Computer-Assisted Delivery of Cognitive-Behavioral Therapy: Efficacy and Durability of CBT4CBT Among Cocaine-Dependent Individuals Maintained on Methadone
Abstract
Objective
A previous pilot trial evaluating computer-based training for cognitive-behavioral therapy (CBT4CBT) in 77 heterogeneous substance users (alcohol, marijuana, cocaine, and opioids) demonstrated preliminary support for its efficacy in the context of a community-based outpatient clinic. The authors conducted a more definitive trial in a larger, more homogeneous sample.
Method
In this randomized clinical trial, 101 cocaine-dependent individuals maintained on methadone were randomly assigned to standard methadone maintenance or methadone maintenance with weekly access to CBT4CBT, with seven modules delivered within an 8-week trial.
Results
Treatment retention and data availability were high and comparable across the treatment conditions. Participants assigned to the CBT4CBT condition were significantly more likely to attain 3 or more consecutive weeks of abstinence from cocaine (36% compared with 17%; p<0.05, odds ratio=0.36). The group assigned to CBT4CBT also had better outcomes on most dimensions, including urine specimens negative for all drugs, but these reached statistical significance only for individuals completing the 8-week trial (N=69). Follow-up data collected 6 months after treatment termination were available for 93% of the randomized sample; these data indicate continued improvement for those assigned to the CBT4CBT group, replicating previous findings regarding its durability.
Conclusions
This trial replicates earlier findings indicating that CBT4CBT is an effective adjunct to addiction treatment with durable effects. CBT4CBT is an easily disseminable strategy for broadening the availability of CBT, even in challenging populations such as cocaine-dependent individuals enrolled in methadone maintenance programs.
Cognitive-behavioral therapy (CBT) has a comparatively strong level of empirical support across a range of psychiatric disorders (1), including substance use disorders (2, 3). Despite evidence of positive and durable outcomes (4, 5), CBT remains rarely implemented in the range of settings where individuals with substance use disorders are treated (6).
The potential of computer-assisted therapies has led to a burgeoning of new Internet and computer-assisted approaches for a range of psychiatric disorders (14). There are now meta-analytic evaluations of computer and Internet interventions for multiple disorders, including depression (15) and anxiety (16) as well as illicit drug use (17), smoking (18), and alcohol use (19).
A preliminary randomized evaluation of computer-based training for CBT (CBT4CBT) as an adjunct to standard addiction treatment compared it to standard treatment alone for 77 individuals seeking outpatient treatment for a range of substance use disorders (22). Participants were predominantly dependent on alcohol, cocaine, marijuana, or opioids, with the use of multiple substances reported by most participants (80%). At the end of the 8-week trial, participants assigned to the CBT4CBT condition submitted significantly more urine specimens that were negative for any type of drugs and tended to have longer continuous periods of abstinence during treatment. A 6-month follow-up of 82% of the intention-to-treat sample indicated significantly better durability of effects of CBT4CBT over standard treatment for both self-report and urinalysis data (23). The limitations of this preliminary study included the small sample size and highly heterogeneous sample that varied greatly in both type and severity of substance use at baseline.
In this article, we describe the primary outcome results from a larger randomized clinical trial of CBT4CBT in a more homogeneous, but highly challenging, clinical population, i.e., cocaine-dependent individuals maintained on methadone. Cocaine use is among the most prevalent and intractable problems within methadone maintenance programs (24, 25), and it is associated with a wide range of problems including HIV, hepatitis C, and multiple other morbidities (26). Methadone treatment programs in the United States face rapidly growing censuses and patients presenting with more complex and severe problems and fewer resources with which to treat them.
In the present trial, cocaine-dependent individuals who were stabilized on methadone were randomly assigned to standard methadone maintenance (treatment as usual) or treatment as usual plus CBT4CBT over a period of 8 weeks. Given the established efficacy of clinician-delivered CBT across a range of addictions (2, 3) and the very limited availability of empirically validated therapies in many community-based settings, CBT4CBT was evaluated in terms of how it is most likely be used in these settings, that is, as a stand-alone addition to regular methadone services. The primary hypothesis was that individuals assigned to CBT4CBT would reduce their frequency of cocaine and other substance use and submit fewer positive urine toxicology screens than individuals randomly assigned to treatment as usual. We also hypothesized that the effects of CBT4CBT would be durable relative to treatment as usual through a 6-month follow-up. Finally, we compared the groups regarding the effects of treatment on HIV risk behavior because an HIV risk-reduction component was added to CBT4CBT to address the high rate of drug- and sex-related risk behaviors in this population (27, 28).
