In This Issue
Insurance Exchange Coverage of the Mentally Ill
Mechanisms to compensate insurance plans covering disproportionate numbers of chronically mentally ill patients in the planned health insurance exchanges are generally adequate, according to an analysis of past claims data (figure). After implementation of the Affordable Care Act (ACA) in 2014, report Barry et al. (p. Original article: 704), financial solvency will be largely ensured through “risk adjustment” by a pool of contributions from all plans in the state. The ACA also designates two temporary measures: commercial reinsurance purchased by each plan for costs above a certain threshold and “risk corridors” of payments flowing from the federal government to plans with higher than expected costs, in conjunction with payments coming in from plans with lower costs. In their editorial, Garfield and Druss (p. Original article: 675) note that some plans may still be underpaid despite these provisions, and they describe the ramifications of “adverse selection,” incentives for mentally ill patients to choose particular health insurance plans.
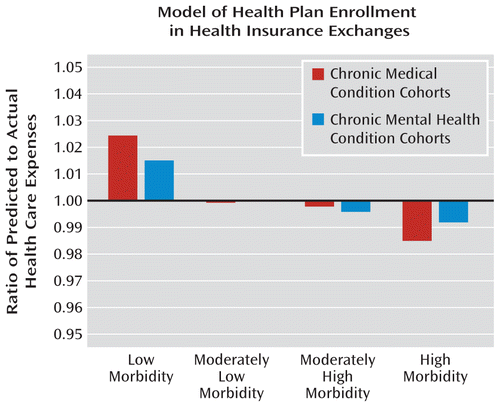
Under current risk adjustment provisions in the Affordable Care Act, health plans with the largest share of high morbidity enrollees with chronic mental health conditions are predicted to lose less than 1% of their mental health treatment costs on average (Barry et al., p. 704)
Chen et al. (CME, p. Original article: 735) separated smokers by their nicotinic receptor gene variants. Those with the low-risk genotype responded equally well to pharmacological treatments, including both nicotine replacement and bupropion, and nonpharmacological therapies. Those with the high-risk genotype, as identified by DNA sequencing, responded only to pharmacological treatments. Clinicians advising patients on smoking cessation can suspect genetic risk on the basis of early onset of heavy smoking and direct those smokers specifically to pharmacological treatments. Lotrich in an editorial (p. Original article: 681) points out that the chance of quitting successfully rises from about 25% to about 50% in patients with the high-risk genetic variant if they are treated with nicotine, bupropion, or their combination.
PTSD and substance use disorder are often comorbid in combat veterans. Abstinence has been historically required before PTSD treatment, to maximize the effect of PTSD treatment and minimize the risk that psychologically challenging treatments, such as exposure to combat stimuli, will lead to increased substance use. Back et al. (p. Original article: 688) proposed that co-treatment might be more effective and developed a 12-session program. Their Clinical Case Conference demonstrates partially successful use of the combination in a returning Marine. The patient was taught that the urge to abuse substances is triggered by cues, often the same that produce PTSD symptoms. The patient was taught over the 12 weekly sessions to monitor the rise and fall of both urges and PTSD symptoms after a period of cue exposure. Reductions of both alcohol use and PTSD symptoms, both the patients' goals, were achieved.
Bowie et al. (CME, p. Original article: 710) show results for patients with schizophrenia obtained from a sequence of cognitive remediation and skills training delivered as two 12-week blocks. The cognitive remediation immediately improved neurocognition, but the specific function skills training was needed to develop household and work skills. Effects were robust, with improvement seen in one of four patients treated. In an editorial, Lehman (p. Original article: 678) agrees that the combined treatment is more helpful than either alone but points out that even this very sophisticated treatment does not restore patients to full, real-world levels of function.



