Naltrexone Implant for the Treatment of Polydrug Dependence: A Randomized Controlled Trial
Abstract
Objective:
The majority of drug addicts are polydrug dependent, and no effective pharmacological treatment is currently available for them. The authors studied the overall real-world effectiveness of naltrexone implant in this patient population.
Method:
The authors assessed the effectiveness of a naltrexone implant in the treatment of coexisting heroin and amphetamine polydrug dependence in 100 heroin- and amphetamine-dependent outpatients in a 10-week randomized, double-blind, placebo-controlled trial. The main outcome measures were retention in the study, proportion of drug-free urine samples, and improvement score on the Clinical Global Impressions Scale (CGI). Analyses were conducted in an intent-to-treat model.
Results:
At week 10, the retention rate was 52% for patients who received a naltrexone implant and 28% for those who received a placebo implant; the proportions of drug-free urine samples were 38% and 16%, respectively, for the two groups. On the CGI improvement item, 56% of the patients in the naltrexone group showed much or very much improvement, compared with 14% of those in the placebo group (number needed to treat=3).
Conclusions:
Naltrexone implants resulted in higher retention in the study, decreased heroin and amphetamine use, and improved clinical condition for patients, thus providing the first evidence of an effective pharmacological treatment for this type of polydrug dependence.
During the past four decades, the only substantially effective treatment for opioid dependence has been the substitution of another opioid for the initial opioid of abuse (1). This approach aims to reduce harm by replacing intravenous use of heroin with orally administered methadone or buprenorphine. Although such substitution therapy has resulted in a reduction of harm related to illicit drug use, such as crime and the spreading of HIV and hepatitis C (2–4), it has also caused severe problems. For example, in several countries, such as Finland, Georgia, and Mauritius, the vast majority of all opioid-dependent individuals now inject illicitly sold buprenorphine or buprenorphine-naloxone instead of heroin (5–7), which has also led to increased incidences of opioid dependence. Therefore, the misused treatment has occasionally become a bigger problem than the heroin use had been.
Naltrexone is an opioid receptor antagonist that has been used for the treatment of both alcohol and opioid dependence (1, 8–11). However, oral naltrexone has proved ineffective in the treatment of opioid dependence because of poor treatment adherence (1). Five recent randomized controlled trials indicate that naltrexone implant (12–14) and depot injection (15, 16) may be the first effective, nonaddictive pharmacological treatments for heroin dependence in patients who have no other coexisting drug dependence. However, the majority of drug addicts are polydrug dependent (17), and thus the real-world effectiveness of long-acting naltrexone formulations is unknown. Moreover, no effective pharmacological treatment is currently available for polydrug dependence (18). In this patient population, treatment with naltrexone might be useless in reducing drug-related harm if the putative compensatory increase in stimulant use outweighs the decrease in opioid use. Oral naltrexone has been reported to decrease amphetamine use compared with placebo (19) in selected amphetamine-dependent patients. Thus, naltrexone might also be a potential treatment for polydrug dependence, even in real-world settings, if the problem of treatment adherence could be solved. We studied the real-world effectiveness of a naltrexone implant in the treatment of heroin-amphetamine polydrug dependence.
Method
Study Design
The trial was conducted at the St. Petersburg State Pavlov Medical University, Russia, and its affiliated hospital, Leningrad Regional Addiction Hospital. The recruitment of patients began in March 2008, and the study was completed in February 2011. An interim analysis of the first 50 patients was conducted to evaluate the putative harms and benefits of the interventions. Since no harmful effects were observed to be associated with the active treatment, the study was continued as planned. One hundred patients having coexisting amphetamine and opioid dependence (confirmed by a positive urine sample) were randomly assigned, in a 1:1 ratio in a double-blind protocol, to receive a naltrexone depot implant (N=50) or a placebo implant that was identical in appearance (N=50). A sample size of 100 was considered sufficient to reveal significance of an effect size of medium magnitude (20). Randomization was done with a computer-generated random number list prepared by an investigator with no clinical involvement in the trial (E.V.). The study was approved by the Independent Ethical Committee of St. Petersburg State Pavlov Medical University.
