In This Issue
Premenstrual Mood Changes in Bipolar Disorder
Women with bipolar disorder who reported having premenstrual exacerbation of mood symptoms had more depressive episodes and more severe symptoms over 1 year of follow-up than bipolar women without premenstrual mood changes. Among the 293 women studied by Dias et al. (p. Original article: 386), those with premenstrual exacerbation had greater severity of both depressive and manic/hypomanic symptoms. They also had shorter gaps between symptomatic intervals but were no more likely to have rapid cycling. The data demonstrate, states Payne in an editorial (p. Original article: 344), that the biggest risk factor for future bipolar illness is not achieving full remission.
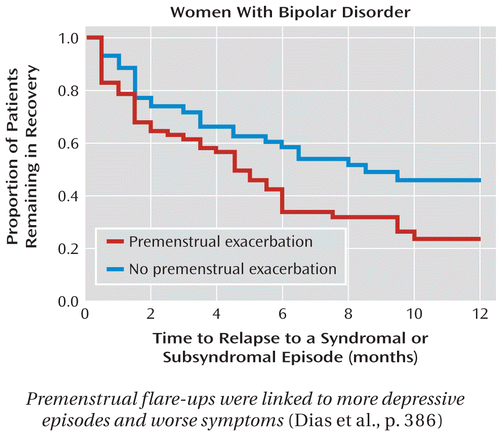
Premenstrual flare-ups were linked to more depressive episodes and worse symptoms (Dias et al., p. 386)
Measuring Functional Outcome of Cognition-Enhancing Drugs for Schizophrenia
The full UCSD Performance-Based Skills Assessment emerged as the front-runner among nine functionally relevant measures proposed for clinical trials of cognition-enhancing medications for schizophrenia. In addition to tests of cognition, the Food and Drug Administration requires a functionally meaningful coprimary outcome measure, but validated tests for this purpose have been lacking. Green et al. (CME, p. Original article: 400) describe a multiple-site study comparing five full instruments and four short forms administered to 166 patients with schizophrenia. The full forms of performance-based measures had stronger test properties than short forms or interview-based tests. All of the measures had acceptable test-retest reliability and were well tolerated, but correlations with community functioning were relatively low in all cases. Performance-based tests had stronger correlations with cognitive performance.
Agitated patients with schizophrenia in the emergency room who were smokers responded well to a 21-mg transdermal nicotine patch, in addition to regular antipsychotic treatment. Agitation was measured as excitement, hostility, tension, uncooperativeness, and poor impulse control. Effects were significant at 4 hours and were more marked in patients who were less nicotine dependent. Allen et al. (p. Original article: 395) speculate that the dose may have been too low for highly addicted patients. Schechter suggests in an editorial (p. Original article: 347) that nicotine replacement therapy in the emergency room might lessen agitation in smokers with other psychiatric disorders.
Mental Health Screening of Soldiers
Combat stress reactions in U.S. military personnel serving in Iraq were 29% less common among three infantry brigades screened for mental health conditions before deployment than among three unscreened brigades. Also, the rate of other psychiatric or behavioral problems during deployment was 78% lower in the screened brigades, and suicidal thoughts and behaviors were about half as common. Outcomes of the new Army program are reported by Warner et al. (CME, p. Original article: 378) for more than 20,000 soldiers in the 2007–2008 surge of forces in Iraq. In addition to determining fitness for deployment, the program creates follow-up plans to ensure continuity of care for deploying soldiers with mental health needs. The editorial by Hicks (p. Original article: 341) notes the value of recent changes in U.S. military programs that link mental health screening directly with proactive mental health care during the soldiers' deployment.
TMS is recommended by George and Post (p. Original article: 356) for moderately depressed patients who have failed to respond adequately or did not tolerate initial treatment of an acute episode of depression with an antidepressant, accompanied by a targeted psychotherapy. Typical stimulation parameters for 5 days per week, 4 to 8 week treatment are presented in the article itself. The treatment is not recommended for more seriously ill or refractory patients for whom ECT remains the treatment of choice.



