In This Issue
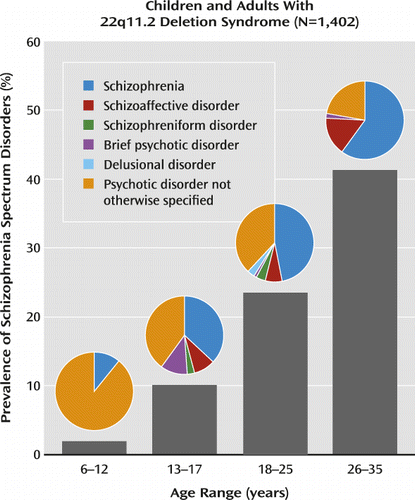
A collaborative study with 1,402 participants indicates that psychotic disorders are present in about 40% of adults over age 25 who have 22q11.2 deletion syndrome, a genetic disorder also known as velocardiofacial or DiGeorge syndrome. Attention deficit hyperactivity disorder is present in more than a third of these patients during childhood. Schneider et al. (p. Original article: 627) found that anxiety disorders are more common than mood disorders and that they interfere with daily living skills.
Virtual Reality for PTSD: Augmentation With d-Cycloserine or Alprazolam
A single dose of d-cycloserine or alprazolam before each session of virtual reality therapy did not increase overall symptom improvement more than adjunctive placebo in 156 veterans with combat-related posttraumatic stress disorder (PTSD). The alprazolam group actually had higher symptom ratings at the end of treatment and a higher rate of PTSD diagnosis at 3-month follow-up, compared to the placebo group. Rothbaum et al. (p. Original article: 640) did observe two advantages for d-cycloserine: greater decreases in salivary cortisol and startle response and an association between extinction learning and symptom improvement. Explanations proposed by editorialist Neylan (p. Original article: 597) for the mixed findings include the possibility that d-cycloserine’s effects are not strong enough or that therapeutic improvement depends on more than extinction learning.
A behavioral group intervention for parents of young children with especially severe antisocial behavior produces long-lasting decreases in antisocial behavior and character traits. Parents of children who were referred for treatment at age 3–7 were offered the “Incredible Years” basic videotape program, which produced better outcomes than brief supportive therapy at the end of treatment and at follow-up at age 10–17. Scott et al. (CME, p. Original article: 649) discovered, in addition, that this parental training improved oppositional defiant behavior, reading, and parental warmth and supervision. A similar study targeting at-risk children identified by community screening did not produce corresponding improvements. Editorialist Weisz (p. Original article: 600) describes how effective parenting interventions produce effects beyond the children to larger social systems.
Children with the new DSM-5 diagnosis of disruptive mood dysregulation disorder are more likely than healthy children to become young adults with anxiety or depressive disorders, general health problems, risky or illegal behaviors, financial problems, or social impairment. They also fare worse than children or adolescents with other psychiatric disorders, in terms of early adulthood health problems and comorbid psychiatric diagnoses, report Copeland et al. (CME, p. Original article: 668). In his editorial, McGough (p. Original article: 607) differentiates childhood disruptive mood dysregulation disorder from bipolar disorder on the basis of nonepisodic irritability, the brain mechanisms of which may ultimately hold the key to effective treatment.
Intensive family-focused treatment was not more effective than brief family psychoeducation for adolescents with bipolar I or II disorder who were also receiving pharmacotherapy. The family-focused therapy tested by Miklowitz et al. (p. Original article: 658) lasted 9 months and consisted of psychoeducation, communication enhancement, and problem-solving training. Patients in both treatment groups received medication prescribed according to a standardized protocol. The negative finding contradicts most earlier results, and editorialist Swartz (p. Original article: 603) explains how such a discrepancy can ultimately advance treatment by spurring research on, for instance, use of guideline-consistent pharmacotherapy, adolescents’ specific needs, or treatments tailored to specific patient subgroups.