Patients
The inclusion criteria were a primary DSM-IV diagnosis of concurrent amphetamine and opioid dependence, present for at least 1 year; age between 18 and 50 years; education level of high school graduate or above; negative urine toxicology and alcohol breath tests; no current use of psychotropic medications; at least one relative willing to participate in the treatment (e.g., to monitor the administration of medications, assist in follow-up, and provide outcome data); a stable address in St. Petersburg or in the nearest districts of Leningrad Region; a home telephone number at which the patient could be reached; willingness and ability to give informed consent and otherwise participate; and, for women of childbearing age, a negative pregnancy test and use of adequate contraception.
The exclusion criteria were clinically significant cognitive impairment, schizophrenia, a paranoid disorder, bipolar disorder, or a seizure disorder; advanced neurological, cardiovascular, renal, or hepatic disease; active tuberculosis; a current febrile illness; an AIDS-defining illness; a significant laboratory abnormality, such as severe anemia, unstable diabetes, or liver function test results greater than three times normal values; pregnancy; pending legal charges with potential impending incarceration; concurrent participation in another treatment study; and concurrent treatment in another substance abuse program.
Procedure
Treatment medication was labeled according to the randomization list, and all individuals involved with the clinical phase of the trial were blind to the intervention. Patients were examined by a psychiatrist at the beginning of the study and at visits throughout treatment. Psychiatrists who were trained in individual drug counseling (E.B., O.M.) enrolled the patients, assigned them to interventions, reviewed their substance use, recovery efforts, functioning, and adverse events, and provided them with psychological support and advice. Patients had to provide an opioid-negative urine sample and undergo a naloxone challenge test, after which they received the surgical naltrexone implant. This sustained-release naltrexone preparation (Prodetoxon) has been approved in the Russian Federation for preventing relapse to opioid dependence. Prodetoxon is a composite subcutaneous implant prepared in a cylinder that is 18 mm long and 8.5 mm in diameter. It contains 1000 mg of naltrexone and blocks opioid effects for 8–10 weeks. Patients gave urine samples (the pH of the urine was measured) once a week, under supervision, for up to 70 days (10 weeks). The cutoff for heroin-free urine was 300 ng/mL of morphine. With this procedure, heroin can be detected for up to 3–4 days after use, which may result in missing occasional heroin use in weekly urine tests. Opioid and amphetamine use was also assessed by self-reported use on the timeline follow-back survey (21). The severity of the addiction at baseline was measured by the Addiction Severity Index (22). Other health assessments included the HIV Risk Assessment Battery (23), visual analogue scales of craving for opioids and amphetamine, the Clinical Global Impressions Scale (CGI), and the Global Assessment of Functioning Scale (GAF). Safety was assessed by weekly monitoring of treatment-emergent adverse events, with vital signs and biochemistry and hematology of urine and blood samples, which included liver function tests. Adverse events were assessed through open questions during the weekly visits. At week 10, participants' relatives were contacted by telephone to investigate outcomes (including mortality) among patients who dropped out.
Outcomes
The primary outcomes assessed were retention in the study, proportion of urine samples that were free of both amphetamine and opioids during the treatment (missing samples were considered positive for both drug classes), and improvement on the CGI during treatment.
The secondary outcomes assessed were proportion of opioid-free urine samples during treatment (missing samples were considered opioid positive), proportion of amphetamine-free urine samples during the treatment (missing samples were considered amphetamine positive), GAF score, number of days per week that amphetamine was used during treatment, craving for opioids and amphetamine, and adverse events.
The study protocol was updated on December 22, 2009, for several reasons. Because of new legislation in Russia prohibiting the export of any biological samples to Finland, the quantitative amphetamine analyses could not be done in the laboratory of the National Public Health Institute, Helsinki. Also, funding was not sufficient for us to perform naloxone challenge tests to evaluate opioid dependence. Under these circumstances, we decided to use conventional urine tests to measure opioid and amphetamine use (our primary outcome measure). The updated protocol also included the addition of retention in the study and CGI improvement score as primary outcome measures (retention in the study and the patients' general well-being are considered the most important indicators of the effectiveness of the treatment in drug addiction trials). For the secondary outcomes, the update added adverse events and excluded cannabis and benzodiazepine use, since it had become evident that their use was not sufficiently common in the study population. The original sponsor, the National Research and Development Centre for Welfare and Health (Finland), merged with the National Public Health Institute on January 1, 2009, and the organization became the National Institute for Health and Welfare; thus, the name of the sponsor changed in the update. Finally, the start and end dates were delayed from the anticipated dates.