Method
Participants
Participants were recruited from one of the methadone maintenance programs of the APT Foundation, the largest provider of methadone maintenance services in New Haven, Conn. Participants were English-speaking adults who were stabilized on methadone (the same dose for >2 months) and who met DSM-IV criteria for current (within the past 30 days) cocaine dependence. As in our previous trial, exclusion criteria were minimized in order to facilitate the recruitment of a broad and clinically representative group of individuals enrolled in this setting. Thus, individuals were excluded only if they 1) failed to meet DSM-IV criteria for current cocaine dependence, 2) had an untreated or unstabilized psychotic disorder or had current suicidal or homicidal ideation such that more intensive treatment was indicated, or 3) could not read at a 6th-grade level (required for provision of written informed consent and completion of assessment instruments).
As depicted in the CONSORT diagram (Figure 1), 101 of the 154 individuals screened were determined to be eligible for the study, provided written informed consent that was approved by the Yale University School of Medicine Human Investigations Committee, and were randomly assigned to either treatment as usual or CBT4CBT. We used a computerized urn randomization program (29) to balance treatment groups with respect to gender, ethnicity, education level, and frequency of cocaine use at baseline.
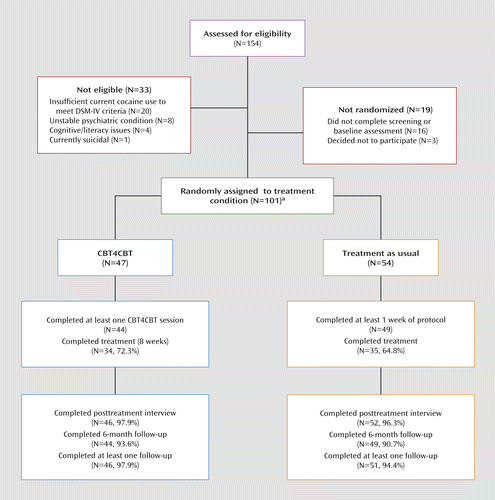
a One additional individual did not proceed to random treatment assignment as a result of uncertain eligibility.
Treatments
All participants were offered standard treatment at the clinic, which consisted of daily methadone maintenance and weekly group sessions. Participants also met twice weekly with an independent research assistant who collected urine specimens, assessed recent substance use, and monitored other clinical symptoms. Those randomly assigned to the CBT4CBT condition were provided access to the program on a dedicated computer in a private room within the clinic. The research assistant guided participants through their initial use of the CBT4CBT program and was available if needed to answer questions and assist participants each time they accessed the program. Participants accessed the program through a login and password system to protect confidentiality.
As described earlier (22), the CBT4CBT program was user friendly, required no previous experience with computers or reading skills (any material presented in text was also read by an on-screen narrator), and collected no protected health information. The program was media rich, using games, cartoons, quizzes, and other interactive exercises to teach and model the effective use of skills and strategies. At its core was a series of videos presenting connected scenes of engaging characters portrayed by professional actors for each topic. These characters first experience a common risky situation or problem and then, after the skill is presented as described above, demonstrate using the targeted skill to successfully negotiate the situation without resorting to drug use.
Assessments
Participants were assessed by a research assistant before treatment; twice weekly during treatment; at the 8-week treatment termination point; and 1, 3, and 6 months after the termination point. Participants were administered the Structured Clinical Interview for DSM-IV (SCID) (30) before treatment randomization to establish substance use and other psychiatric diagnoses. The Substance Use Calendar, similar to the Timeline Followback (31), was administered weekly during treatment to collect day-by-day self-reports of drug and alcohol use for the 28-day period before randomization as well as throughout the 56-day treatment phase and the 6-month follow-up. HIV risk behaviors were assessed using the Risk Assessment Battery (32).
