Reduced Pain Perception in Schizophrenia: A Case of an Undetected Intrathoracic Pencil
To the Editor: Although reduced pain sensitivity in schizophrenia has been reported many times (1), cases of foreign bodies remaining in situ with reduced pain are sparse. We present the case of a patient with schizophrenia who inserted a pencil into his thoracic wall. The pencil remained in position over the course of 3 weeks, causing only mild subjective distress.
Case Report
A 24-year-old man with schizophrenia was admitted to our hospital after a suicide attempt by clozapine overdose. Three weeks later, another patient on the ward reported that he had witnessed the patient injuring his own chest with a pencil. Immediate clinical examination revealed a small pinpoint lesion on the left thoracic wall in the axillary line and seventh intercostal space. Additional surgical examination and wound inspection, as well as an X-ray examination, did not reveal any other abnormalities (Figure 1A).
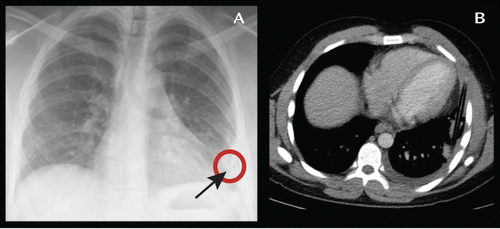
FIGURE 1. Imaging of Patient's Chest Performed on the Injury Day and After 3 Weeksa
a Panel A shows a posteroanterior thoracic X-ray; retrospectively, the correlate of a foreign body can be identified in the left basal lobe (arrow). Panel B shows an axial CT scan of the chest (mediastinal window). A 14 cm-long foreign body of tangential anterioposterior orientation is located in the left basal lobe.
Moderate signs of infection were treated successfully with sultamicillin, 375 mg b.i.d. for 7 days. During this phase, no subjective clinical symptoms were reported. Ten days later, we observed a rapid increase of infection symptoms. Despite fever and prominent infection signs from laboratory results, the patient reported only mild and inconstant subjective symptoms, such as dull unspecific abdominal pain. A second thoracic X-ray and an ultrasound examination of the abdomen showed no pathologies. A CT examination of the chest finally revealed a foreign body that was 14 cm in length and located in the left basal lobe (Figure 1B). Because of the organic structure of the foreign body, it had apparently been overlooked on both thoracic X-rays. A thoracotomy was performed immediately, and the pencil was removed without any other complications.
Discussion
Reduced pain perception is a widely reported but often neglected phenomenon in schizophrenia that can have vital implications for the physical and mental health of this patient population (2). Our case is unusual because the foreign body remained in situ for 3 weeks and caused only minor subjective distress.
Neurophysiological reports have repeatedly suggested altered pain perception in patients with schizophrenia. Greater pain tolerance and decreased activation in the pain processing regions of the brain have been demonstrated, and they cannot be solely explained by the effects of antipsychotic medication (3). These observations have been attributed to, among other things, information-processing abnormalities, decreased behavioral pain expression because of communication deficits, modifications in pain expression, and biochemical alterations in nociceptive parameters (4).
We suggest a closer consideration of the subjective perception of pain in routine medical care of schizophrenia patients, as altered pain perception could be an important risk factor for self-mutilation and injuries. Additionally, feeling pain is an important cue that facilitates the detection of acute and chronic physical conditions. In combination with the reduced participation in health maintenance that is common in patients with schizophrenia, impaired sensitivity to physical pain could contribute to delays in identification and treatment of somatic diseases and thus to higher morbidity and mortality rates (5).
1. : Altered pain perception in schizophrenia. Lancet 2010; 375:864Crossref, Medline, Google Scholar
2. : Pain insensitivity in schizophrenia: a neglected phenomenon and some implications. Schizophr Bull 1994; 20:235–248Crossref, Medline, Google Scholar
3. : Hypoalgesia in schizophrenia is independent of antipsychotic drugs: a systematic quantitative review of experimental studies. Pain 2008; 138:70–78Crossref, Medline, Google Scholar
4. : Pain perception in psychiatric disorders: a review of the literature. J Psychiatr Res 1994; 28:109–122Crossref, Medline, Google Scholar
5. : Physical illness in patients with severe mental disorders, I: prevalence, impact of medications and disparities in health care. World Psychiatry 2011; 10:52–77Crossref, Medline, Google Scholar