Statistical Analysis
The results were analyzed in an intent-to-treat model in which missing urine samples were classified as drug positive. Categorical variables were analyzed with the chi-square test or Fisher's exact test and continuous variables with the t test or Mann-Whitney U test, depending on the validity of distributional assumptions. Data management and analyses were conducted with SPSS, version 17.0 (SPSS, Inc., Chicago), and StatCalc (www.acastat.com). For patients lost to follow-up, the change in the CGI improvement score was defined as the change between baseline (week 0) and the last available observation.
Results
The CONSORT flow diagram of the study is presented in Figure S1 in the online data supplement that accompanies the online edition of this article. The main baseline clinical measures are listed in Table 1; no statistically significant differences were observed between the two treatment groups. Most patients were men; the naltrexone arm included four women (8%), and the placebo arm included seven (14%). HIV status was available for 86 patients; in the placebo arm, 77% (34/44) were HIV positive, and in the naltrexone arm, 48% (20/42) were HIV positive (χ2=8.09, df=1, p=0.004). Fifteen patients (30%) in the naltrexone group used marijuana, and 13 (26%) in the placebo group did so. The use of sedatives was rare in this sample (none in the naltrexone arm, and one in the placebo arm). The mean consumption of alcohol was only 7.5 g/day (SD=9.9) for the total study population, and therefore the putative reduction was not studied.
| Placebo (N=50) | Naltrexone (N=50) | |||
|---|---|---|---|---|
| Characteristic | Mean | SD | Mean | SD |
| Age (years) | 29.3 | 4.38 | 28.0 | 4.10 |
| Duration of heroin addiction (years) | 8.7 | 2.83 | 8.2 | 3.75 |
| Duration of amphetamine addiction (years) | 5.6 | 2.62 | 5.6 | 3.11 |
| Amphetamine use (days per month) | 24.3 | 14.35 | 27.4 | 13.50 |
| Heroin useb (g/day) | 1.0 | 0.64 | 0.9 | 0.49 |
| Alcoholb (g/day) | 6.8 | 10.18 | 8.2 | 10.11 |
| Craving for heroinc | 39.7 | 32.17 | 44.2 | 34.08 |
| Craving for amphetaminec | 45.0 | 28.77 | 47.5 | 31.39 |
| Addiction Severity Index | ||||
| Medical status | 0.09 | 0.085 | 0.11 | 0.085 |
| Work | 0.81 | 0.23 | 0.82 | 0.25 |
| Opiates | 0.24 | 0.085 | 0.24 | 0.091 |
| Amphetamine | 0.19 | 0.11 | 0.18 | 0.091 |
| Legal status | 0.06 | 0.078 | 0.07 | 0.071 |
| Family | 0.25 | 0.18 | 0.25 | 0.16 |
| Drug HIV risk behaviord | 9.14 | 3.73 | 10.34 | 4.48 |
| Sexual HIV risk behaviord | 5.22 | 2.72 | 5.76 | 2.92 |
| Global Assessment of Functioning Scale score | 66.4 | 7.92 | 67.8 | 7.64 |
| Alanine aminotransferase (ALT) (U/L) | 39.9 | 23.54 | 34.2 | 20.79 |
| Aspartate aminotransferase (AST) (U/L) | 57.0 | 29.76 | 50.0 | 17.39 |
TABLE 1. Baseline Characteristics of Opioid-Amphetamine Polydrug-Dependent Patients Treated With Naltrexone or Placebo Implanta
Primary Outcome Measures
Retention in the study is illustrated in Figure 1. At week 10, the retention rate was 52% (N=26) for the naltrexone group and 28% (N=14) for the placebo group (χ2=6.00, df=1, p=0.01). The proportion of drug-free urine samples was 38% (N=19) in the naltrexone group and 16% (N=8) in the placebo group (χ2=6.14, df=1, p=0.01). The changes in the CGI improvement score indicating the difference in treatment effect are summarized in Table 2. The naltrexone arm showed a substantially greater treatment effect than the placebo arm, with 56% of naltrexone patients showing much or very much improvement according to the CGI, compared with only 14% of the placebo patients (χ2=19.4, df=1, p<0.001; number needed to treat=3, 95% CI=2–4).