Participant self-reports of drug use were verified through urine toxicology screens that were obtained at every assessment visit. Of the 875 urine specimens collected during the treatment phase of the study (between days 4 and 56), the majority (84.7%) were consistent with participant self-report; only 106 (12%) were positive for cocaine in cases where the participant had denied recent use during the 3-day period that cocaine metabolites are typically detectable in urine. Finally, given that a weakness of computerized therapy literature is the lack of attention to potential adverse events associated with computerized therapies (20, 21), possible adverse events and hospitalizations were monitored and reviewed regularly by the Data Safety Monitoring Board using procedures worked out in previous multisite behavioral trials (33).
Data Analyses
The primary outcome measures were change in self-reported drug use over time (days of cocaine use by week); results of urine toxicology screens (operationalized as the percentage of drug-negative urine samples collected during treatment); and attainment of 3 or more weeks of continuous abstinence, a variable found in multiple trials to be predictive of better long-term cocaine outcomes (34). Secondary outcomes included reductions in self-reported HIV risk behaviors. The principal data analytic strategy was random-effects regression analysis for the longitudinal outcome (days of cocaine use by week during the 8 weeks of active treatment) and analysis of variance (ANOVA) for the other primary outcome variables (percentage of drug-negative urine specimens and self-reported abstinence) for the 101 participants who were randomly assigned to treatment (intention-to-treat sample), the 93 participants who initiated treatment (treatment-exposed), and the 69 who completed treatment. Follow-up data were evaluated using a single piecewise random-effects regression model (35) to assess change from pretreatment through follow-up, which included treatment phase and associated interactions as independent variables. The results were highly consistent across analysis subsamples.
Results
Sample Description
Table 1 summarizes the baseline demographic and substance use characteristics and psychiatric diagnoses of the 101 participants. Of these, 60% were female; 30% identified themselves as African American, 60% as European American, and 8% as Latin American. Most participants (88%) were single or divorced, 89% were unemployed, and 71% had completed high school. The majority (77%) received some public assistance, and 17% were on probation or parole. Participants used cocaine an average of 15 days per month and had been using cocaine for approximately 11 years. They reported using marijuana for about 2.5 days per month and alcohol less than 1 day per month. ANOVA and chi-square analyses indicated no significant differences by treatment condition on these and other baseline variables as presented in Table 1.
| Treatment Group | Analysisa | |||||
|---|---|---|---|---|---|---|
| Variables | CBT4CBT (N=47)b | Treatment as Usual (N=54)c | χ2 | p | ||
| Categorical | N | % | N | % | ||
| Female | 28 | 59.6 | 33 | 61.1 | 0.025 | 0.87 |
| Ethnicity | ||||||
| European American | 28 | 59.6 | 33 | 61.1 | 2.57 | 0.63 |
| African American | 16 | 34 | 14 | 25.9 | ||
| Latin American | 3 | 6.4 | 5 | 9.3 | ||
| Native American, other | 0 | 0 | 2 | 3.9 | ||
| Completed high school | 31 | 66 | 41 | 75.9 | 1.22 | 0.27 |
| Never married/living alone | 41 | 87.2 | 48 | 88.9 | 0.07 | 0.80 |
| Unemployed | 43 | 91.5 | 47 | 87 | 0.51 | 0.47 |
| On probation or parole | 7 | 14.9 | 10 | 18.5 | 0.24 | 0.63 |
| Major depression, lifetimed | 15 | 31.9 | 14 | 25.9 | 0.44 | 0.51 |
| Anxiety disorder, lifetimed | 16 | 34 | 16 | 29.6 | 0.23 | 0.63 |
| Current alcohol use disorderd | 1 | 2.2 | 3 | 5.7 | 0.77 | 0.38 |
| Continuous | Mean | SD | Mean | SD | F | p |
| Age (years) | 42.7 | 9.5 | 41.3 | 9.7 | 0.55 | 0.46 |
| Years of regular cocaine use | 12.6 | 7.1 | 10.6 | 9.6 | 1.34 | 0.25 |
| Days of cocaine use, past 28 | 15.5 | 9.5 | 13.9 | 9.3 | 0.79 | 0.38 |
