically serious suicide attempts: analyses of Canterbury Suicide Project data. Alcohol Clin Exp Res 2003; 27:1156–1161Crossref, Medline, Google Scholar
38 : Predisposing and precipitating factors for suicide among alcoholics: empirical review and conceptual integration. Alcohol Clin Exp Res 2004; 28(suppl):6S–17SCrossref, Medline, Google Scholar
39 : Substance-induced depression and independent depression in proximal risk for suicidal behavior. J Stud Alcohol Drugs 2014; 75:567–572Crossref, Medline, Google Scholar
40 : Indexing the “dark side of addiction”: substance-induced affective symptoms and alcohol use disorders. Addiction 2019; 114:139–149Crossref, Medline, Google Scholar
41 : Suicide: A Study in Sociology. Spaulding JA, Simpson G (trans.). Glencoe, Ill, Free Press, 1951Google Scholar
42 : Drug abuse-associated mortality across the lifespan: a population-based longitudinal cohort and co-relative analysis. Soc Psychiatry Psychiatr Epidemiol 2017; 52:877–886Crossref, Medline, Google Scholar
43 : Prevalence, correlates, and comorbidity of DSM-IV antisocial personality syndromes and alcohol and specific drug use disorders in the United States: results from the National Epidemiologic Survey on Alcohol and Related Conditions. J Clin Psychiatry 2005; 66:677–685Crossref, Medline, Google Scholar
44 : Prevalence, correlates, disability, and comorbidity of DSM-IV drug abuse and dependence in the United States: results from the National Epidemiologic Survey on Alcohol and Related Conditions. Arch Gen Psychiatry 2007; 64:566–576Crossref, Medline, Google Scholar
45 : Parental separation in childhood as a risk factor for depression in adulthood: a community-based study of adolescents screened for depression and followed up after 15 years. BMC Psychiatry 2017; 17:117Crossref, Medline, Google Scholar
46 : Parental separation in childhood and adult smoking in the 1958 British birth cohort. Eur J Public Health 2017; 27:723–728Medline, Google Scholar
47 : The role of depression in the differential effect of childhood parental divorce on male and female adult offspring suicide attempt risk. J Nerv Ment Dis 2010; 198:687–690Crossref, Medline, Google Scholar
48 : Childhood or adolescent parental divorce/separation, parental history of alcohol problems, and offspring lifetime alcohol dependence. Drug Alcohol Depend 2008; 98:264–269Crossref, Medline, Google Scholar
49 : Health-related factors associated with discrepancies between children’s potential and attained secondary school level: a longitudinal study. PLoS One 2016; 11:
50 : Childhood attention problems and socioeconomic status in adulthood: 18-year follow-up. Br J Psychiatry 2012; 201:20–25Crossref, Medline, Google Scholar
51 : Age-specific suicide mortality following non-fatal self-harm: national cohort study in Sweden. Psychol Med 2015; 45:1699–1707Crossref, Medline, Google Scholar
52 : Types of alcoholics, I: evidence for an empirically derived typology based on indicators of vulnerability and severity. Arch Gen Psychiatry 1992; 49:599–608Crossref, Medline, Google Scholar
53 : Gender and alcoholic subtypes. Alcohol Health Res World 1996; 20:56–62Medline, Google Scholar
54 : Types of alcoholics: concurrent and predictive validity of some common classification schemes. Br J Addict 1992; 87:1415–1431Crossref, Medline, Google Scholar
55 : Neurogenetic adaptive mechanisms in alcoholism. Science 1987; 236:410–416Crossref, Medline, Google Scholar
56 : Genetic heterogeneity and the classification of alcoholism. Adv Alcohol Subst Abuse 1988; 7:3–16Crossref, Medline, Google Scholar
57 : Genetic overlap between impulsivity and alcohol dependence: a large-scale national twin study. Psychol Med 2016; 46:1091–1102Crossref, Medline, Google Scholar
58 : Type I and type II alcoholism: an update. Alcohol Health Res World 1996; 20:18–23Medline, Google Scholar
59 : Inheritance of alcohol abuse: cross-fostering analysis of adopted men. Arch Gen Psychiatry 1981; 38:861–868Crossref, Medline, Google Scholar



