Distinguishing the Effects of Lead-Time Bias and Duration of Untreated Psychosis
To The Editor: In the April issue of this journal, O’Keeffe and colleagues (1) investigated the association between duration of untreated psychosis (DUP) and long-term outcomes in an epidemiological, prospective study of first episode psychosis. It has long been believed that decreasing DUP improves illness course for those with schizophrenia, a theory with important clinical implications. However, in a similar epidemiological cohort with a first hospitalization for psychosis, we showed that the long-term effects of DUP were explained by lead-time bias (2). In other words, differences in outcome were attributable to time that elapsed since illness onset rather than DUP itself.
With this as context, we were grateful to see O’Keeffe et al. test these findings in a distinct, but methodologically similar, cohort. Although their results suggested that a shorter DUP does predict better long-term outcomes, there are two differences between the analyses that compromise the comparison to our findings.
The first is that the analyses do not control for lead-time bias. To test the hypothesis in question and distinguish the effect of DUP from duration of illness requires that each participant’s trajectory begin at psychosis onset, rather than study baseline.
Second, the effect of DUP on outcomes has generally been considered specific to schizophrenia. Prior meta-analyses (3), and prior analyses within the iHOPE cohort (4), have removed those with affective psychosis, because they have shorter DUPs and better prognoses. In the Suffolk County cohort, the mean DUP among those with schizophrenia is more than twice that of affective psychoses, and Global Assessment of Functioning Scale results are more than 10 points lower (Figure 1), such that DUP is a significant predictor of illness course when the two groups are analyzed together (β=−0.09 [SD=0.03]; t=-3.54, p<0.05). A clear test of the hypothesis requires constraining the sample to those with schizophrenia/schizophreniform disorder.
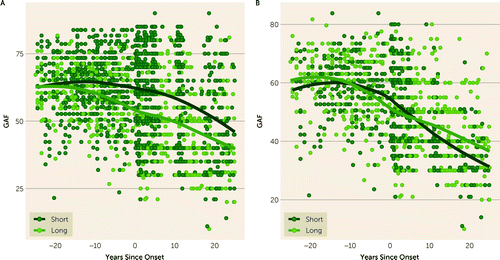
FIGURE 1. The association between DUP (dichotomized via a median split) and psychosocial function when affective psychoses are included (panel A), and excluded (panel B).
In many ways the iHOPE cohort and the Suffolk County cohort are well-matched, and this has the potential for a rigorous test of our findings. However, these two significant confounds must be addressed for results to be comparable.
1. : 20-year prospective, sequential follow-up study of heterogeneity in associations of duration of untreated psychosis with symptoms, functioning, and quality of life following first-episode psychosis. Am J Psychiatry 2022; 179:288–297Link, Google Scholar
2. : Lead-time bias confounds association between duration of untreated psychosis and illness course in schizophrenia. Am J Psychiatry 2020; 177:327–334Link, Google Scholar
3. : Duration of untreated psychosis as predictor of long-term outcome in schizophrenia: systematic review and meta-analysis. Br J Psychiatry 2014; 205:88–94Crossref, Medline, Google Scholar
4. : Prospective relationship of duration of untreated psychosis to psychopathology and functional outcome over 12 years. Schizophr Res 2012; 141:215–221Crossref, Medline, Google Scholar