| Days of heroin use, past 28 | 1.2 | 4.2 | 2.0 | 5.2 | 0.77 | 0.38 |
| Days of marijuana use, past 28 | 1.8 | 5.3 | 3.1 | 7.2 | 1.06 | 0.31 |
| Days of alcohol use, past 28 | 0.5 | 0.5 | 0.4 | 0.5 | 0.60 | 0.44 |
| Age of first use of cocaine (years) | 20.0 | 5.3 | 20.1 | 5.1 | 0.00 | 0.99 |
| Addiction Severity Index scores | ||||||
| Medical compositee | 0.4 | 0.4 | 0.4 | 0.4 | 0.13 | 0.72 |
| Employment composite | 0.7 | 0.2 | 0.8 | 0.3 | 0.46 | 0.50 |
| Alcohol composite | 0.1 | 0.1 | 0.0 | 0.1 | 0.89 | 0.35 |
| Cocaine composite | 0.7 | 0.2 | 0.6 | 0.3 | 0.37 | 0.55 |
| Other drug composite | 0.1 | 0.1 | 0.1 | 0.1 | 1.04 | 0.31 |
| Legal composite | 0.1 | 0.1 | 0.1 | 0.2 | 0.83 | 0.36 |
| Family composite | 0.1 | 0.2 | 0.1 | 0.2 | 0.59 | 0.45 |
| Psychological composite | 0.2 | 0.2 | 0.1 | 0.2 | 1.19 | 0.28 |
| Days paid for working, past 28 | 3.4 | 6.7 | 2.6 | 6.5 | 0.38 | 0.54 |
| Lifetime number of arrests | 11.7 | 14.0 | 11.0 | 14.4 | 0.06 | 0.82 |
| Number of prior outpatient treatment episodes | 3.6 | 3.7 | 3.0 | 6.2 | 0.36 | 0.55 |
| Number of prior inpatient treatment episodes | 4.2 | 6.4 | 3.1 | 3.8 | 1.04 | 0.31 |
| Methadone dose at baseline, mg | 84.02 | 28.32 | 83.4 | 27.4 | 0.01 | 0.91 |
Treatment Implementation, Retention, and Data Availability by Condition
Of the 93 individuals who initiated the protocol, 69 (74%) completed the 8-week treatment protocol (34 in the CBT4CBT condition and 35 in treatment as usual). Posttreatment data were collected from 98 individuals (97% of the intention-to-treat sample). In all, 96% of the intention-to-treat sample was reached for at least one follow-up, and 92% were reached for the 6-month follow-up, as the vast majority (97%) were still enrolled in the methadone program. Hence, analyses of the primary substance use outcomes were not constrained by differential rates of attrition nor by data availability. No participant deaths occurred during the trial, and rates of serious adverse events (typically overnight hospitalizations) did not differ by treatment condition either within treatment or during follow-up (Table 2). None of the adverse events were determined to be protocol related by the Data Safety Monitoring Board.
| Treatment Group | Analysis | |||||
|---|---|---|---|---|---|---|
| Variable | CBT4CBT (N=47) | Treatment as Usual (N=54) | F | p | ||
| Mean | SD | Mean | SD | |||
| Days in treatment (maximum=56) | 46.7 | 17.2 | 43.9 | 19.9 | 0.58 | 0.45 |
| Urine specimens provided | 9.5 | 5.0 | 10.8 | 2.8 | 1.81 | 0.18 |
| Total individual sessions within treatment | 3.7 | 1.8 | 4.2 | 2.8 | 0.8 | 0.38 |
| Total group sessions within treatment | 6.3 | 8.6 | 5.2 | 7.3 | 0.3 | 0.56 |
| N | % | N | % | |||
| Participants with one or more serious adverse events within treatmenta | 3 | 6.4 | 1 | 1.9 | 1.4 | 0.24 |
| Participants with one or more serious adverse events during follow-up | 8 | 17.0 | 6 | 11.1 | 0.8 | 0.39 |
As summarized in Table 2, the levels of exposure to the standard counseling services offered in the program were also comparable in both groups, with individuals assigned to CBT4CBT completing a mean of 47 days and those assigned to treatment as usual completing 44 days of the 56-day protocol. Of individuals who initiated the CBT4CBT program, the mean number of completed computer sessions was 5.1 (SD=2.3) of the seven modules offered (73%). Participants spent an average of 35 minutes (SD=8.6) per session working with each module and tended to complete the modules in the order presented (e.g., 44/44 participants completed module 1 [patterns of use and functional analysis], 38 completed module 2 [coping with craving], 34 completed module 3 [refusing offers], 31 completed module 4 [problem solving], 26 completed module 5 [addressing cognitions], 28 completed module 6 [decision making], and 23 completed the HIV risk-reduction module). Most participants (84.1%) completed at least one of the six weekly homework assignments, and overall they completed an average of 2.9 homework assignments (maximum=6, SD=2.2).