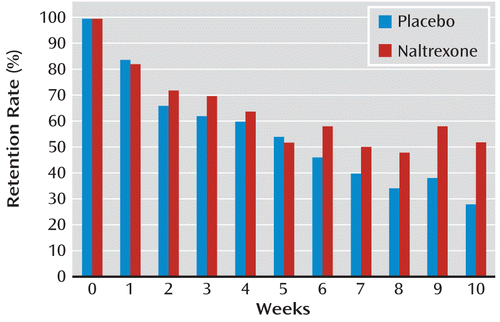
FIGURE 1. Study Retention Among Opioid-Amphetamine Polydrug-Dependent Patients Treated With Naltrexone or Placebo Implant During the 10-Week Treatment Perioda
a At week 10, retention was 52% (26/50) for patients in the naltrexone group, compared with 28% (14/50) for patients in the placebo group (significantly different at p=0.01). Since patients were permitted to continue in the trial despite missing previous visits, the retention rate increased at weeks 6 and 9, when patients who missed visits the previous week resumed participation.
| Placebo (N=50) | Naltrexone (N=50) | |||
|---|---|---|---|---|
| Rating | N | % | N | % |
| Much improved | 7 | 14 | 28 | 56 |
| Moderately improved | 11 | 22 | 6 | 12 |
| Minimally improved | 8 | 16 | 6 | 12 |
| No change | 24 | 48 | 10 | 20 |
TABLE 2. Change From Baseline in Clinical Global Impression Scale Improvement Score in Opioid-Amphetamine Polydrug-Dependent Patients Treated With Naltrexone or Placebo Implanta
Secondary Outcome Measures
At week 10, patients in the naltrexone group had significantly more heroin-free urine samples (52% compared with 20%; χ2=11.1, df=1, p<0.001) and more amphetamine-free urine samples, although the difference fell short of significance (40% compared with 24%; χ2=2.94, df=1, p=0.09). In the weekly urine analyses, a statistically significant difference in heroin-free samples was also observed at week 6 (χ2=8.1, df=1, p=0.005), at week 8 (χ2=4.3, df=1, p=0.04), and at week 9 (χ2=4.2, df=1, p=0.04), with patients in the naltrexone arm having more heroin-free samples. No statistically significant differences were observed in amphetamine-free urine samples. At week 10, the mean number of amphetamine use incidents (times/week) was 4.5 times in the naltrexone group and 5.7 times in the placebo group (Mann-Whitney U test=1030.5, p=0.06). The rating of subjective effects of amphetamine was available for 18 patients in the placebo group and 22 patients in the naltrexone group. Fifteen patients in the placebo group (83.3%) and three in the naltrexone group (13.6%) reported full effect for amphetamine use, indicating that naltrexone suppressed the euphoric effect more than did placebo (p<0.001, Fisher's exact test). The mean GAF scores at week 10 were 82.0 for the naltrexone group (N=20) and 71.9 for the placebo group (N=28) (Mann-Whitney U test=145.5, p=0.004), indicating a better outcome among patients receiving naltrexone.
Craving for opioids or amphetamine, as well as HIV-drug and HIV-sex risk behaviors, decreased in both groups over the study period (Figure 2). However, no significant differences in craving, for either opioids or amphetamine, were observed between the groups.
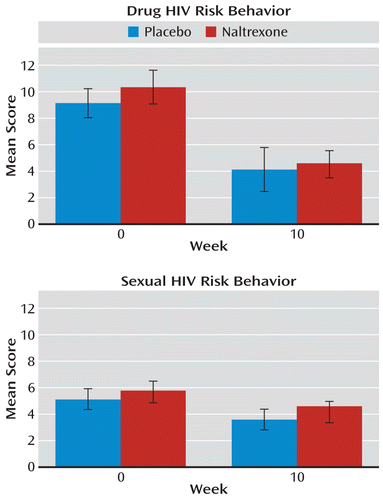
FIGURE 2. Drug and Sexual HIV Risk Behavior
Adverse Events
Adverse events are listed in Table 3. No severe adverse events were reported, and no significant differences were observed between groups. No significant differences were seen between groups in change in the alanine aminotransferase (ALT) level from baseline to week 10 (from 39.9 U/L to 36.2 U/L for the placebo group compared with 34.2 U/L to 30.3 U/L for naltrexone group; reference range, 10–45 U/L for females and 10–70 U/L for males), but the aspartate aminotransferase (AST) level decreased in the naltrexone group (N=13) and increased in the placebo group (N=26) (from 50.0 U/L to 48.7 U/L in the naltrexone group and from 57.0 U/L to 65.0 U/L in the placebo group; reference range, 10–35 U/L for females and 10–45 U/L for males; difference between groups, Mann-Whitney U test=92, p=0.02). All patients or their relatives were contacted by telephone at the end of the study. All patients in the study were alive at week 10.
