EEG and PET Changes in Anti-N-Methyl-d-Aspartic Acid Receptor Encephalitis
To the Editor: A-30-year-old woman with no prior medical history presented with a 2-week history of headaches, progressive encephalopathy, and dysautonomia. She was found to exhibit intermittent episodes of bizarre behavior characterized by moaning, crying, screaming, teeth clenching, and posturing without any surface EEG correlate. Her serum (1:10, normal<1:10) and CSF (1:5, normal<1:1) anti-N-methyl-d-asparate (NMDA) receptor antibodies were positive, while CSF Purkinje cell cytoplasmic antibody type 1 and 2; anti-neuronal nuclear AB type 1, 2, and 3; anti-glial nuclear AB type 1; amphiphysin AB; CRMP-5-IgG and blood anti-Ri; anti-Hu; anti-Ma1 and Ma2; anti-CV2; anti-YO; anti-Zic4; anti-amphiphysin; anti-alpha 3AChR; anti-LGI1; anti-VGCC; anti-VGKC; and anti-CASPR2 were negative. No primary tumor was identified on whole-body PET scan, and [18F]fluorodeoxyglucose (FDG) uptake in bilateral adnexa was thought to be physiological. A PET scan of her brain showed occipital and superior parietal hypometabolism bilaterally (Figure 1). While continuous EEG revealed no overt seizure activity, “extreme delta brush” pattern and rhythmic delta activity with superimposed rhythmic beta activity were noted (Figure 2).
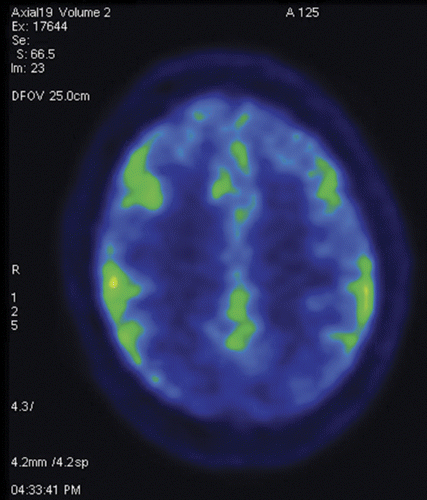
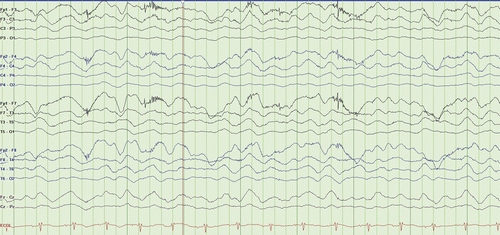
a Rhythmic delta activity at 1–3 Hz with superimposed bursts of rhythmic beta frequency activity “riding” on the top of the delta waves.
An FDG PET brain scan showing relative frontal and temporal glucose hypermetabolism associated with occipital hypometabolism (increased frontotemporal-to-occipital gradient) and extreme delta brush pattern on EEG has been reported in patients with NMDA-receptor antibody encephalitis (1, 2). Although abnormalities in brain FDG-PET have been reported to occur in autoimmune encephalitis of various etiologies as well as in neurodegenerative disorders such as frontotemporal dementias, in anti-NMDA encephalitis the fronto- and temporo-to-occipital gradient of cerebral FDG uptake correlates with disease severity and is reported to normalize after recovery (1). Recognition of these patterns in the appropriate clinical setting may therefore aid in the timely diagnosis of patients presenting with anti-NMDA receptor encephalitis.
1 : Fluorodeoxyglucose positron emission tomography in anti-N-methyl-D-aspartate receptor encephalitis: distinct pattern of disease. J Neurol Neurosurg Psychiatry 2012; 83:681–686Crossref, Medline, Google Scholar
2 : Extreme delta brush: a unique EEG pattern in adults with anti-NMDA receptor encephalitis. Neurology 2012; 79:1094–1100Crossref, Medline, Google Scholar