Effects of Treatment on Cocaine and Other Drug Use: Within Treatment and at 6-Month Follow-Up
Within-treatment cocaine use outcomes were consistently better in the group assigned to CBT4CBT compared with those assigned to treatment as usual alone.
| Treatment Group | Analysis | ||||||
|---|---|---|---|---|---|---|---|
| Variable | CBT4CBT (N=47) | Treatment as Usual (N=54) | F or χ2 | p | Effect Sizea | ||
| Mean | SD | Mean | SD | ||||
| Intention-to-treat sampleb | |||||||
| Percent days of abstinence, self-report | 65.3 | 29.4 | 56.6 | 31.6 | 1.97 | 0.16 | 0.28 |
| Percent cocaine-free urine samples | 24.4 | 35.5 | 19.0 | 28.7 | 2.36 | 0.13 | 0.19 |
| Percent drug-free urine samples | 22.5 | 30.3 | 11.9 | 24.0 | 3.45 | 0.06 | 0.44 |
| N | % | N | % | ||||
| 3 or more weeks of continuous abstinence | 17 | 36.2 | 9 | 17.0 | 4.77 | 0.03 | 0.36 |
| Mean | SD | Mean | SD | ||||
| Individuals completing treatmentc | |||||||
| Percent days of abstinence, self-report | 67.8 | 26.4 | 59.4 | 27.7 | 1.65 | 0.23 | 0.30 |
| Percent cocaine-free urine samples | 33.3 | 34.2 | 18.8 | 24.4 | 4.14 | 0.05 | 0.59 |
| Percent drug-free urine samples | 26.7 | 29.8 | 12.4 | 21.9 | 5.16 | 0.03 | 0.65 |
| N | % | N | % | ||||
| 3 or more weeks of continuous abstinence | 11 | 32.4 | 3 | 8.0 | 6.03 | 0.01 | 0.20 |
Longitudinal outcomes (i.e., change in frequency of cocaine use by time), which paralleled those of the “static” summary outcomes (percentage of negative urine samples or days abstinent), are presented in Figure 2. The random-effects regression analyses resulted in a significant effect for time, indicating a reduction in the frequency of cocaine use over the course of treatment for the sample as a whole (F=42.5, df=1, 792.6, p<0.001) and a significant treatment group-by-time effect (F=10.8, df=1, 792, p=0.002). This result indicated greater reduction in cocaine use by time for the participants assigned to CBT4CBT compared with treatment as usual.
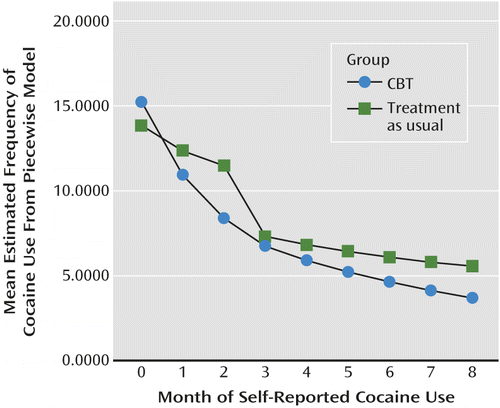
a Estimates from random regression analyses by treatment assignment.
The follow-up outcomes indicate relative durability of the effects of CBT4CBT through the 6-month follow-up assessment; these results are also depicted in Figure 2. The piecewise random-effects regression analyses revealed a significant overall reduction in the frequency of cocaine use by month from the baseline assessment through the 6-month follow-up (log F=35.92; p<0.001), where, as expected, the rate of change within treatment was greater than the rate of change during follow-up (effect of phase, F=4.41; p=0.04). Overall, participants assigned to the CBT4CBT condition had a greater reduction in cocaine use compared with those assigned to treatment as usual (group-by-log time, 8.49; p<0.001).