| Event | Placebo (N=50) | Naltrexone (N=50) |
|---|---|---|
| Surgical implantation | 0 | 2 |
| Diarrhea | 0 | 3 |
| Nervousness | 1 | 0 |
| Insomnia | 3 | 3 |
| Fatigue | 1 | 1 |
| Irritability, nervousness | 2 | 2 |
| Dry mouth | 1 | 0 |
| Loss of appetite | 1 | 2 |
TABLE 3. Adverse Events in Opioid-Amphetamine Polydrug-Dependent Patients Treated With Naltrexone or Placebo Implanta
Discussion
Our results show that relative to placebo, the naltrexone implant resulted in higher retention in the study, decreased heroin and amphetamine use, and improved clinical condition of patients, thus providing the first evidence of an effective pharmacological treatment for this type of polydrug dependence. Because the majority of drug-dependent patients use more than one drug (17), treatment of only one dependence, such as intravenous heroin use by oral methadone or buprenorphine, would not be sufficient for injection-related harm reduction if the patient continued to inject other drugs, such as amphetamine. Since long-acting naltrexone effectively decreases opioid use, it might lead to compensatory increases in the use of nonopioid drugs, such as amphetamine, among polydrug-dependent patients, resulting in zero net benefit. However, our results indicate that this is not the case. The effectiveness of polydrug dependence treatment with naltrexone implants or depot injections should be studied and confirmed in other patient populations who use combinations of heroin, buprenorphine, amphetamine, and cocaine. Preliminary evidence from a study by Comer et al. (15) suggests that naltrexone depot formulations might have a beneficial effect on cocaine abuse and even on cannabis and benzodiazepine abuse. This suggests that the opioidergic system may be the common pathway for the effects of all these drugs of abuse. A recent meta-analysis that included 10 randomized controlled trials comparing oral naltrexone and placebo detected no beneficial effect on retention or relapse rates for opioid-dependent patients (24). However, a significant treatment effect was observed in a Swedish study (19) that compared oral naltrexone and placebo in the treatment of amphetamine dependence in selected and highly motivated patients (more than 70% of the assessed individuals were excluded from the study). In the present study, our sample was a typical treatment-seeking patient population (only 16% of assessed individuals were excluded), which suggests that our results reflect the real-world effectiveness of the naltrexone implant treatment. The duration of our trial was 10 weeks, which is a short period when considering the chronic nature of concurrent opioid and amphetamine dependence. It is likely that in clinical practice, patients should be treated with several successive implants in 2- to 3-month intervals to achieve long-term recovery from dependence.
The naltrexone implant was generally well tolerated. It was not associated with increased levels of ALT or AST, and it was actually associated with a reduction in AST levels compared with placebo. Two patients (4%) experienced mild surgical side effects. The implant used in this study results in naltrexone serum levels of around 2 ng/mL for 10 weeks, which is somewhat higher than levels provided by the currently available depot injection (Vivitrol) during 4-week injection intervals (25). Vivitrol has been shown to be effective for the treatment of heroin dependence, and on the basis of the results of our previous trial (16), it was recently approved by the U.S. Food and Drug Administration for the treatment of opioid dependence. However, whether it is also effective for the treatment of amphetamine dependence is unknown.
It has been suspected that oral naltrexone treatment could lead to an increased risk of death due to accidental overdose (26). However, a large follow-up study (27) that included all patients in Western Australia starting methadone (N=553) or naltrexone implant (N=341) found that naltrexone implant was associated with a slightly lower age-standardized mortality rate ratio compared with methadone (0.65, 95% CI=0.12–1.17). This suggests that while oral naltrexone may be ineffective in treating opioid dependence, because of low treatment adherence and the increased risk of concomitant opioid overdose, a naltrexone implant is at least as safe as methadone. In our study, no deaths were reported in the survey of all patients at the end of the study.