Effects on HIV Risk Behavior
To evaluate the possible effects of adding the HIV or sexually transmitted disease risk-reduction module, self-reported levels of risk were evaluated with the Risk Assessment Battery (32). Although overall risk levels were low, and the results of an analysis of group-by-time effects did not attain significance, a marked decrease was observed in self-reported drug risk behavior for individuals assigned to CBT4CBT relative to treatment as usual. However, this effect did not persist during follow-up. Sex-related risk behaviors did not change appreciably in either condition.
Discussion
This randomized clinical trial of CBT4CBT as an adjunct to methadone maintenance therapy for 101 cocaine-dependent individuals indicated improved cocaine and drug use outcomes relative to standard methadone maintenance treatment alone (treatment as usual). Participants in the CBT4CBT condition were significantly more likely to attain 3 or more consecutive weeks of abstinence within treatment, an outcome indicator associated with better long-term cocaine use outcomes and general functioning across multiple trials. The results of a 6-month follow-up also indicated significant enduring benefit of CBT4CBT relative to treatment as usual over time. The effects of treatment on the percentage of urine specimens that were negative for all illicit drugs also approached statistical significance.
To our knowledge, this study represents the first replication, via randomized clinical trial, of a computer-assisted therapy for addiction (20), which is significant because replication studies, while critical to the advancement of science (36), are comparatively rare in the clinical science literature (37). Moreover, evidence standards for both pharmacological and behavioral therapies require replication before a therapy can be considered evidence based (38). Furthermore, we found these favorable outcomes for CBT4CBT in a particularly highly challenging population, methadone-maintained cocaine-dependent individuals, many of whom used other drugs in addition to cocaine. Other than contingency management, few behavioral or pharmacological treatments have resulted in a positive effect, much less a durable one, in this population (39). Finally, while the overall magnitude of drug use reduction in this sample was modest, the results do compare favorably with those of other randomized trials in this population (39–41), and the effect sizes were comparable with those found in the initial trial of CBT4CBT (range=0.45–0.59).
The durability of effects of CBT4CBT reported for the initial trial (23), and consistent with clinician-delivered CBT (4), was also replicated here. Few, if any, other behavioral therapies, and no pharmacological therapies for cocaine dependence, have demonstrated durable effects once terminated. As addictions are a chronic relapsing condition, the durability of effects is a particularly important feature of any empirically validated therapy (42).
The effect of the HIV risk-reduction module on risk behavior in this sample was more mixed. As it was the last module delivered, only half of those individuals assigned to CBT4CBT completed it (22/44). The level of self-reported drug-related risk behaviors, as assessed by the Risk Assessment Battery, fell to 0 in the CBT4CBT group by the end of treatment, but analyses did not indicate significant differences by treatment condition. An ongoing trial is evaluating the efficacy of this module, delivered alone, on the frequency of high-risk behaviors relative to standard HIV risk-reduction groups in the context of a methadone maintenance program.
The strengths of this protocol include methodological features of importance for rigorous clinical trials of computer-assisted therapies (20, 21) and therapist-delivered behavioral therapies more broadly (38). These include randomization to treatment, 6-month follow-up for 92% of the sample, assessment of primary outcomes using both a urine toxicology screen and validated self-report instruments, adequate sample size with intention-to-treat analyses of outcomes using appropriate statistical procedures, monitoring and reporting of adverse events, and requiring all participants to meet standardized diagnostic criteria for cocaine and opioid dependence. Moreover, in contrast to many computer-delivered interventions where low levels of adherence typically limit inferences that can be drawn regarding effectiveness (18, 20, 43), the level of engagement with the CBT4CBT program was comparatively high, as participants completed an average of 73% of sessions offered.
This study had several limitations as well. First, CBT4CBT was evaluated as an add-on to treatment, and thus conditions were not balanced for time spent and attention. Furthermore, it cannot yet be concluded that the effects of CBT4CBT are comparable with those of individual clinician-delivered CBT. For the intention-to-treat sample, the results of study treatments on overall rates of cocaine-negative and all drug-negative urine specimens approached but did not reach statistical significance. However, the rates of negative urine screens did reach significance in the sample of individuals completing treatment, highlighting the importance of retention in evaluation treatment outcomes. Moreover, these effects were observed in the context of participants also attending group and individual counseling at least once per week while the trial was ongoing.
Overall, this extension of an initial trial of CBT4CBT to a more homogeneous (in terms of all participants meeting criteria for current cocaine dependence in addition to opioid dependence) but highly challenging clinical population is another milestone in the validation of this cost-effective (44), easily disseminable approach. A major strength of the CBT4CBT approach itself is the ease of implementation of the computer-assisted therapy. Given the multiple roadblocks to implementation of empirically supported therapies into practice, this study confirms that CBT4CBT may provide a safe, inexpensive, and sustainable option for doing so.
The next steps for this line of research include less-tightly controlled effectiveness trials that address feasibility and outcomes when delivered in clinical settings. Another line of research would involve evaluating the efficacy of CBT4CBT with limited clinician involvement (that is, as a stand-alone approach rather than as a clinician extender) as well as direct comparisons of computer-delivered CBT4CBT with CBT when delivered by well-trained and closely supervised clinicians, all of which are ongoing in our clinics. In addition, we are exploring the utility of the program when adapted for use by other clinical populations (e.g., for alcohol-dependent or Spanish-speaking populations). Ultimately, we hope that carefully studied approaches like CBT4CBT may provide a new paradigm for treating a wide variety of addictive disorders in a broad range of settings.
1 : What Works for Whom? A Critical Review of the Psychotherapy Literature, 2nd ed. New York, Guilford Press, 2005Google Scholar
2 : A meta-analytic review of psychosocial interventions for substance use disorders. Am J Psychiatry 2008; 165:179–187Link, Google Scholar
3 : Cognitive-behavioral treatment with adult alcohol and illicit drug users: a meta-analysis of randomized controlled trials. J Stud Alcohol Drugs 2009; 70:516–527Crossref, Medline, Google Scholar
4 : One-year follow-up of psychotherapy and pharmacotherapy for cocaine dependence: delayed emergence of psychotherapy effects. Arch Gen Psychiatry 1994; 51:989–997Crossref, Medline, Google Scholar
5 : Is cognitive-behavioral therapy more effective than other therapies? a meta-analytic review. Clin Psychol Rev 2010; 30:710–720Crossref, Medline, Google Scholar
6
7 : National survey of psychotherapy training in psychiatry, psychology, and social work. Arch Gen Psychiatry 2006; 63:925–934Crossref, Medline, Google Scholar
8 : Contemporary addiction treatment: a review of systems problems for adults and adolescents. Biol Psychiatry 2004; 56:764–770Crossref, Medline, Google Scholar
9 : We don’t train in vain: a dissemination trial of three strategies of training clinicians in cognitive-behavioral therapy. J Consult Clin Psychol 2005; 73:106–115Crossref, Medline, Google Scholar
10 : Manual-guided cognitive-behavioral therapy training: a promising method for disseminating empirically supported substance abuse treatments to the practice community. Psychol Addict Behav 2001; 15:83–88Crossref, Medline, Google Scholar
11
12 : Computer-assisted therapy in psychiatry: be brave—it’s a new world. Curr Psychiatry Rep 2010; 12:426–432Crossref, Medline, Google Scholar
13 : A promising debut for computerized therapies. Am J Psychiatry 2008; 165:793–795Link, Google Scholar
14 : Hands on Help: Computer-Aided Psychotherapy. Hove, UK, Psychol Press, 2007Crossref, Google Scholar
15 : Internet-based cognitive behavior therapy for symptoms of depression and anxiety: a meta-analysis. Psychol Med 2007; 37:319–328Crossref, Medline, Google Scholar
16 : Computer therapy for the anxiety and depressive disorders is effective, acceptable, and practical health care: a meta-analysis. PLoS ONE 2010; 5:e13196Crossref, Medline, Google Scholar
17 : Internet and computer-based interventions for cannabis use: a meta-analysis. Drug Alcohol Depend 2013; 133:295–304Crossref, Medline, Google Scholar
18 : Computer-delivered interventions for alcohol and tobacco use: a meta-analysis. Addiction 2010; 105:1381–1390Crossref, Medline, Google Scholar
19 : Can stand-alone computer-based interventions reduce alcohol consumption? a systematic review. Addiction 2011; 106:267–282Crossref, Medline, Google Scholar