1. : A review of opioid dependence treatment: pharmacological and psychosocial interventions to treat opioid addiction. Clin Psychol Rev 2010; 30:155–166Crossref, Medline, Google Scholar
2. : Evidence-based treatment of opioid-dependent patients. Can J Psychiatry 2006; 51:635–646Crossref, Medline, Google Scholar
3. : Diacetylmorphine versus methadone for the treatment of opioid addiction. N Engl J Med 2009; 361:777–786Crossref, Medline, Google Scholar
4. : A comparison of levomethadyl acetate, buprenorphine, and methadone for opioid dependence. N Engl J Med 2000; 343:1290–1297Crossref, Medline, Google Scholar
5. : Why do the clients of Georgian needle exchange programmes inject buprenorphine? Eur Addict Res 2010; 16:1–8Crossref, Medline, Google Scholar
6. : Bioavailability of buprenorphine from crushed and whole buprenorphine (Subutex) tablets. Eur Addict Res 2010; 16:85–90Crossref, Medline, Google Scholar
7. Mauritian delegation lies to UN about drugs problem. Mauritius News, June 11, 2010. http://weluvmu.wordpress.com/2010/06/11/mauritian-delegation-lies-to-un-about-drugs-problem/Google Scholar
8.
9. : Opioid antagonists for alcohol dependence. Cochrane Database Syst Rev 2010; 12:CD001867Medline, Google Scholar
10. : Intramuscular extended-release naltrexone: current evidence. Ann NY Acad Sci 2011; 1216:144–166Crossref, Medline, Google Scholar
11.
12. : Improving clinical outcomes in treating heroin dependence: randomized controlled trial of oral or implant naltrexone. Arch Gen Psychiatry 2009; 66:1108–1115Crossref, Medline, Google Scholar
13. : Naltrexone implants after in-patient treatment for opioid dependence: randomised controlled trial. Br J Psychiatry 2009; 194:541–546Crossref, Medline, Google Scholar
14. : Use of naltrexone to treat opioid addiction in a country in which methadone and buprenorphine are not available. Curr Psychiatry Rep 2010; 12:448–453Crossref, Medline, Google Scholar
15. : Injectable, sustained-release naltrexone for the treatment of opioid dependence: a randomized, placebo-controlled trial. Arch Gen Psychiatry 2006; 63:210–218Crossref, Medline, Google Scholar
16. : Injectable extended-release naltrexone for opioid dependence: a double-blind, placebo-controlled, multicentre randomised trial. Lancet 2011; 377:1506–1513Crossref, Medline, Google Scholar
17.
18. : Pharmacotherapy of dual substance abuse and dependence. CNS Drugs 2007; 21:213–237Crossref, Medline, Google Scholar
19. : Naltrexone for the treatment of amphetamine dependence: a randomized, placebo-controlled trial. Am J Psychiatry 2008; 165:1442–1448Link, Google Scholar
20. : Statistical Power Analysis for the Behavioral Sciences, 2nd ed. Hillsdale, NJ, Lawrence Erlbaum Associates, 1988Google Scholar
21. : Timeline follow-back: a technique for assessing self-reported alcohol consumption, in Measuring Alcohol Consumption: Psychosocial and Biological Methods. Edited by Litten RZAllen JP. Totawa, NJ, Humana Press, 1992, pp 41–72Crossref, Google Scholar
22. : An improved diagnostic evaluation instrument for substance patients: the Addiction Severity Index. J Nerv Ment Dis 1980; 168:26–33Crossref, Medline, Google Scholar
23. : Preparations for AIDS vaccine trials: an automated version of the Risk Assessment Battery (RAB): enchancing the assessment of risk behaviors. ADIS Res Hum Retroviruses 1994; 10(suppl 2):S281–S283Medline, Google Scholar
24. : Oral naltrexone maintenance treatment for opioid dependence. Cochrane Database Syst Rev 2011; 4:CD001333Medline, Google Scholar
25. : Long-acting depot formulations of naltrexone for heroin dependence: a review. Curr Opin Psychiatry 2010; 23:210–214Crossref, Medline, Google Scholar
26.
27. : Mortality in heroin users 3 years after naltrexone implant or methadone maintenance treatment. J Subst Abuse Treat 2008; 35:116–124Crossref, Medline, Google Scholar