20 : A methodological analysis of randomized clinical trials of computer-assisted therapies for psychiatric disorders: toward improved standards for an emerging field. Am J Psychiatry 2011; 168:790–799Link, Google Scholar
21 : Is computerized CBT really helpful for adult depression? a meta-analytic re-evaluation of CCBT for adult depression in terms of clinical implementation and methodological validity. BMC Psychiatry 2013; 13:113Crossref, Medline, Google Scholar
22 : Computer-assisted delivery of cognitive-behavioral therapy for addiction: a randomized trial of CBT4CBT. Am J Psychiatry 2008; 165:881–888Link, Google Scholar
23 : Enduring effects of a computer-assisted training program for cognitive behavioral therapy: a 6-month follow-up of CBT4CBT. Drug Alcohol Depend 2009; 100:178–181Crossref, Medline, Google Scholar
24 : Opioid maintenance treatment, in The American Psychiatric Publishing Textbook of Substance Abuse Treatment, 4th ed. Edited by Galanter MKleber HD. Washington, DC, American Psychiatric Publishing, 2008, pp 289–308Google Scholar
25 : Methadone maintenance, in Substance Abuse: A Comprehensive Textbook, 4th ed. Edited by Lowinson JRuiz PMillman RBLangrod JG. Philadelphia, Lippincott Williams & Wilkins, 2005, pp 616–633Google Scholar
26 : The Effectiveness of Methadone Maintenance Treatment. New York, Springer-Verlag, 1991Crossref, Google Scholar
27 : The effects of psychosocial services in substance abuse treatment. JAMA 1993; 269:1953–1959Crossref, Medline, Google Scholar
28 : A randomized clinical trial of a manual-guided risk reduction intervention for HIV-positive injection drug users. Health Psychol 2003; 22:223–228Crossref, Medline, Google Scholar
29 : Ensuring balanced distribution of prognostic factors in treatment outcome research. J Stud Alcohol Suppl 1994; 12(suppl 12):70–75Crossref, Medline, Google Scholar
30 : Structured Clinical Interview for DSM-IV, Patient Edition. Washington, DC, American Psychiatric Press, 1995Google Scholar
31 : Reliability of the Timeline Followback for cocaine, cannabis, and cigarette use. Psychol Addict Behav (Epub ahead of print, Dec 31, 2012)Google Scholar
32 : Preparations for AIDS vaccine trials: an automated version of the Risk Assessment Battery (RAB): enhancing the assessment of risk behaviors. AIDS Res Hum Retroviruses 1994; 10(suppl 2):S281–S283Medline, Google Scholar
33 : Serious adverse events in randomized psychosocial treatment studies: safety or arbitrary edicts? J Consult Clin Psychol 2008; 76:1076–1082Crossref, Medline, Google Scholar
34 : Contingent reinforcement increases cocaine abstinence during outpatient treatment and 1 year of follow-up. J Consult Clin Psychol 2000; 68:64–72Crossref, Medline, Google Scholar
35 : Applying Longitudinal Data Analysis: Modeling Change and Event Occurrence. New York, Oxford University Press, 2003Crossref, Google Scholar
36 : Data replication and reproducibility: again, and again, and again. Introduction. Science 2011; 334:1225Crossref, Medline, Google Scholar
37 : Replications in psychology research: how often do they really occur? Perspect Psychol Sci 2012; 7:537–542Crossref, Medline, Google Scholar
38 : Defining empirically supported therapies. J Consult Clin Psychol 1998; 66:7–18Crossref, Medline, Google Scholar
39 ;
40 : Six-month trial of bupropion with contingency management for cocaine dependence in a methadone-maintained population. Arch Gen Psychiatry 2006; 63:219–228Crossref, Medline, Google Scholar
41 : Low-cost contingency management for treating cocaine- and opioid-abusing methadone patients. J Consult Clin Psychol 2002; 70:398–405Crossref, Medline, Google Scholar
42 : Drug dependence, a chronic medical illness: implications for treatment, insurance, and outcomes evaluation. JAMA 2000; 284:1689–1695Crossref, Medline, Google Scholar
43 : Computer-aided psychotherapy for anxiety disorders: a meta-analytic review. Cogn Behav Ther 2009; 38:66–82Crossref, Medline, Google Scholar
44 : Cost-effectiveness of computer-assisted training in cognitive-behavioral therapy as an adjunct to standard care for addiction. Drug Alcohol Depend 2010; 110:200–207Crossref, Medline, Google Scholar



